 |
 |
 |
 |
 |
|
 |
 |
 |
|||
 |
 |
 |
 |
||
 |
 |
 |
|||
Seeking Perfect Solution to A Tough Anterior Case
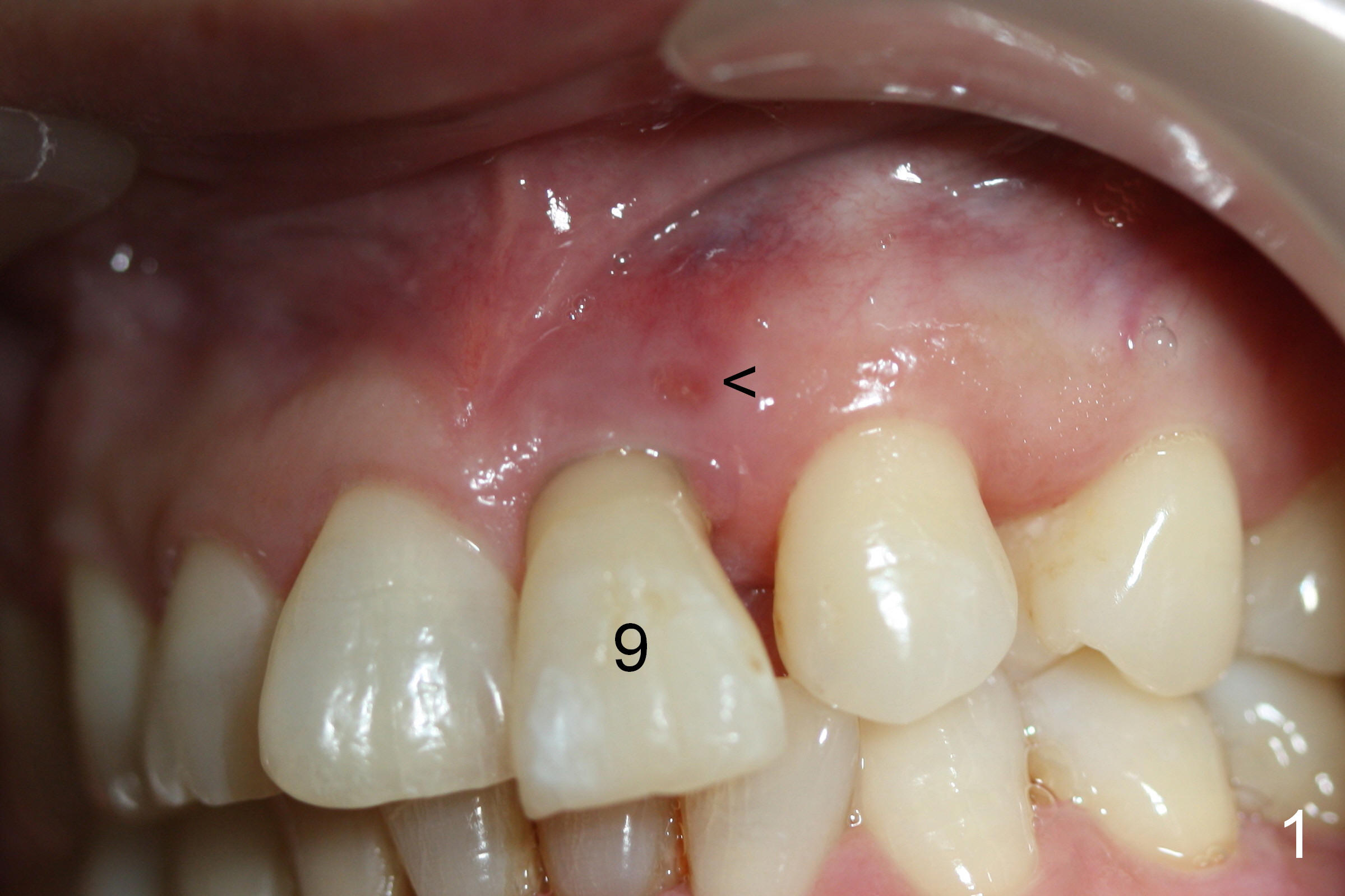
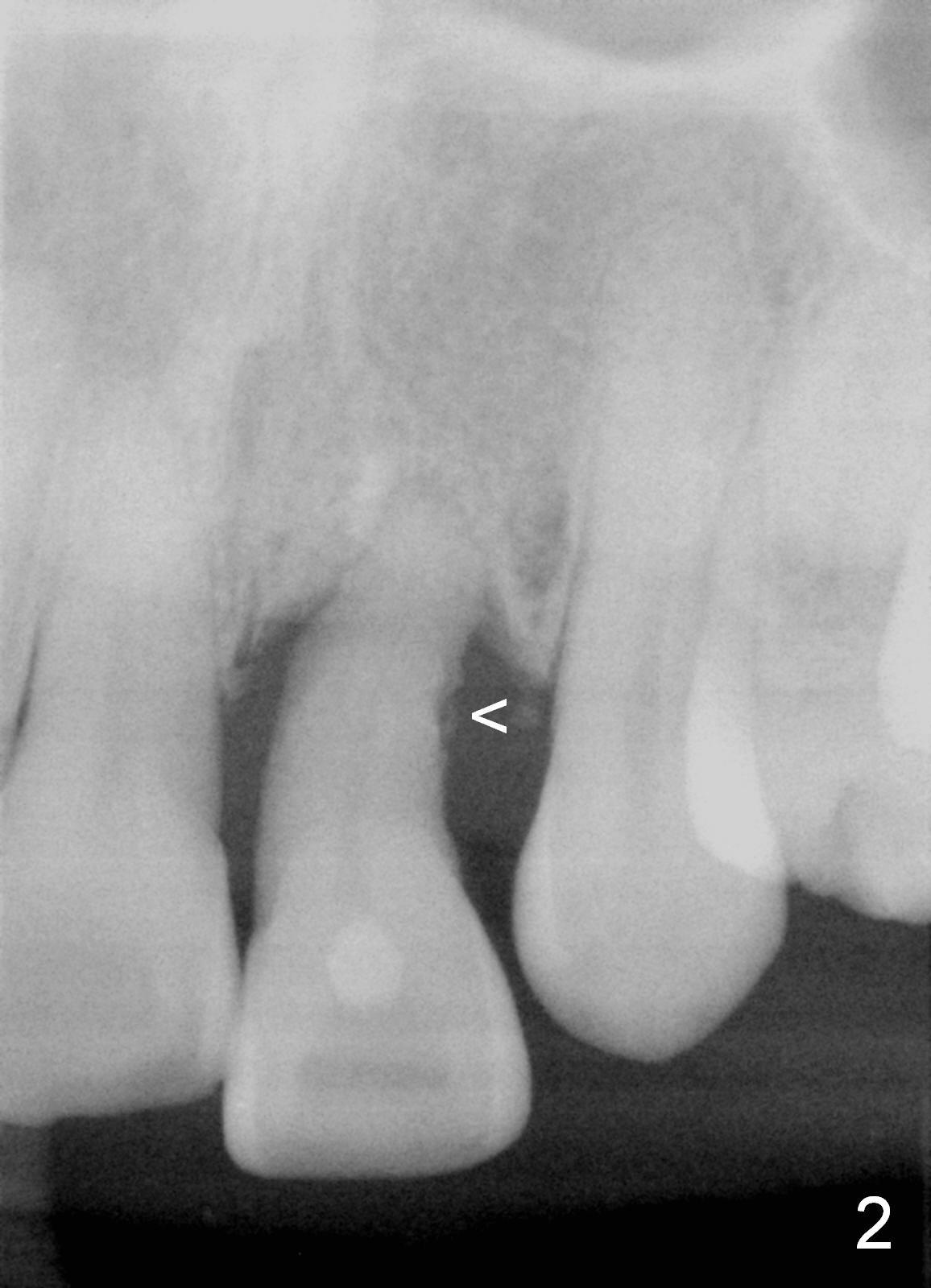
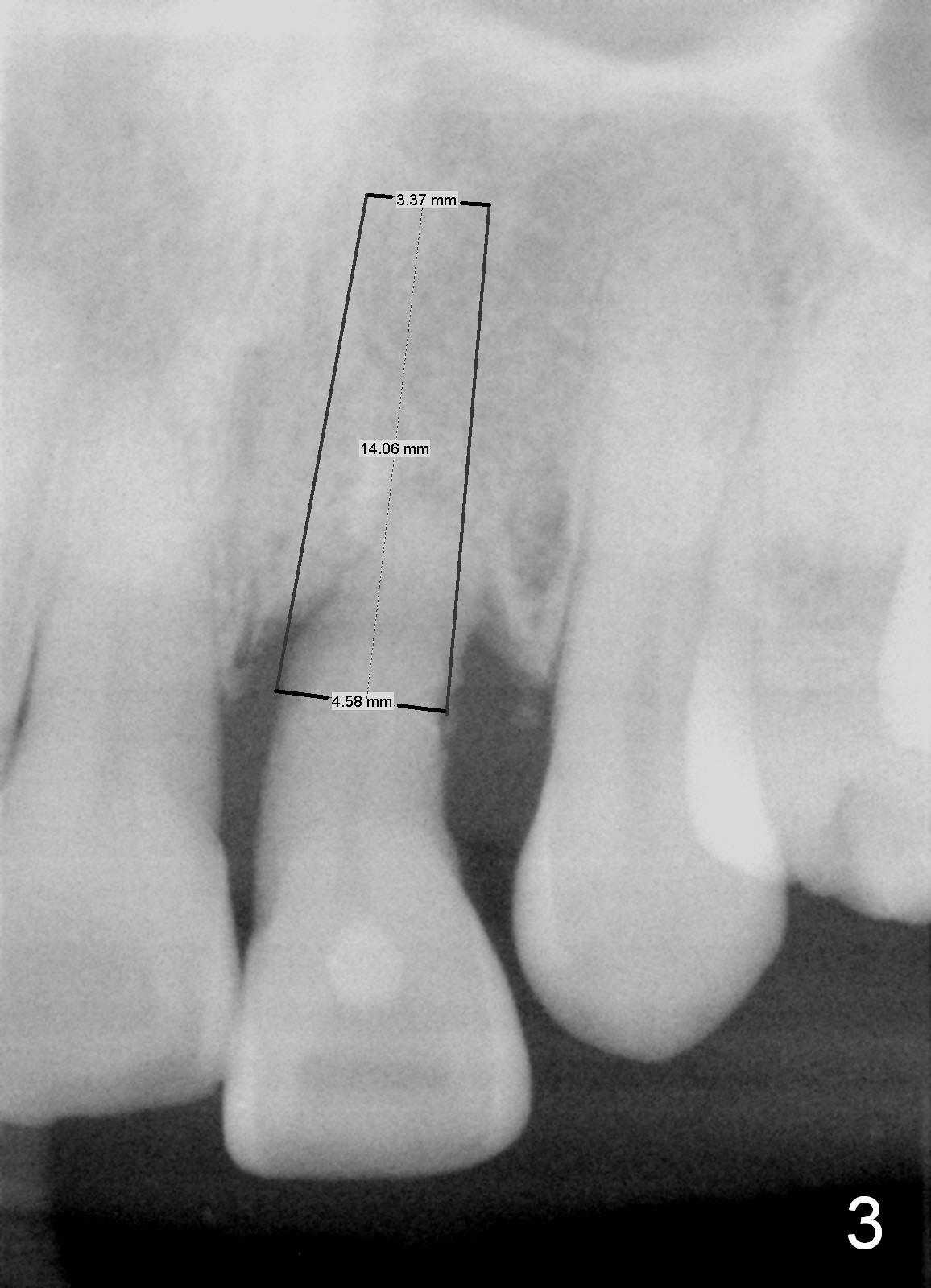
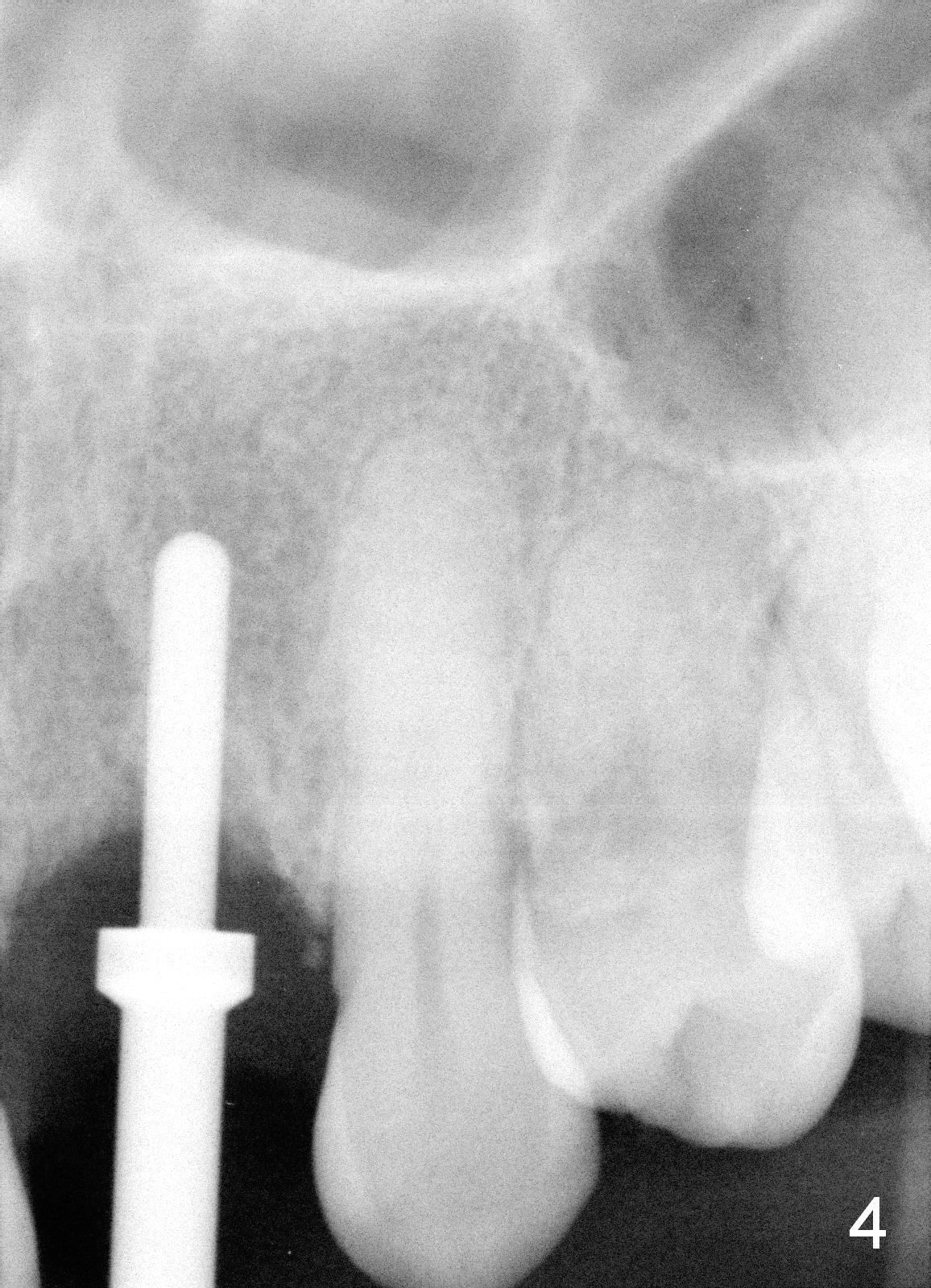
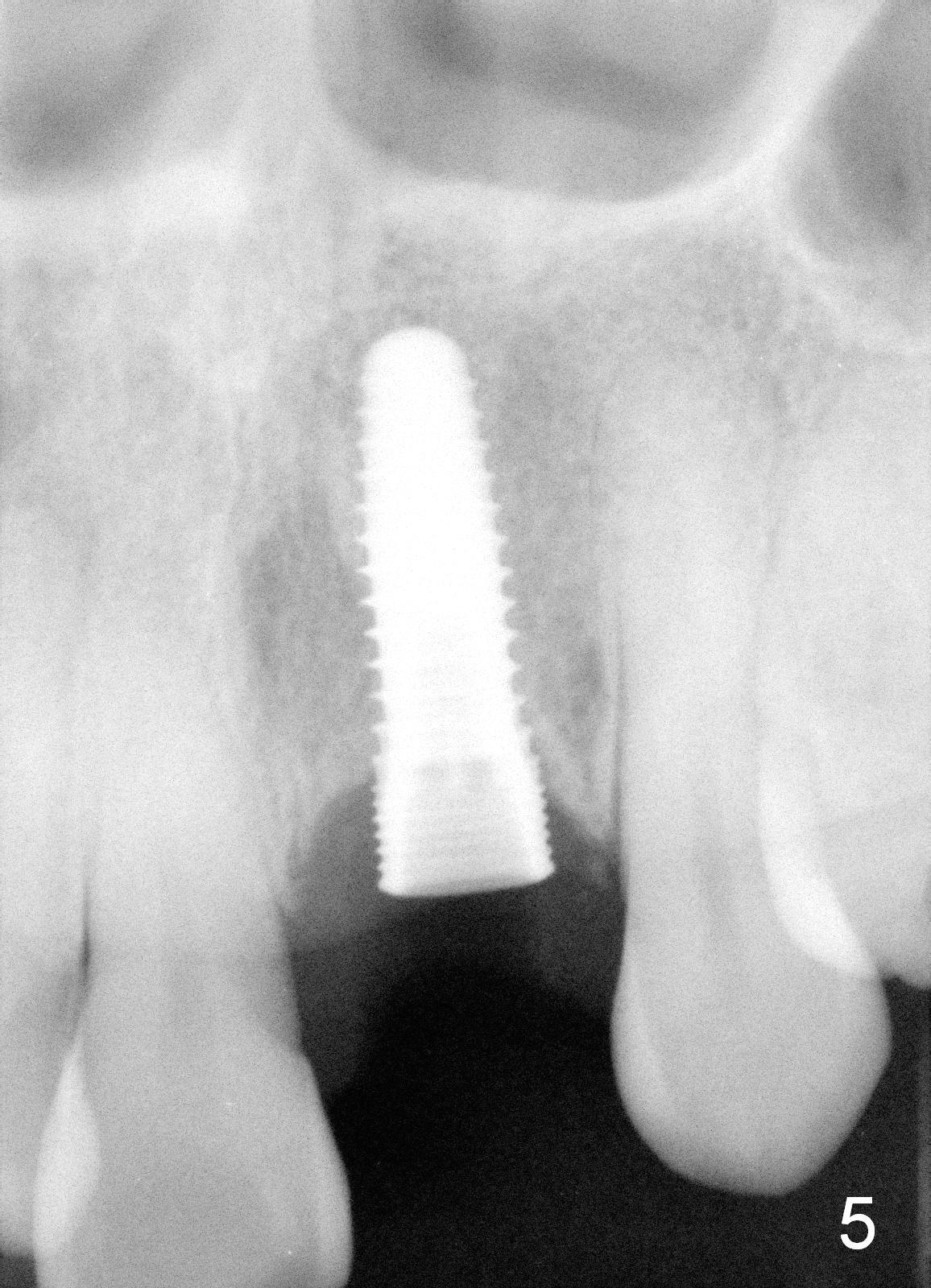
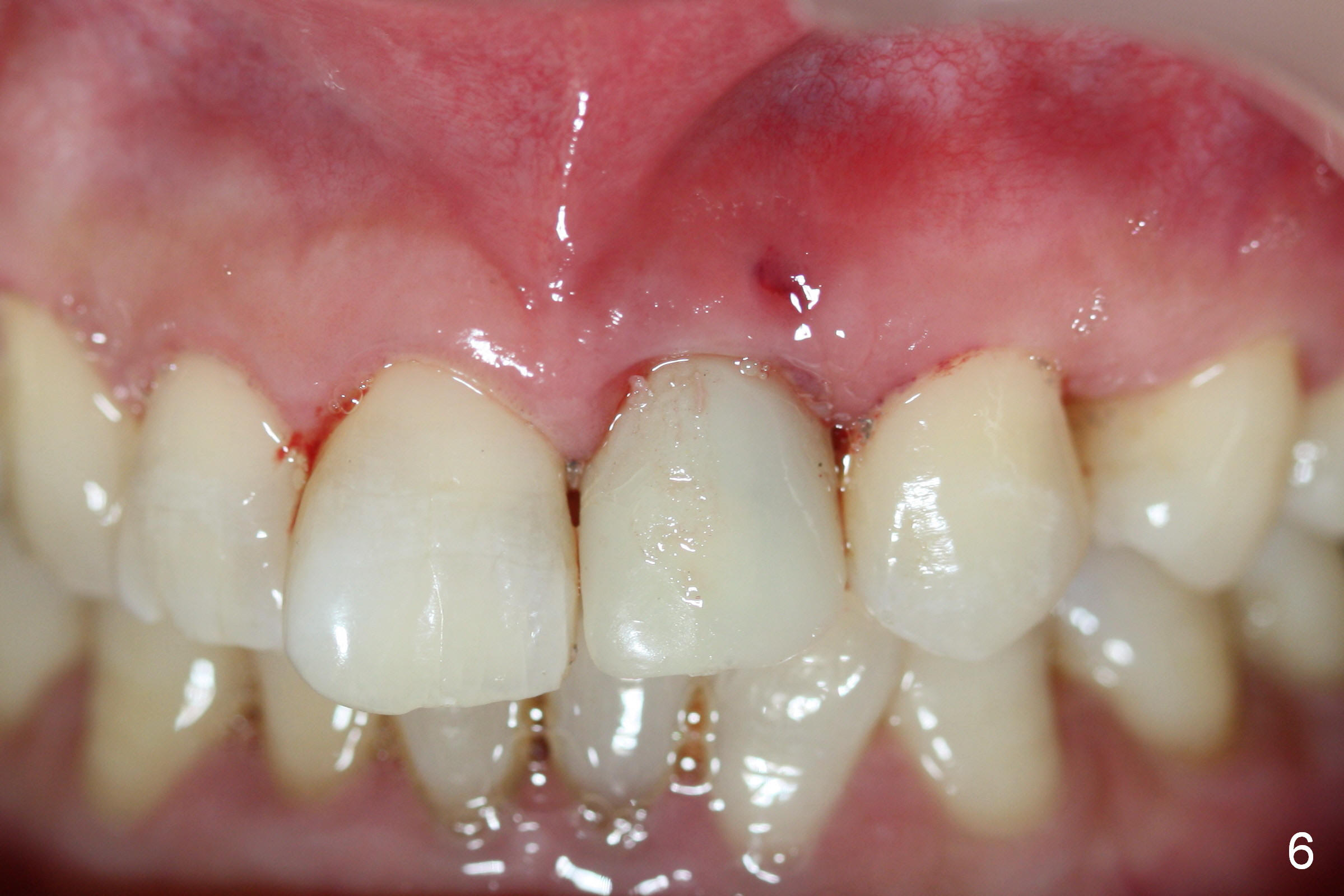
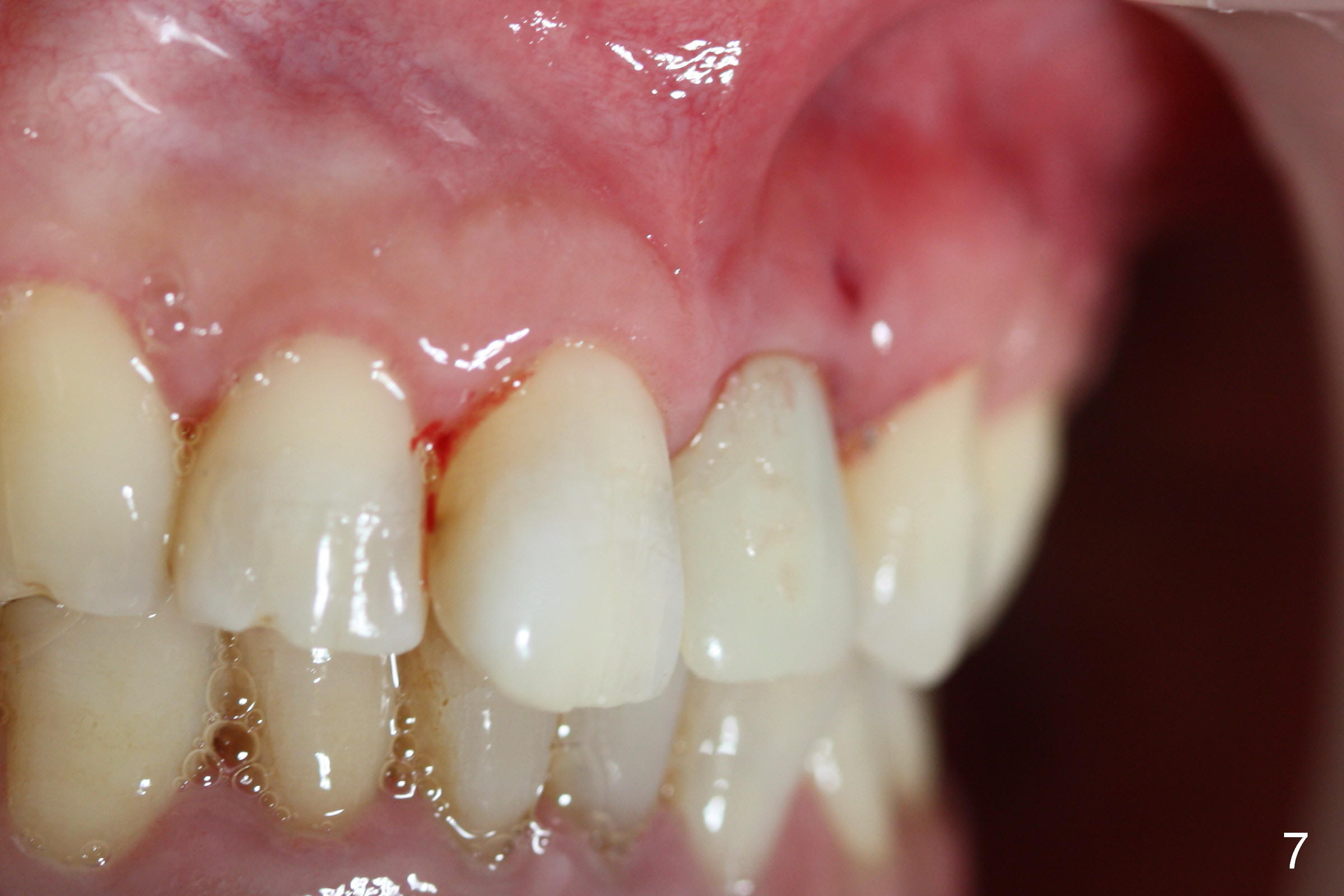
A 52-year-old lady is a dental phobic. The upper left central incisor with a fistula (Fig.1 <) is displaced, probably due to severe bone loss (Fig.2). A 4.5x14 mm bone-level implant appears to be a proper root replacement (Fig.3). After extraction, exploration reveals that both the buccal and lingual plates are lost coronally. Mid buccal and lingual crest is 5 mm from the gingival margin. Osteotomy is initiated in the lingual aspect of the shallow socket with a 2 mm pilot drill 14 mm from the gingival margin. The bone density feels low. A parallel pin is inserted (Fig.4). Then the osteotomy extends to 18 mm, followed by a 3.8 mm tapered drill at 16 mm and 4.1 at 14 mm. A 4.5x14 mm implant is placed with insertion torque >60 Ncm (Fig.5). The implant remains lingual, whereas there is an approximate 3 mm buccal gap, which is bone grafted. A 4.8x10 mm temporary abutment is placed; the length adjusted. An immediate provisional is fabricated with normal morphology and trajectory (Fig.6,7).
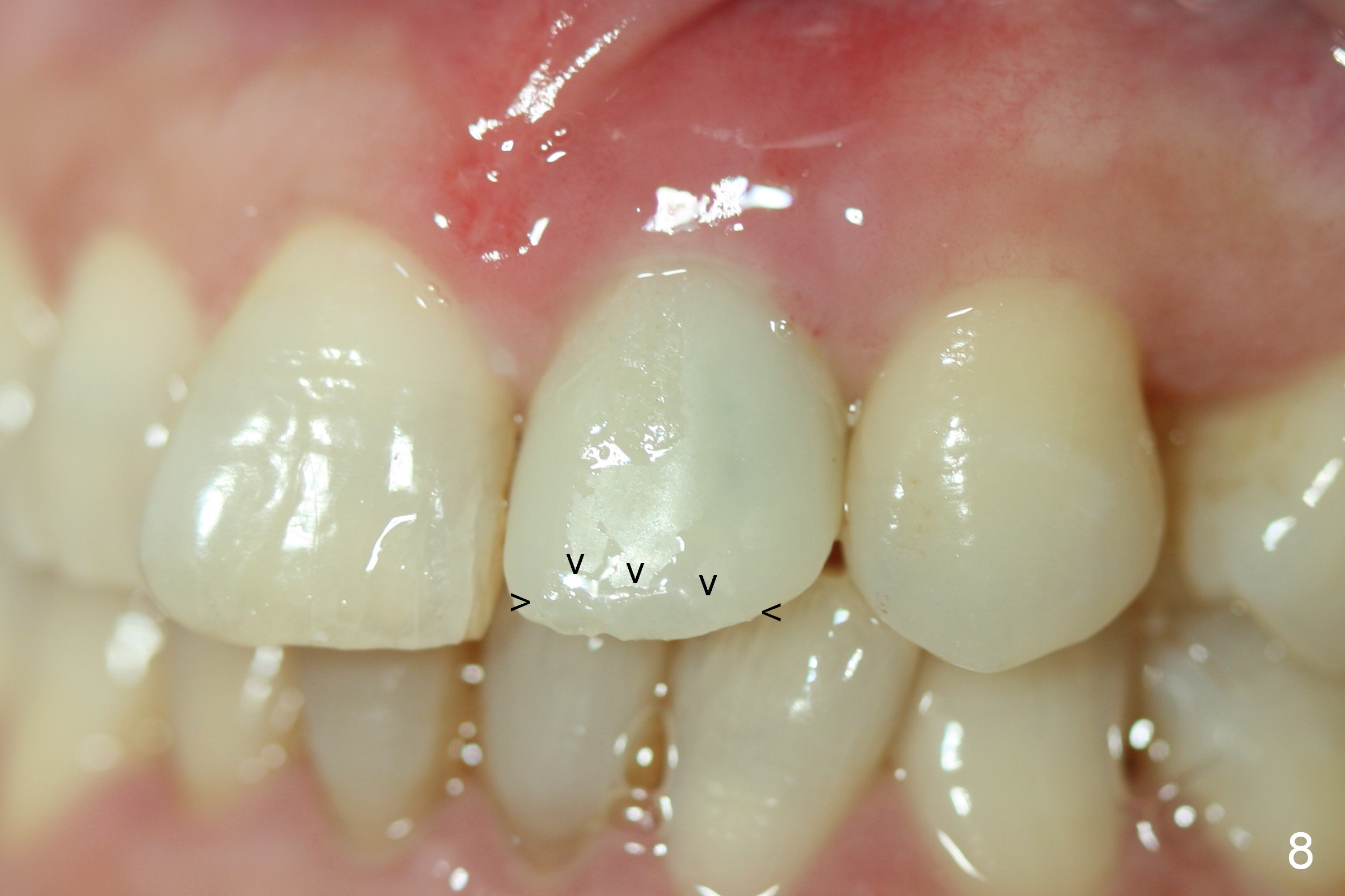
The patient returns 6 days postop asymptomatic. The provisional is loose. After extending access labially, the temporary abutment screw is retightened. The access is repaired with composite (Fig.8 arrowheads). The fistula has reduced, but not disappeared, as compared to Fig.1,6,7.
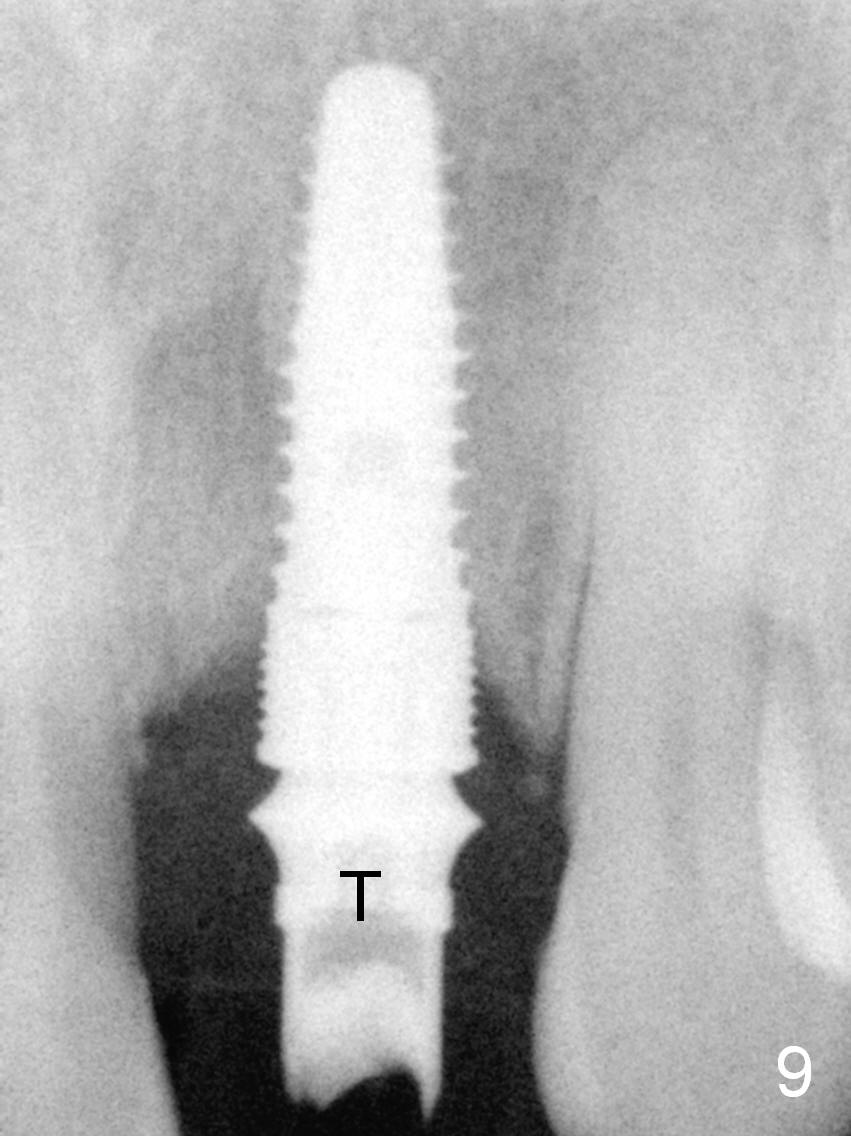
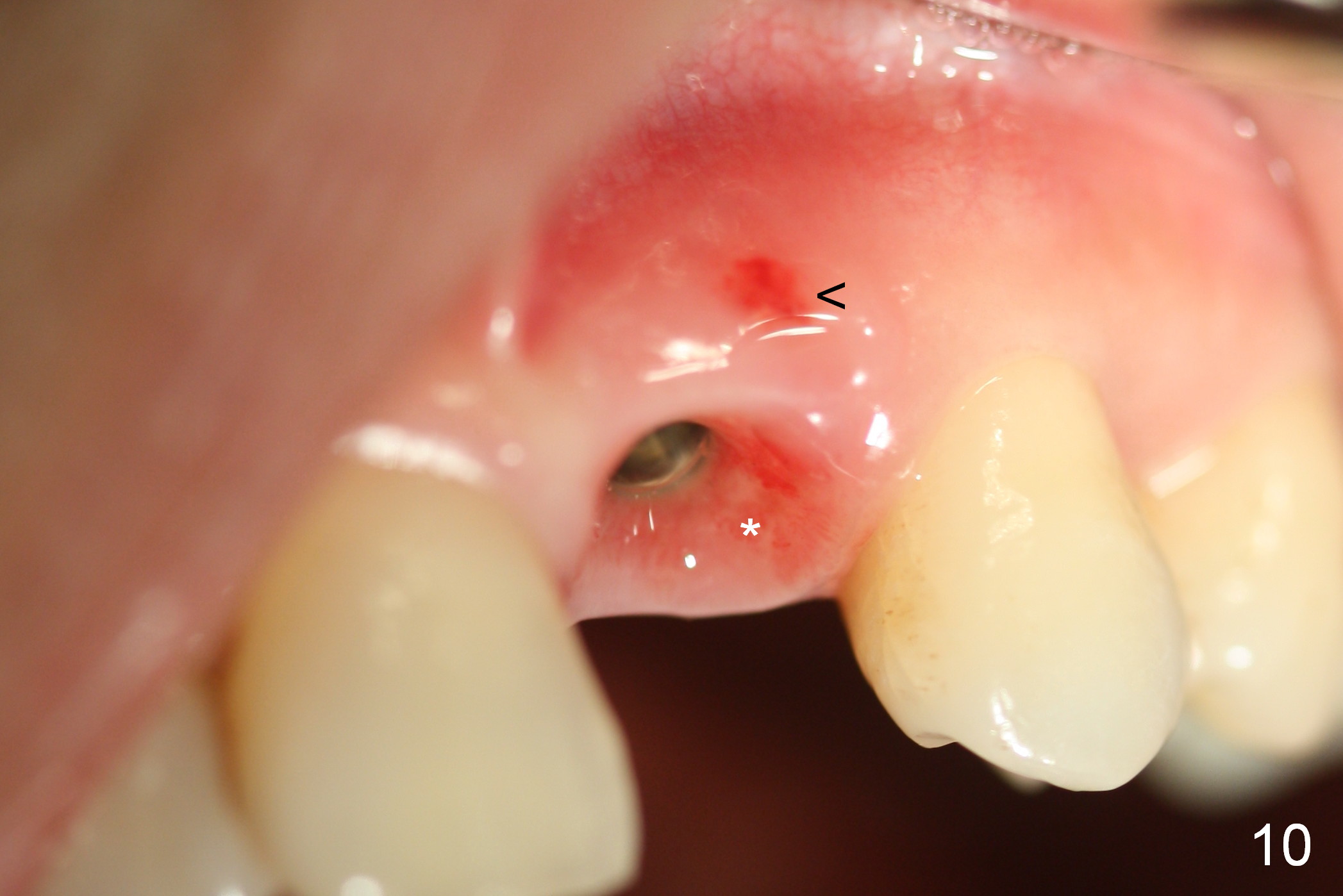
The composite dislodges from the incisal edge 2 months postop. The patient is concerned about the shrinking fistula (Fig.10 <). After taking follow-up PA (Fig.9), the temporary abutment (Fig.9 T) is removed (Fig.10). The fistula is found to have no connection with the tissue (*) contacting the temporary abutment. The latter is retightened. The incisal edge defect is repaired with acrylic. The ease of breakdown of the incisal edge may be related to abnormal occlusal scheme (traumatic occlusion), which may be the reason that the tooth had severe bone loss (Fig.1,2).
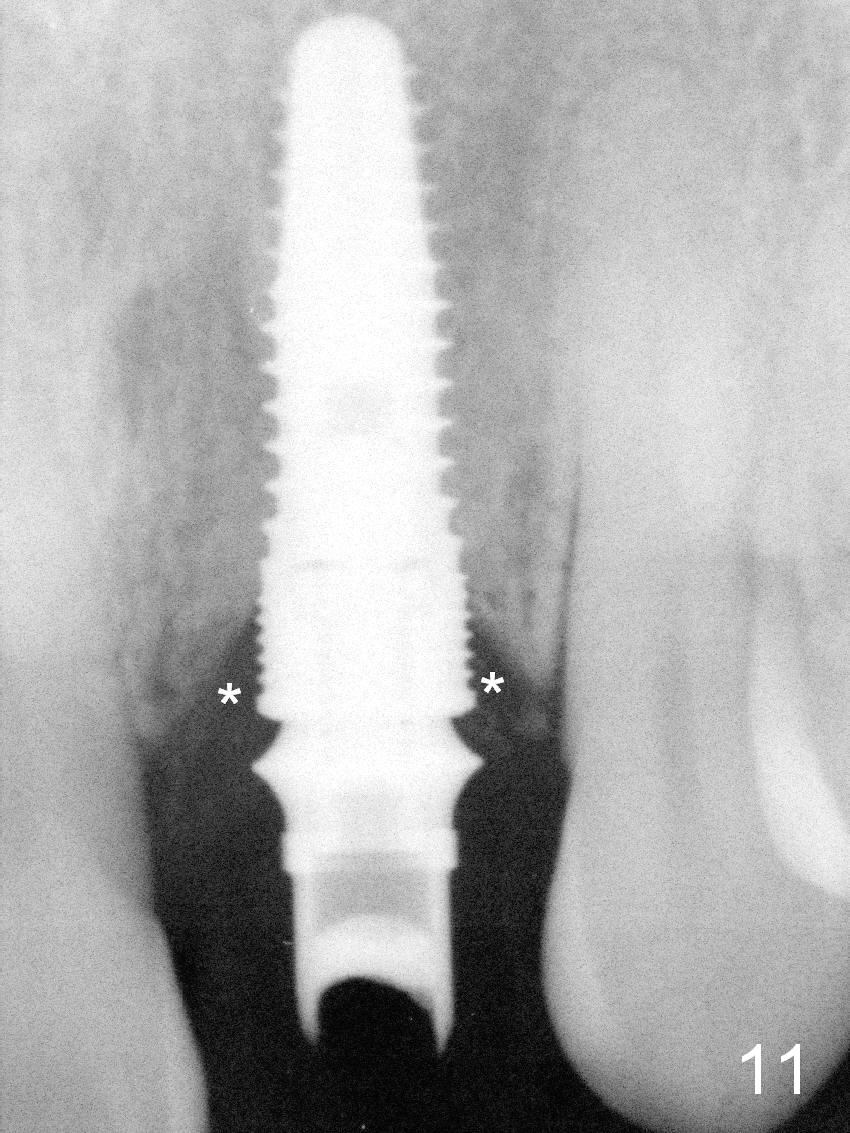
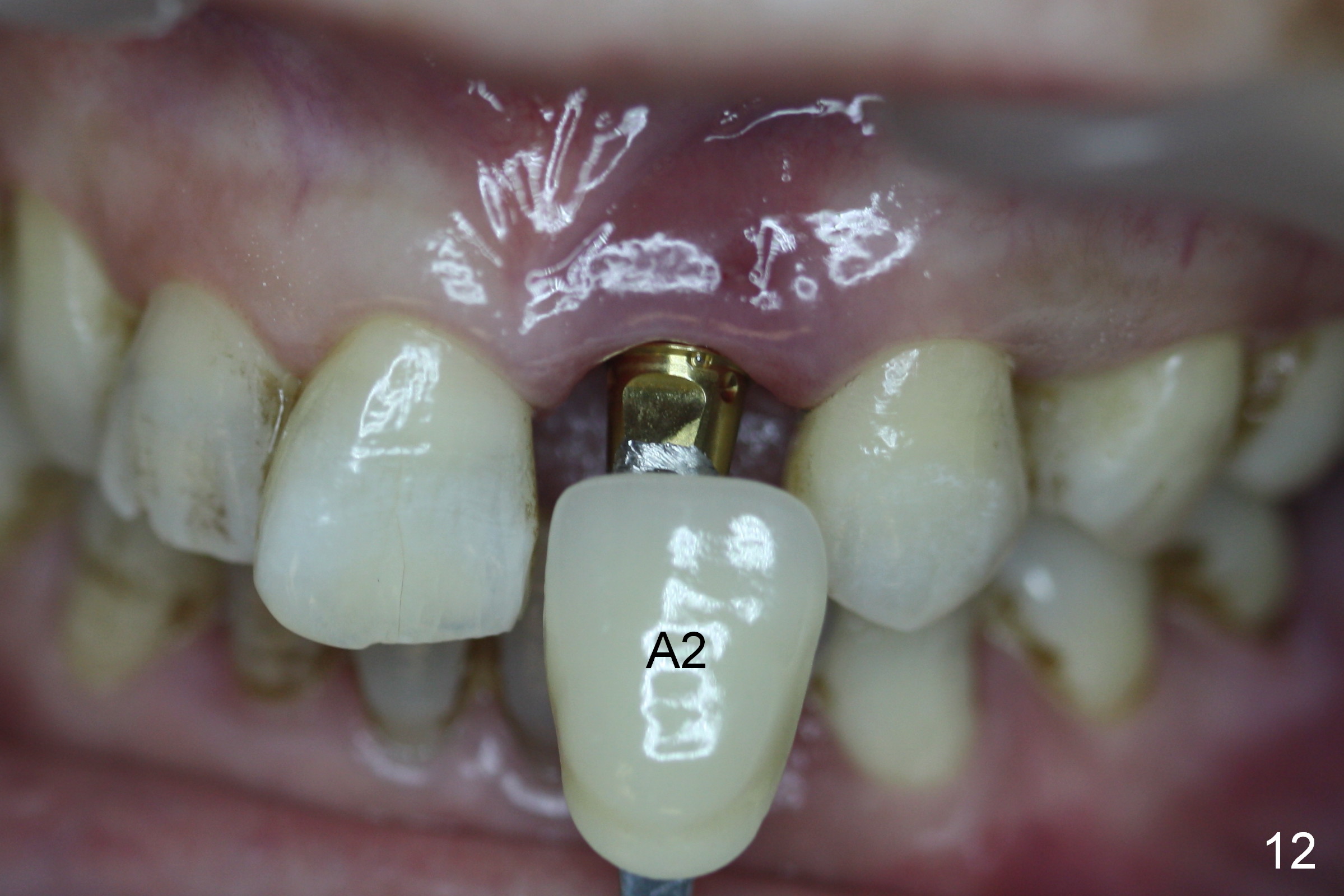
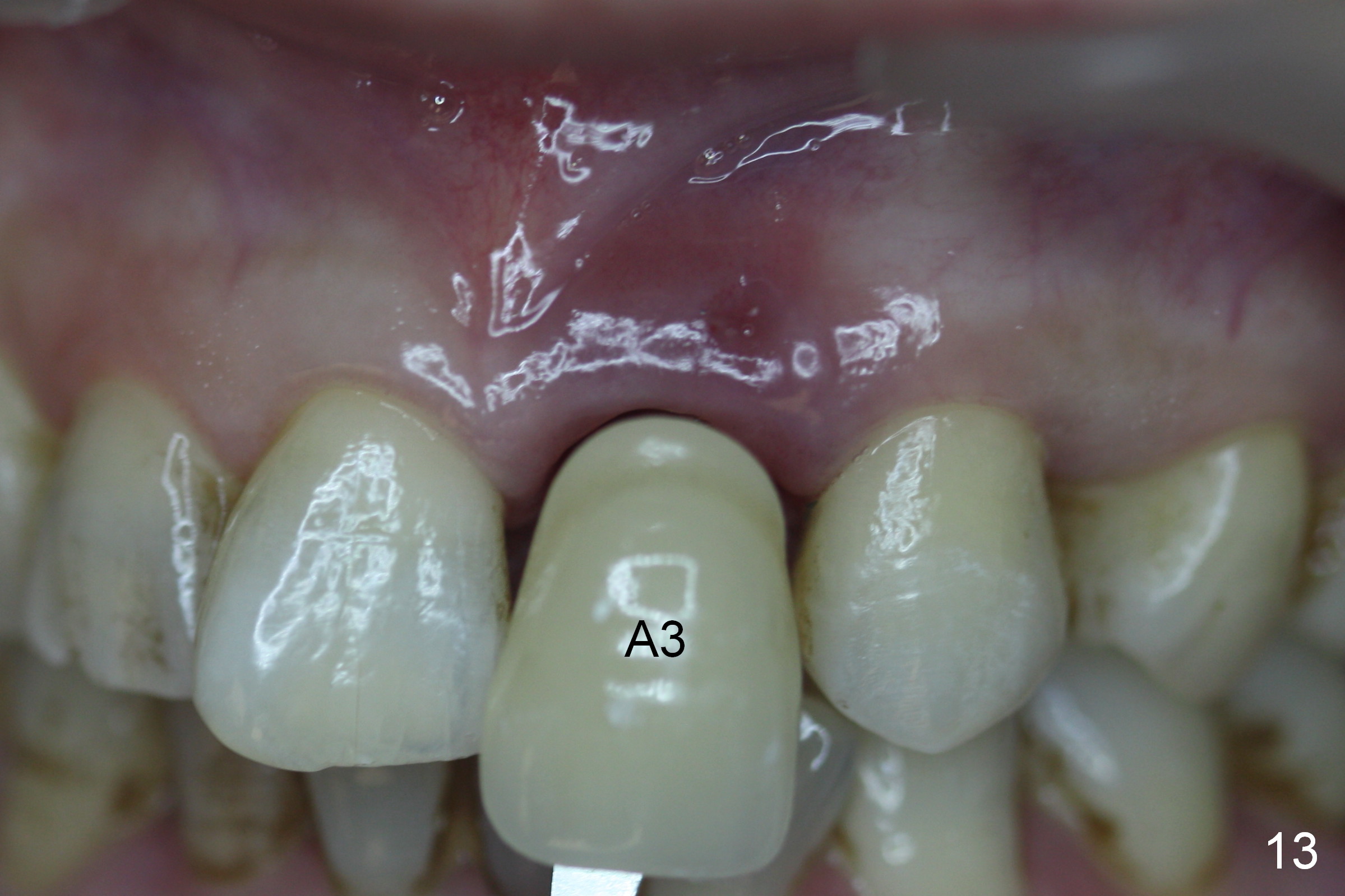
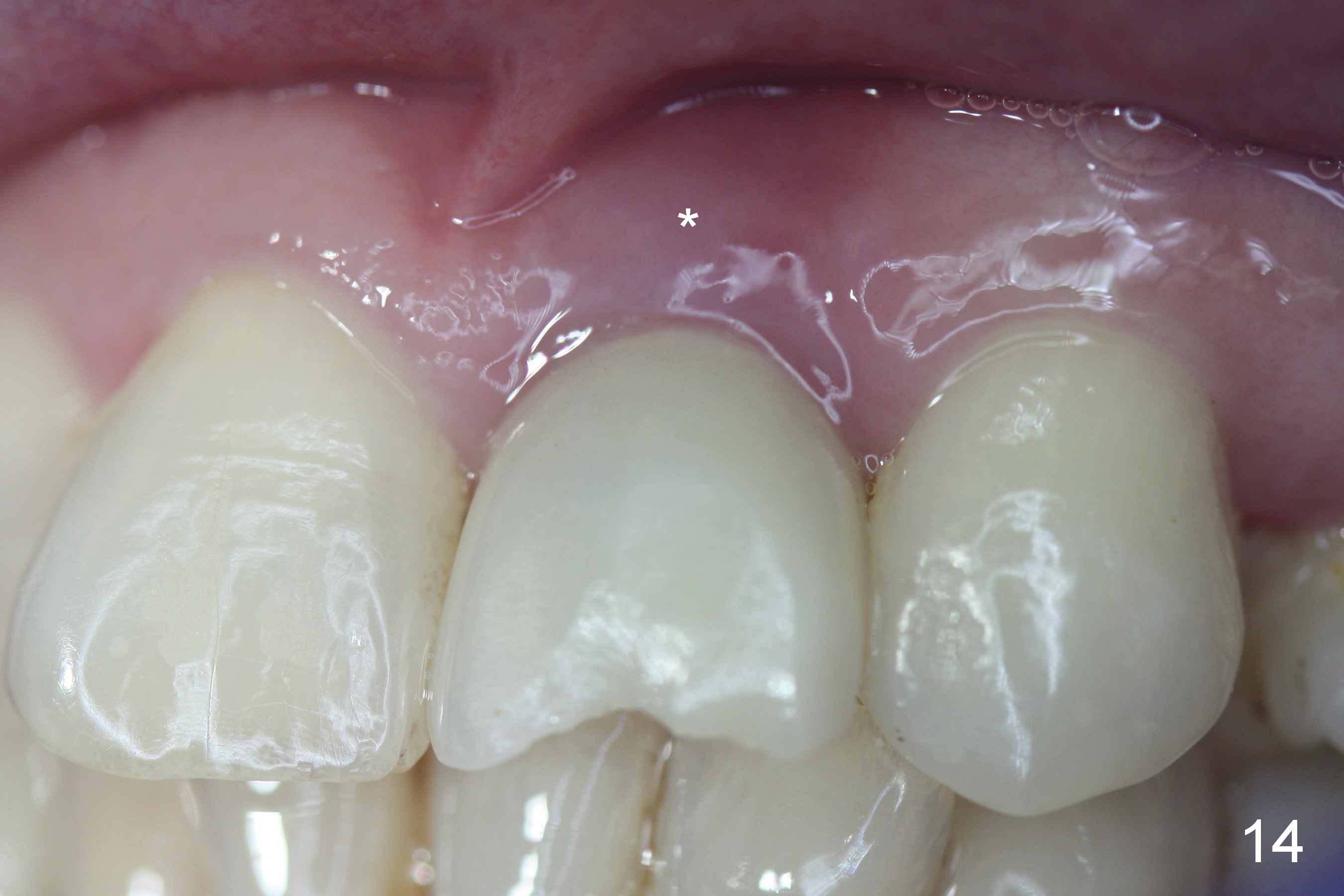
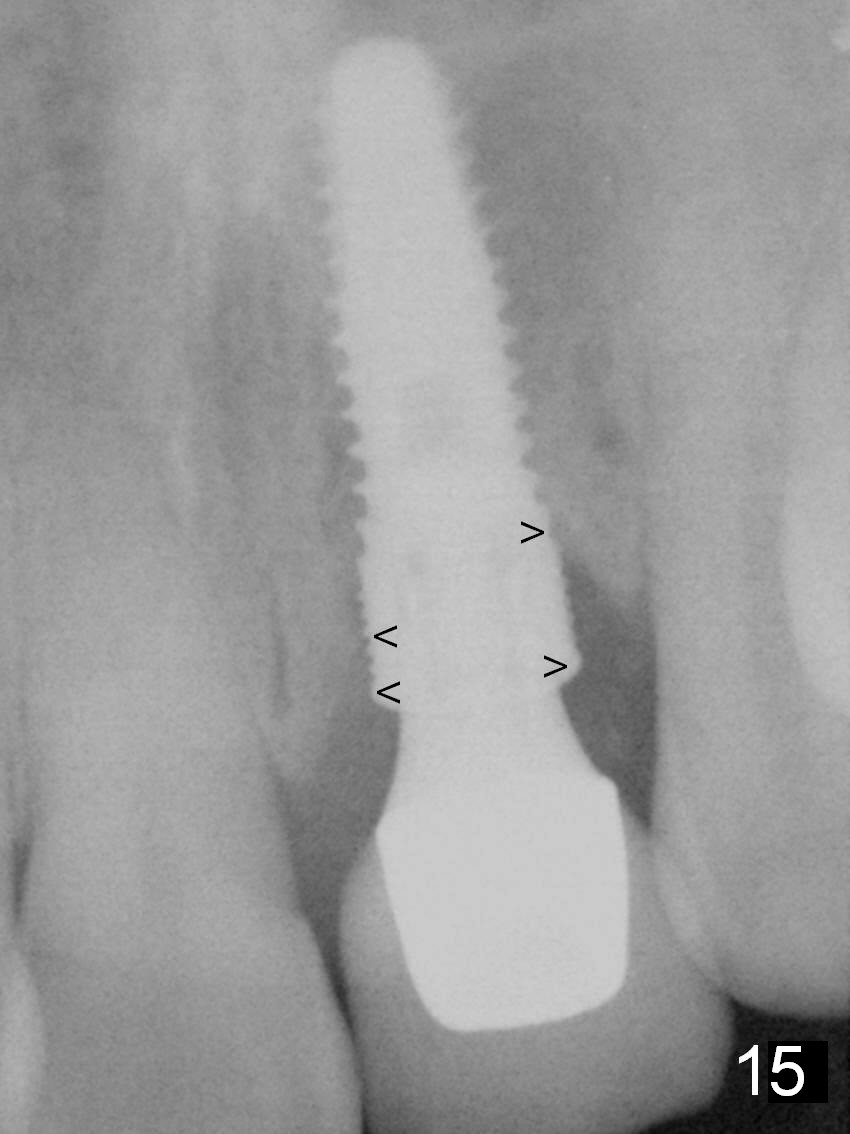
The temporary abutment is loosened 6 months postop; there is no apparent bone regeneration mesial and distal to the implant (Fig.11 *). The labial gingiva easily bleeds when the temporary abutment is removed for a permanent abutment and impression. Although there is no history of purulent discharge, the labial gingiva remains erythematous, a sign of labial bone loss (Fig.12,13). Five months post cementation, the patient complains of hemorrhage on brushing, a sign of periimplantitis (Fig.14 *). Purulent smell persists 16 months post placement in spite of use of Water Pik. Gingival bleeding persists 18 months postop (12 months post cementation; it appears that the coronal threads are not covered by the bone (Fig.15). It seems that bone graft is needed.
Return to Upper Incisor
Immediate Implant,
Technician
Xin Wei, DDS, PhD, MS 1st edition 02/26/2015, last revision 06/13/2018