,%208%20wks.jpg)
 |
 |
 |
 |
||
 |
 |
 |
 |
 |
 |
 |
 |
 |
|||
 |
 |
 |
 |
||
 |
 |
 |
|||
,%208%20wks.jpg) |
 |
 |
|||
 |
 |
 |
|||
 |
 |
||||
Place Early Implants as Immediate Ones
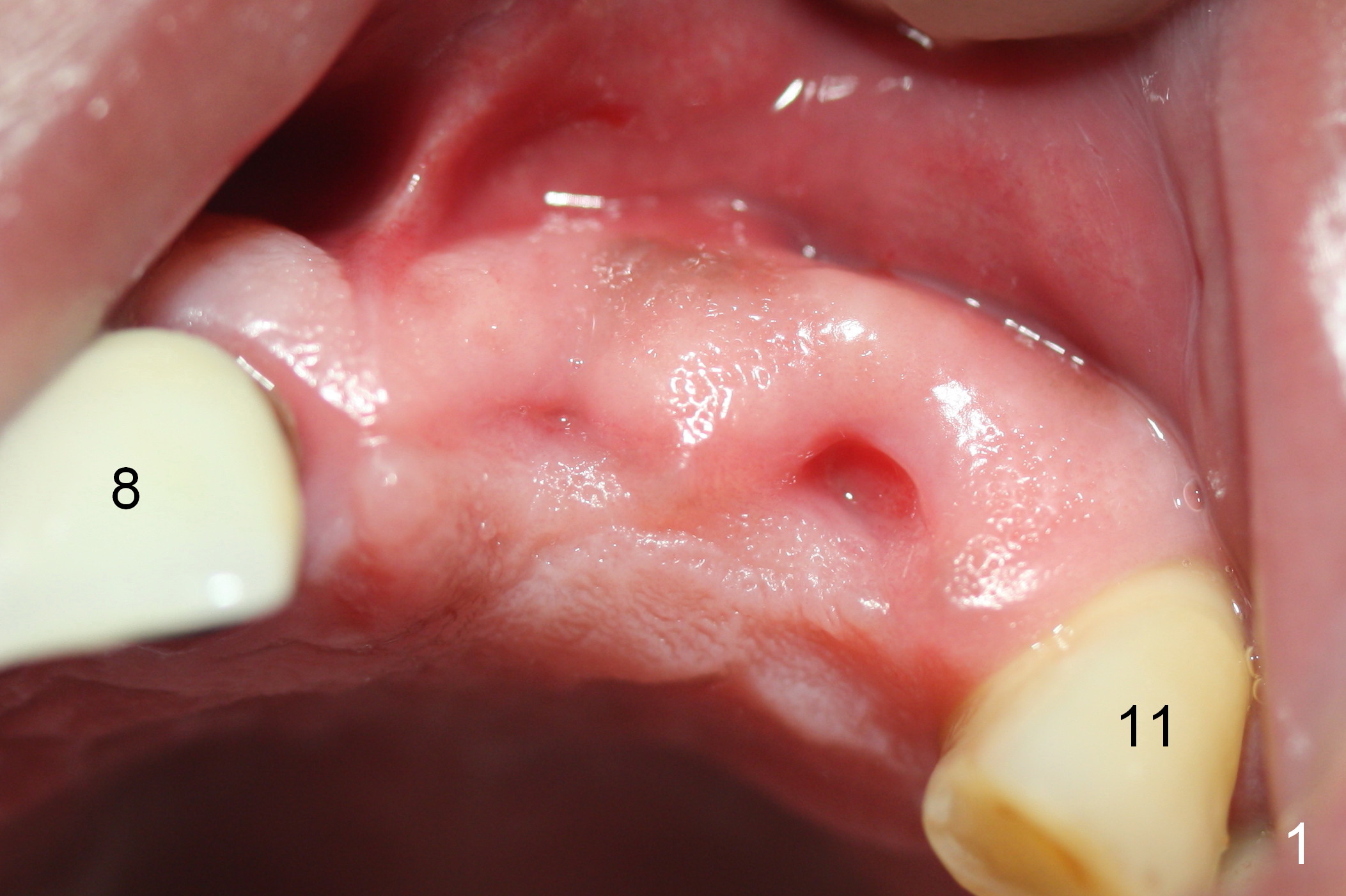
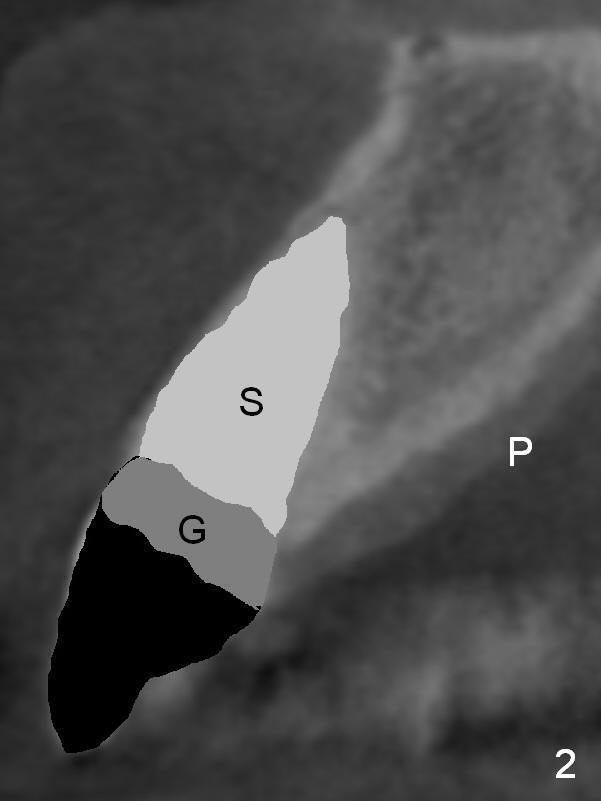
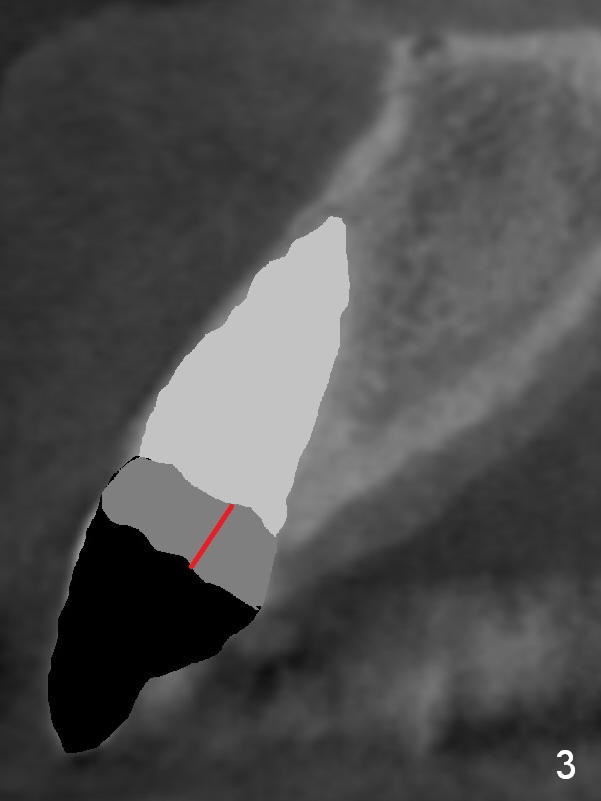
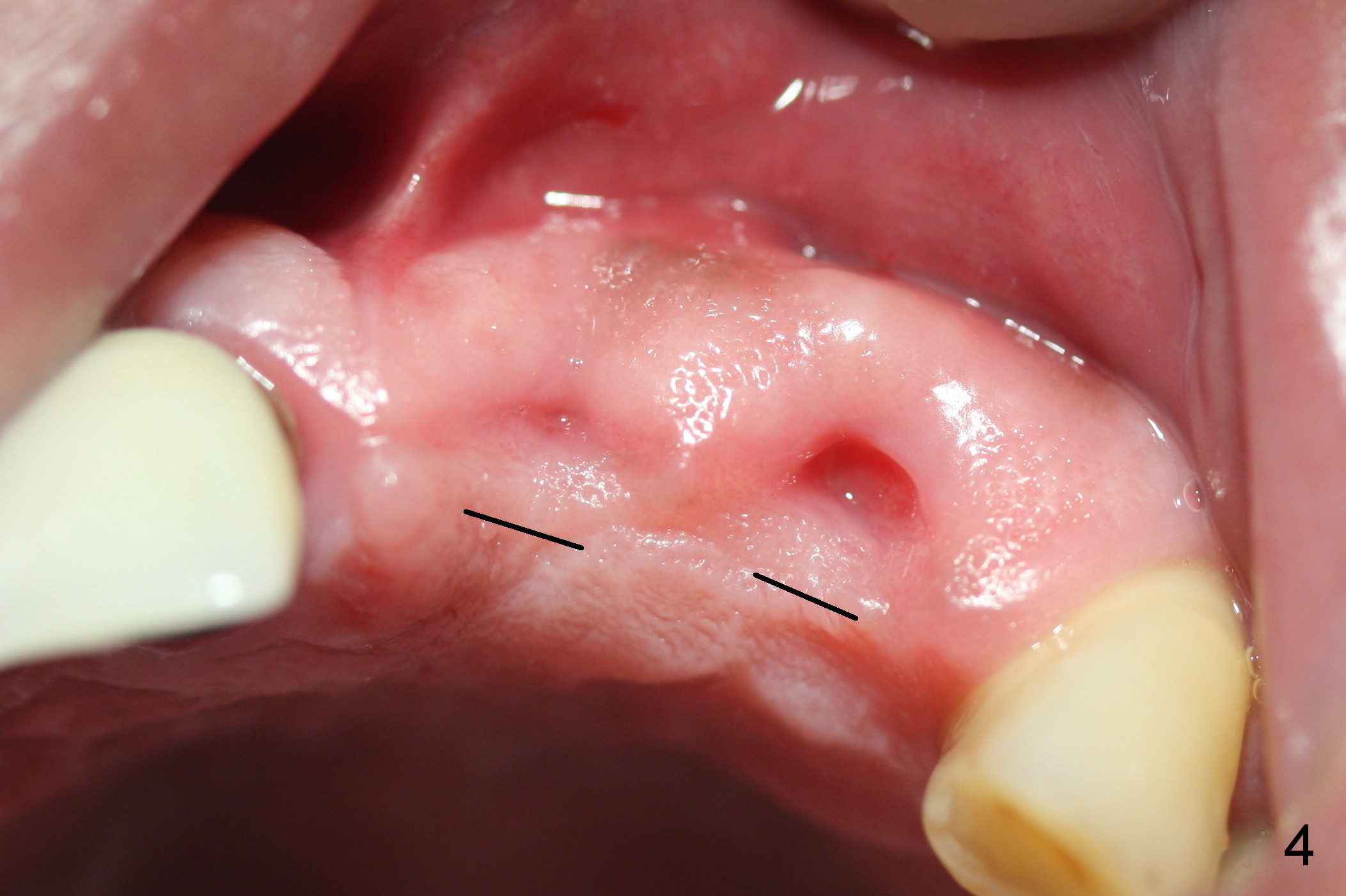
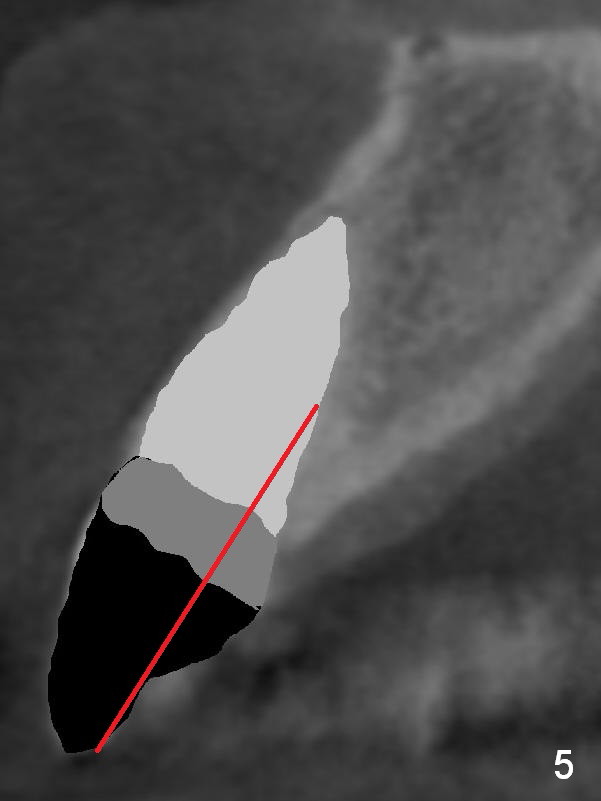
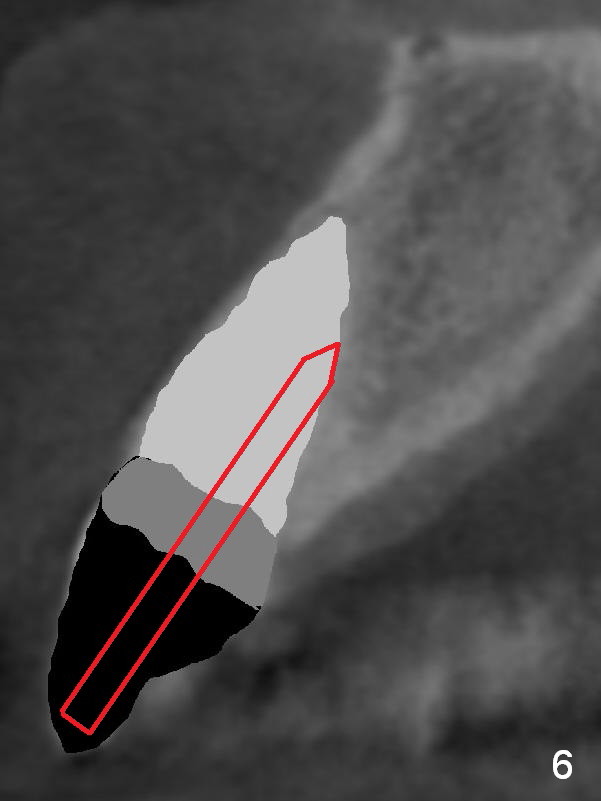
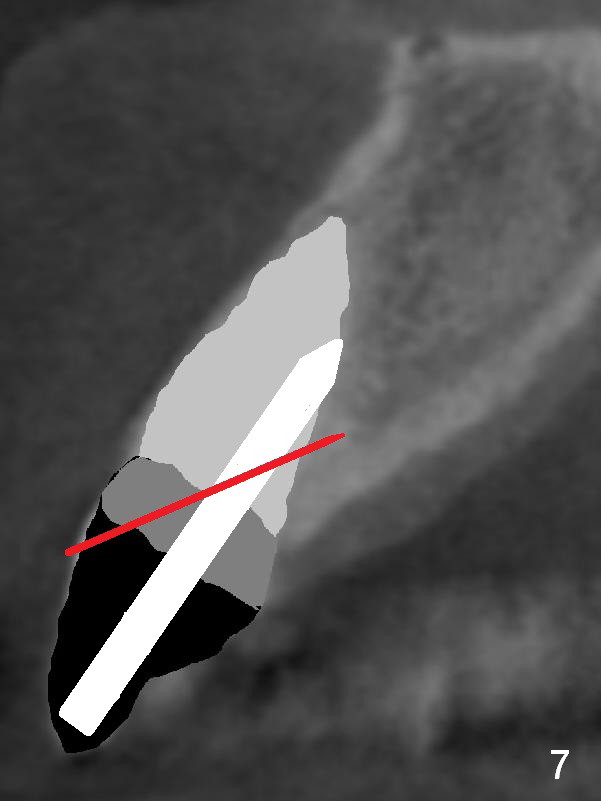
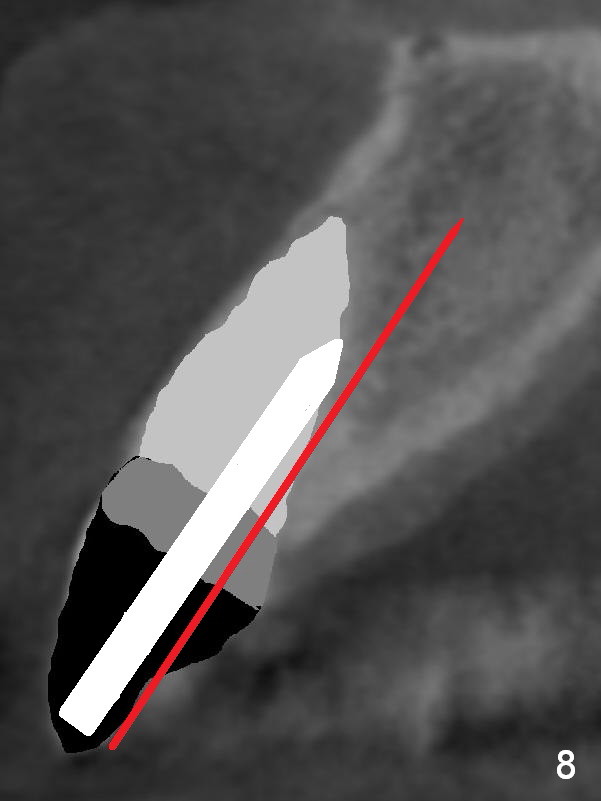
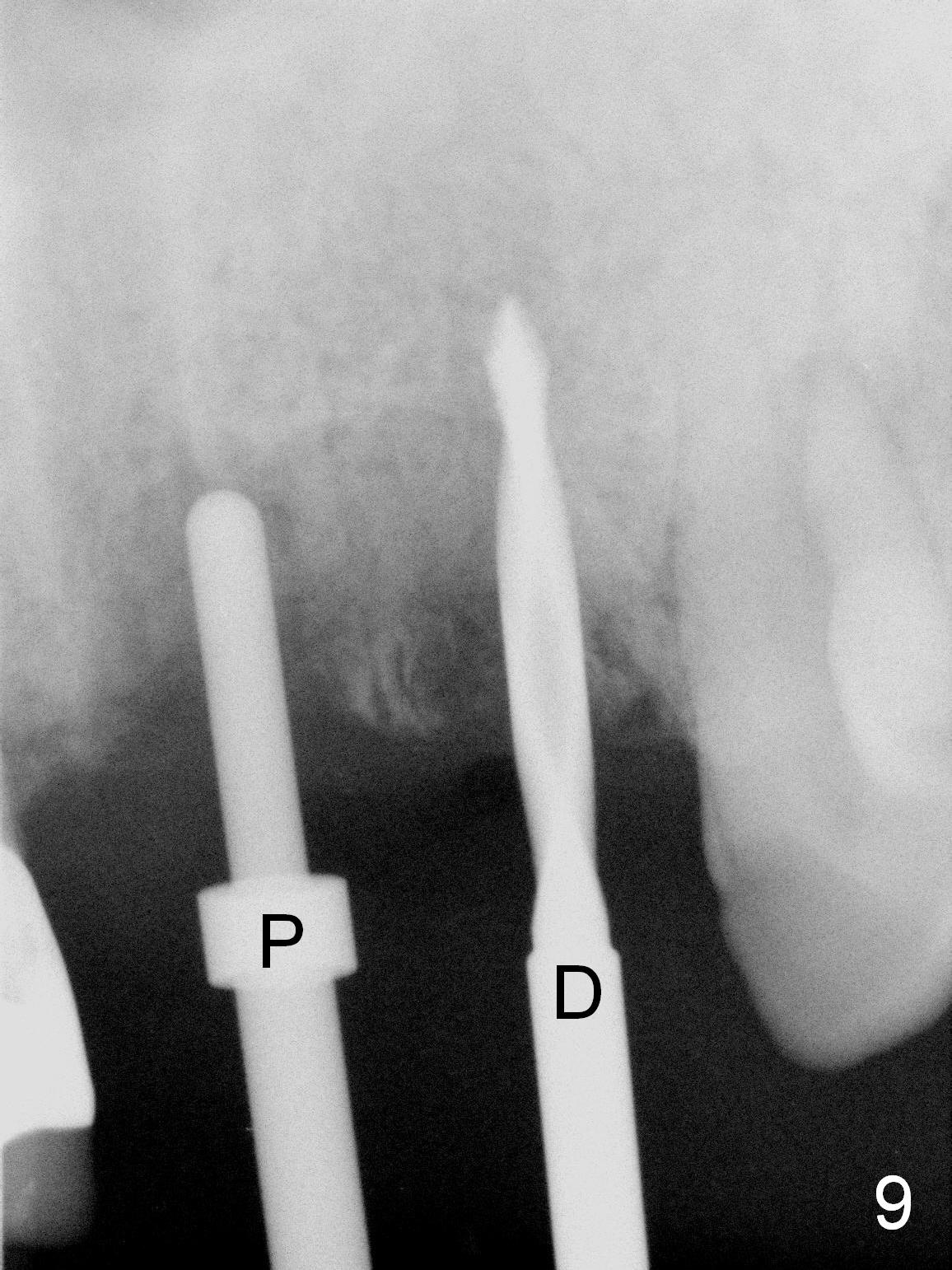
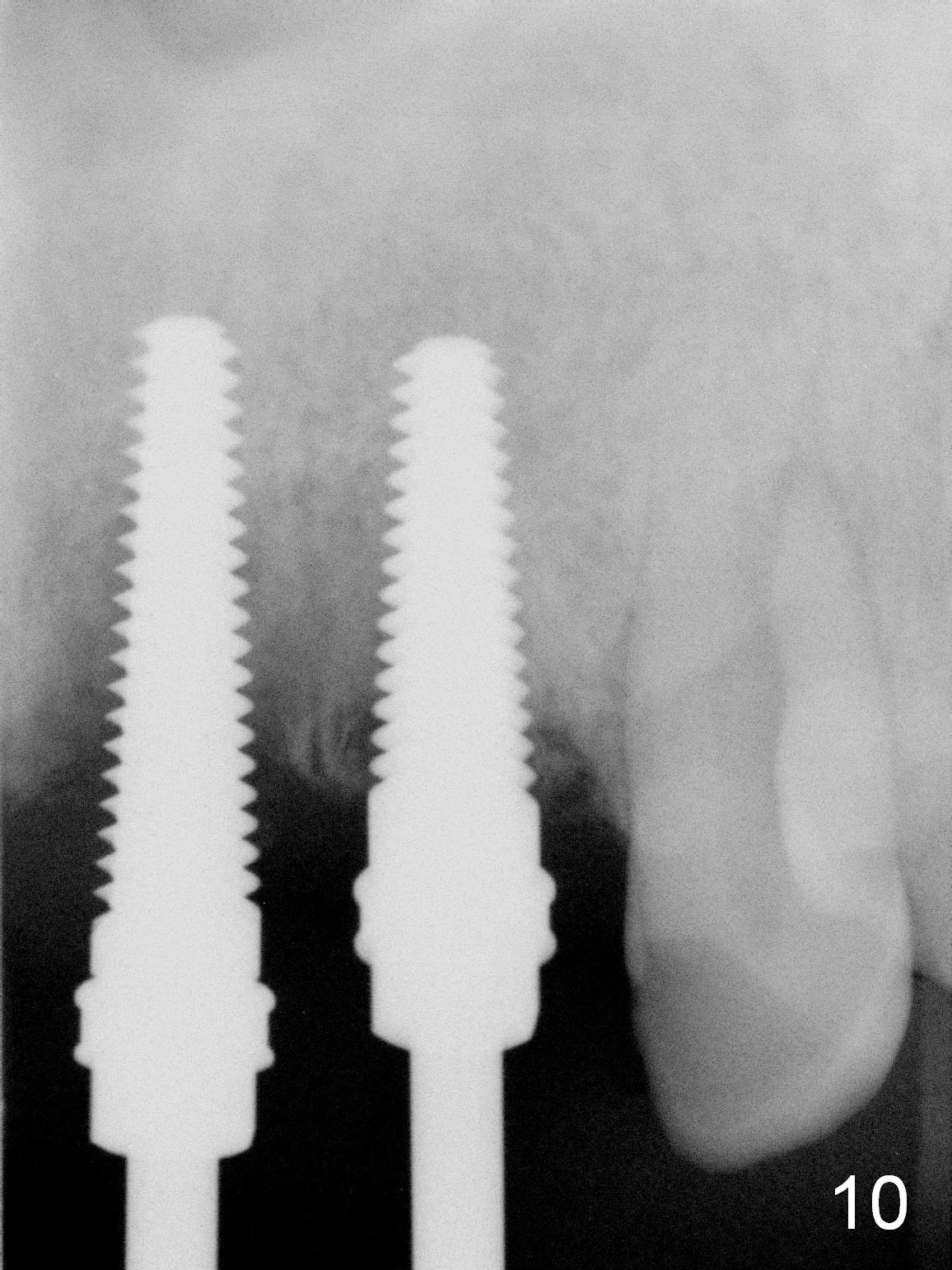
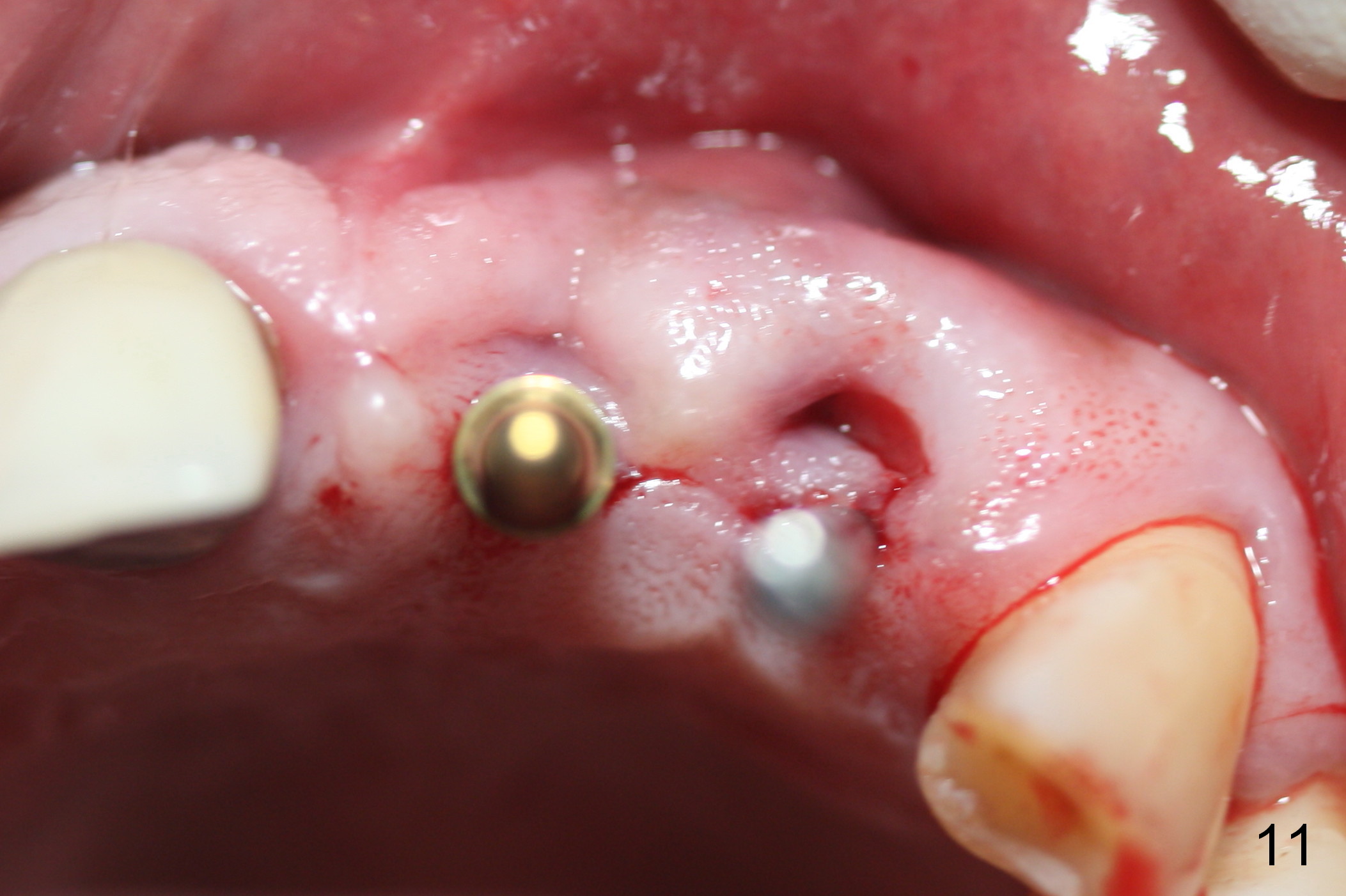
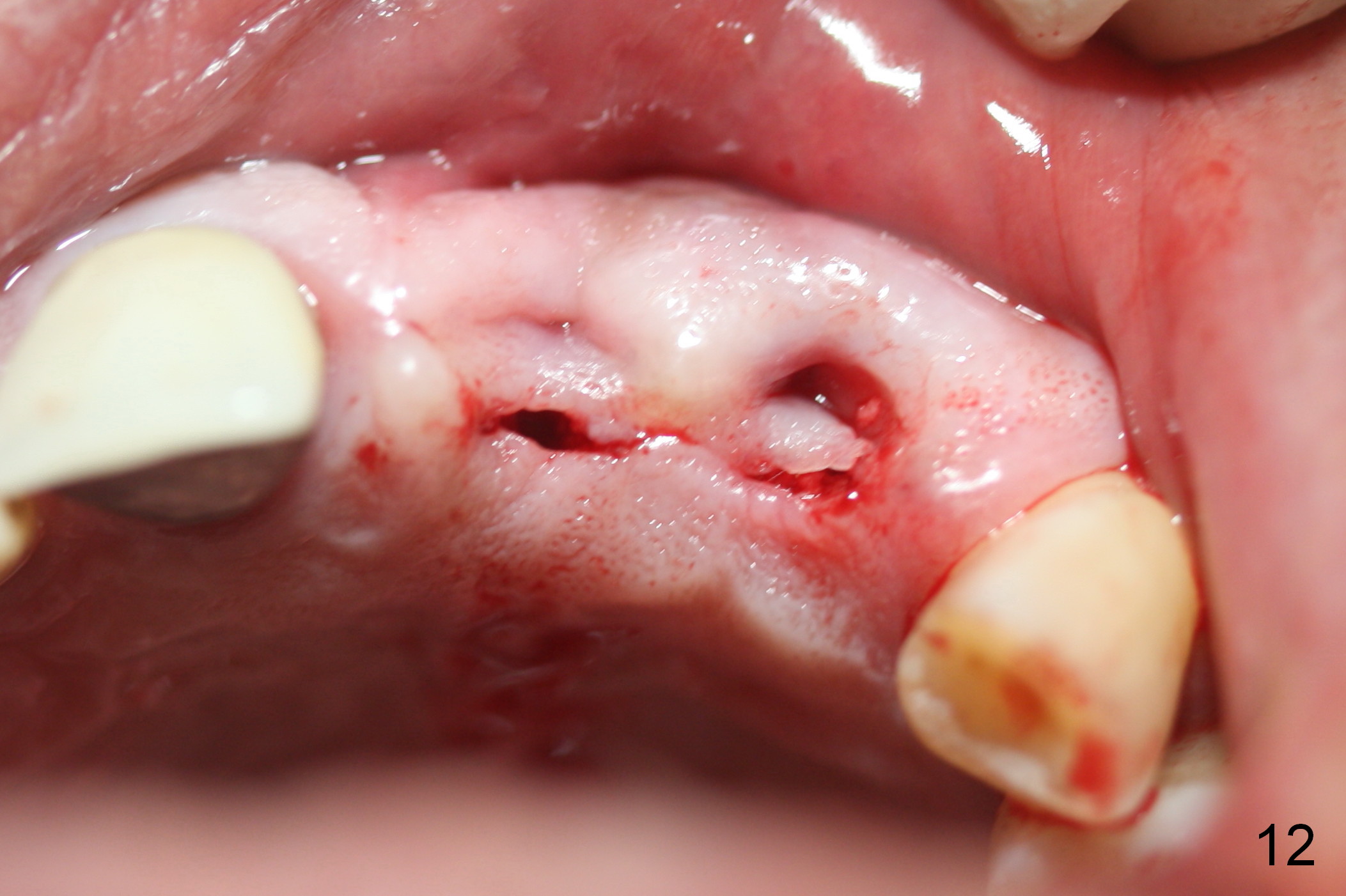
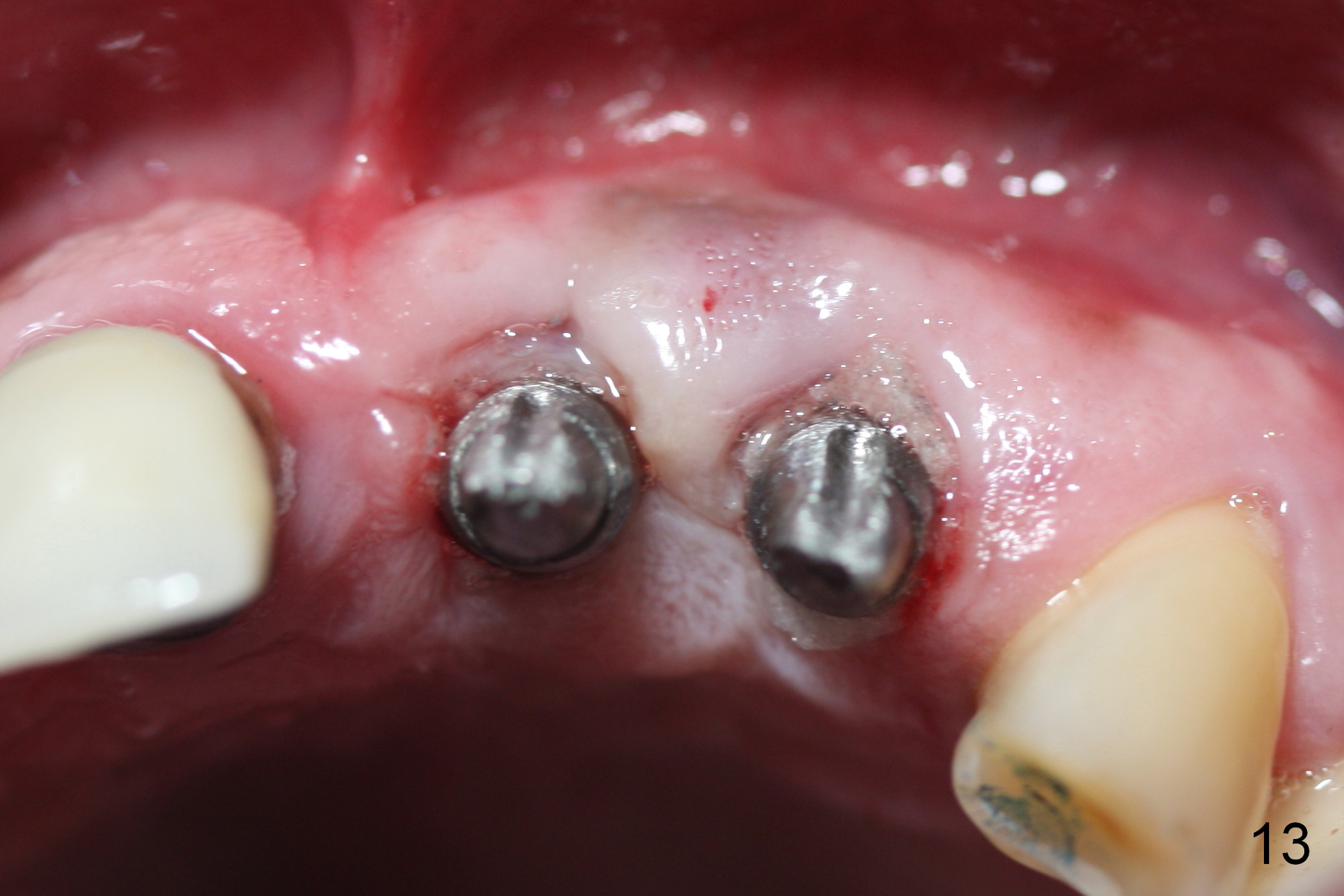
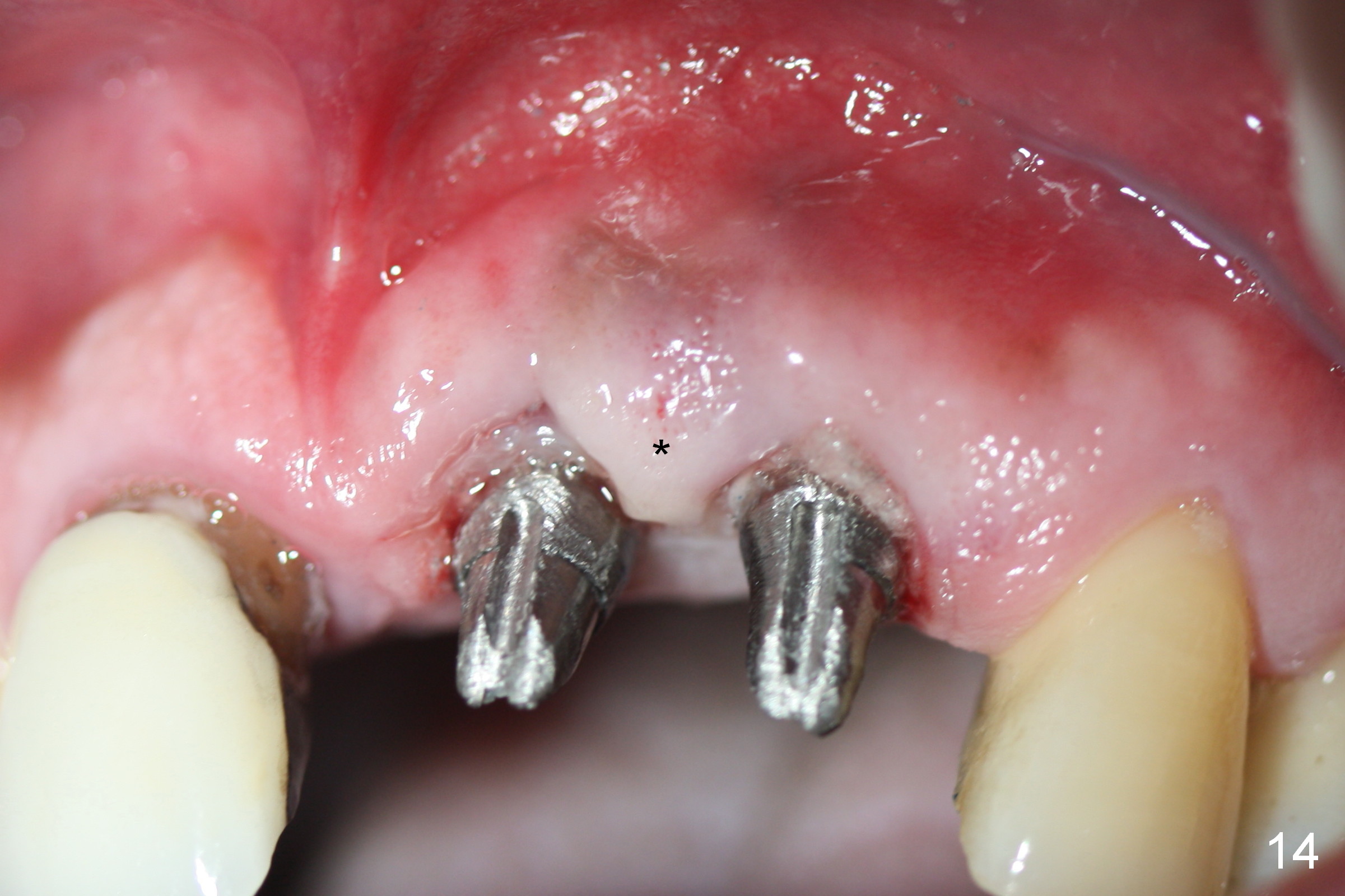
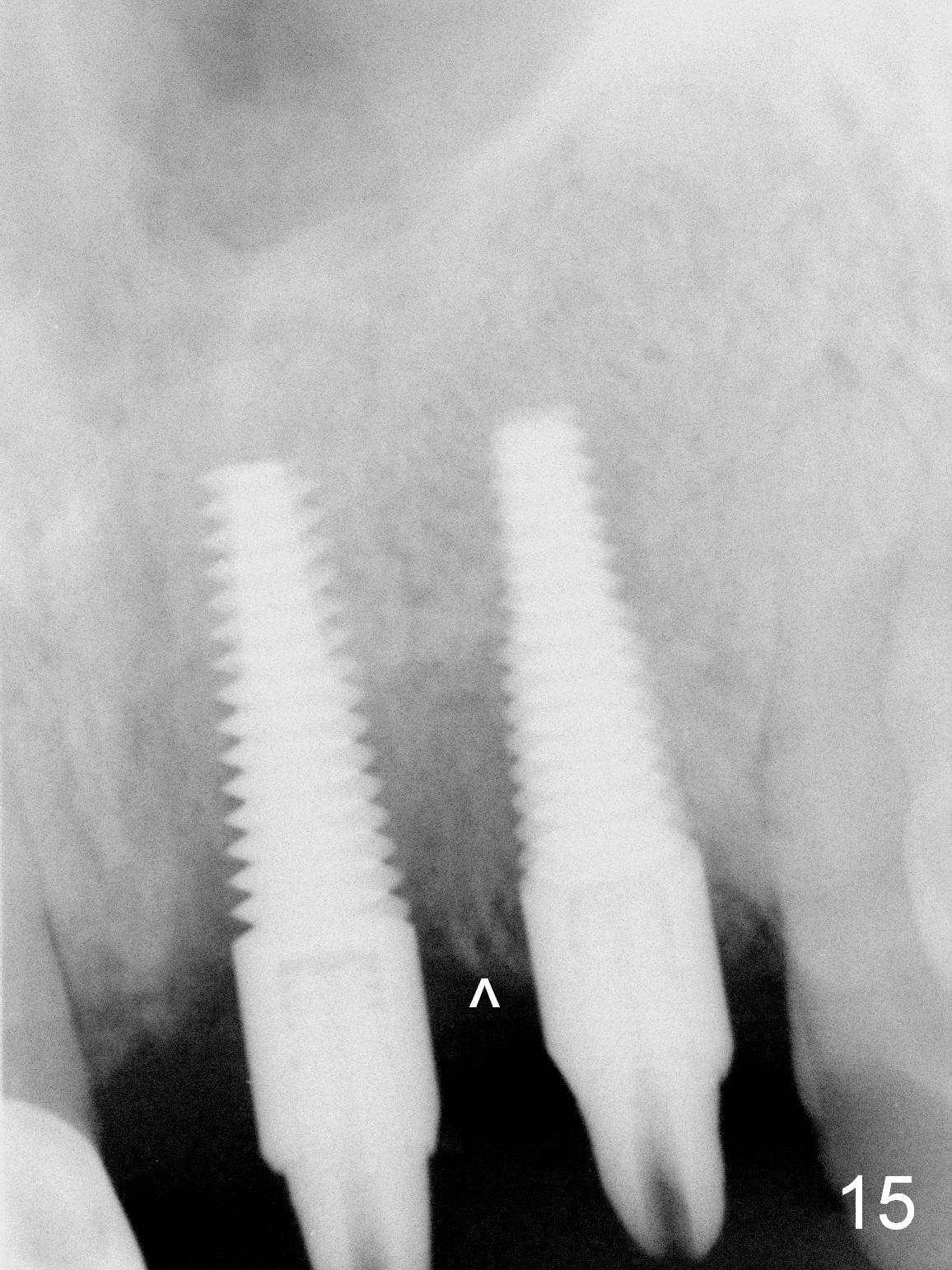
The teeth #9 and 10 were extracted apparently without socket preservation approximately 3 months ago. The sockets heal without apparent soft or hard tissue collapse (Fig.1). Fig.2 is a CBCT cross section of an upper central incisor with illustration of a healing socket (S) and overlying gingiva (G). To place implants in a favorably surgical and restorative position, an incision should be made as palatal (P) as possible (Fig.3, 4 lines). The #15 blade is then driven with a mallet into the low density socket to initiate osteotomy, i.e., bone expansion and condensation (Fig.5 red line). The osteotomy is enlarged with 1, 1.5, 2 and 3 mm osteotomes; the last osteotome is unavoidably pushed buccally (Fig.6, least resistant area). When the last osteotome is removed (Fig.7 white area), a 2 mm pilot drill is used to start a new, more palatal entry obliquely (Fig.7 red line). Once got a "bite", the drill is redirected to finish the depth of the more favorable osteotomy (Fig.8 red line). Fig.9, 11 show a parallel pin (P) and the pilot drill (D) at the sites of #9 and 10, respectively (approximately 11 mm subgingival). Fig.12 shows the sites after the parallel pin and the pilot drill are withdrawn. The soft tissue architecture is basically preserved. When 4.5 mm taps are inserted, they are stable (Fig.10). Finally 4.5x17 mm implants are placed with insertion torque > 60 Ncm (Fig.13-15). Following insertion of abutments (3.5x5 mm), immediate provisionals are fabricated.
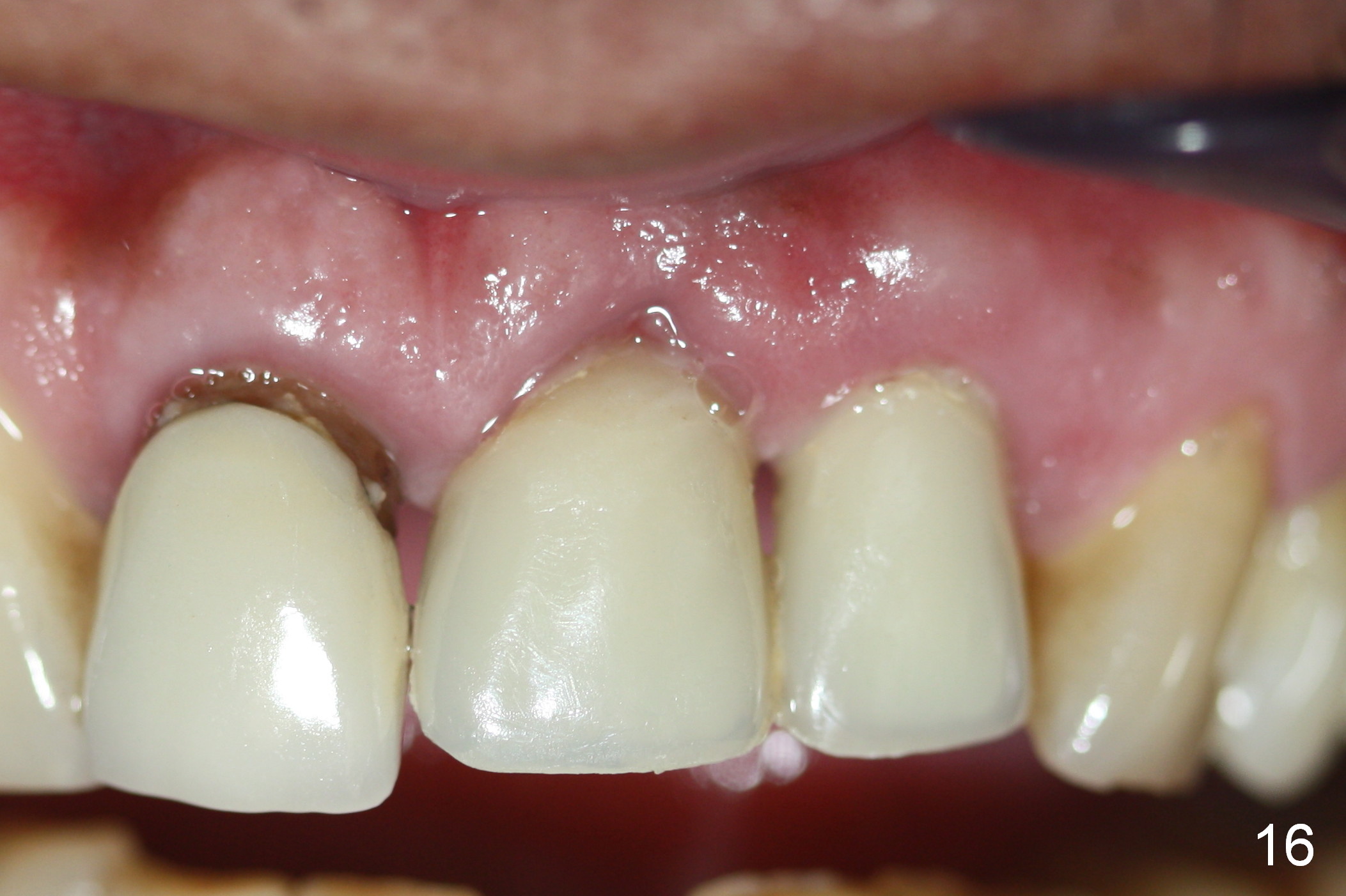
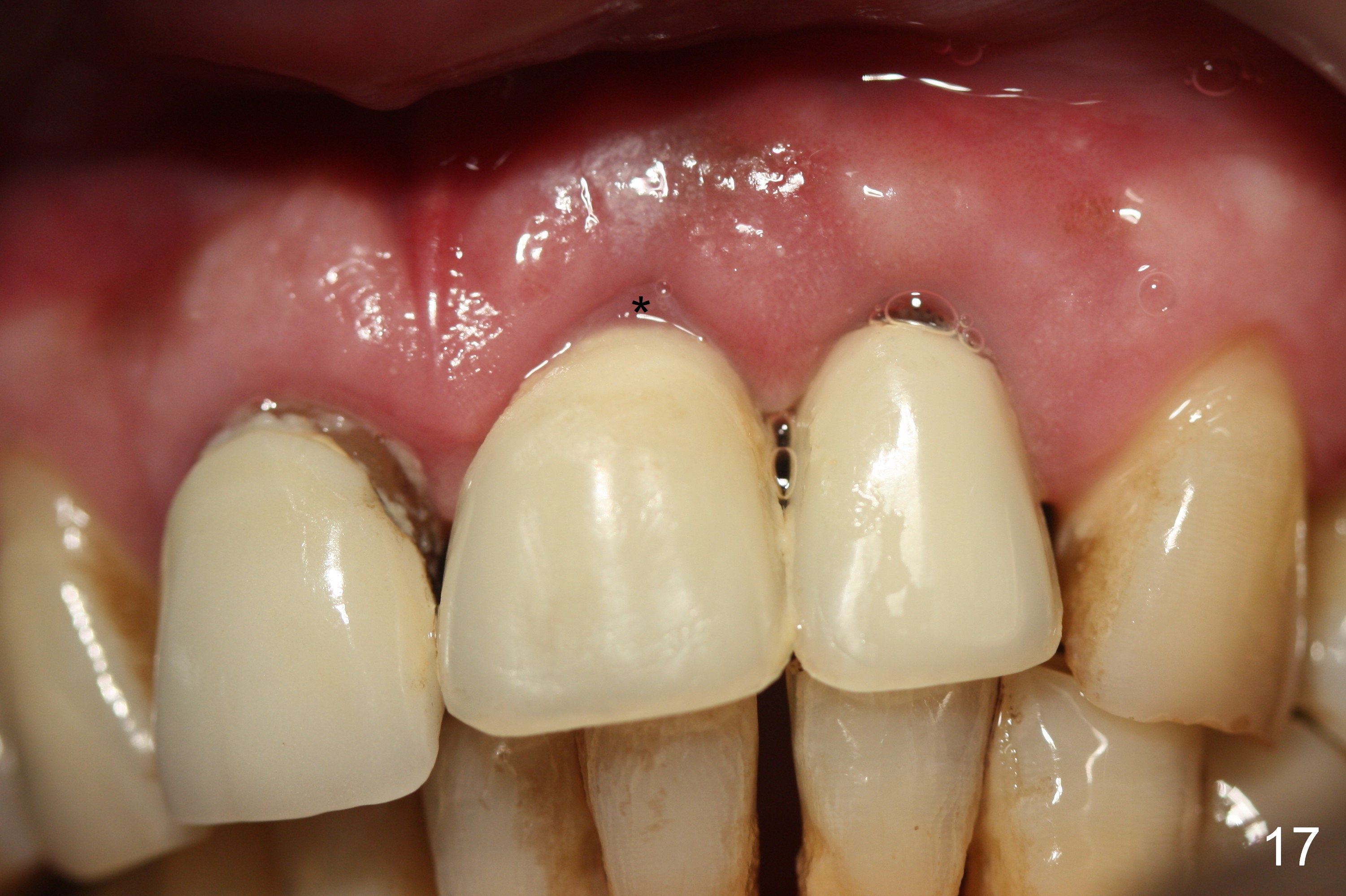
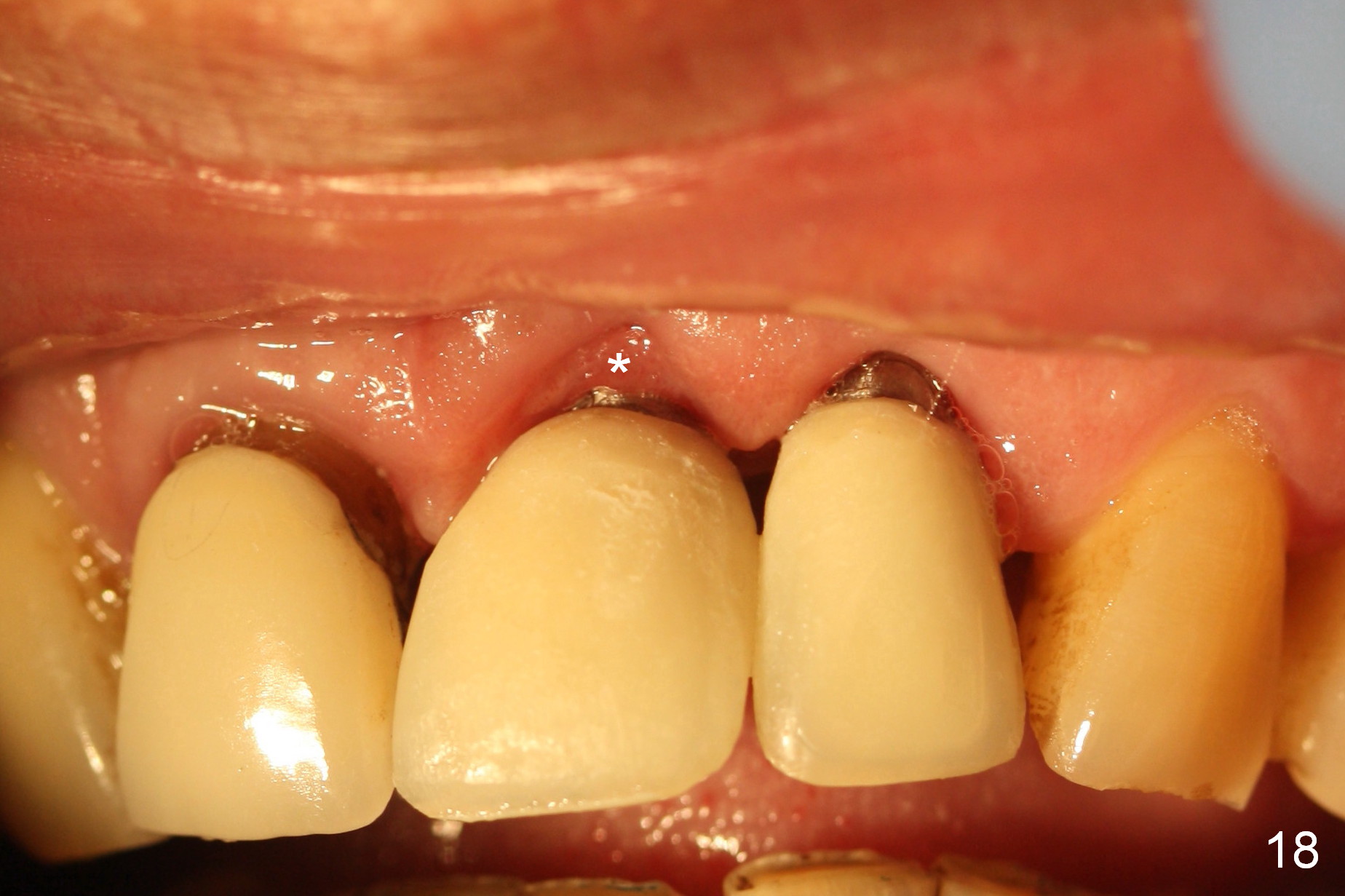
The patient returns for follow up with gratitude 1 and 4 weeks postop (Fig.16,17). The provisionals are relined to lower not only the incisal edges but also the gingival margin 4 weeks postop (Fig.18). The relined provisionals barely covers the margin of the prep. They should avoid contacting the immature gingiva (Fig.17,18 *).
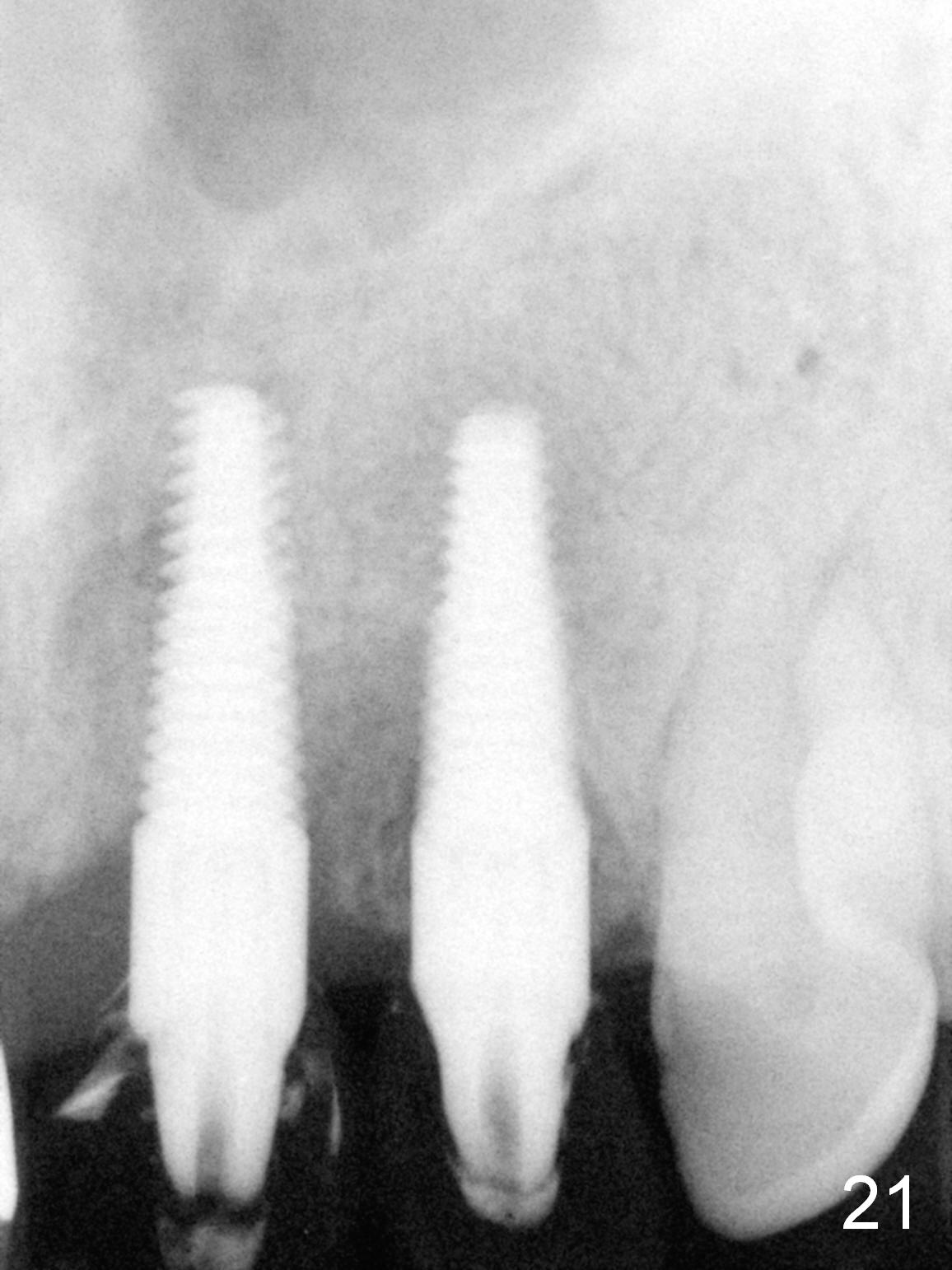
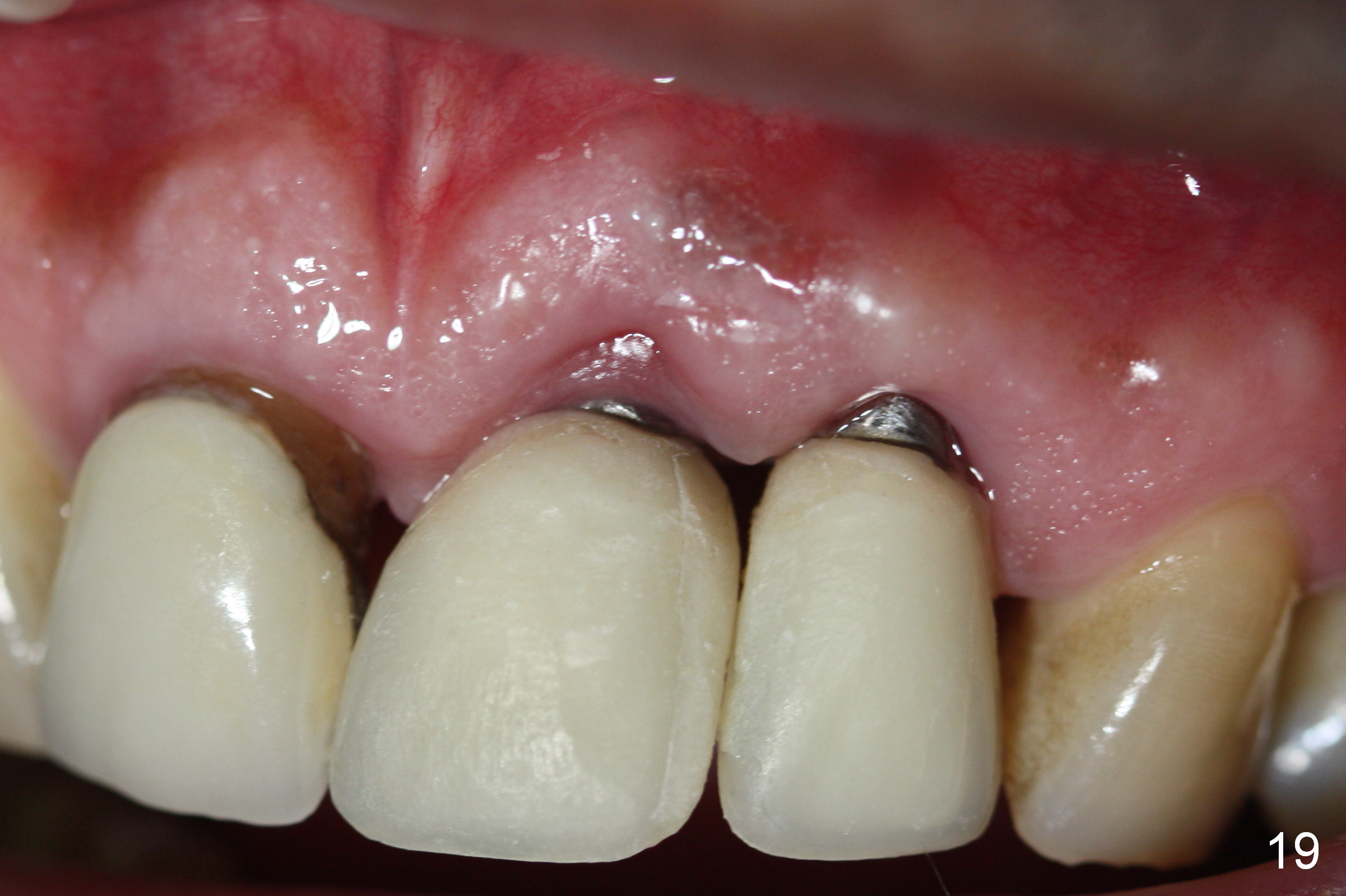
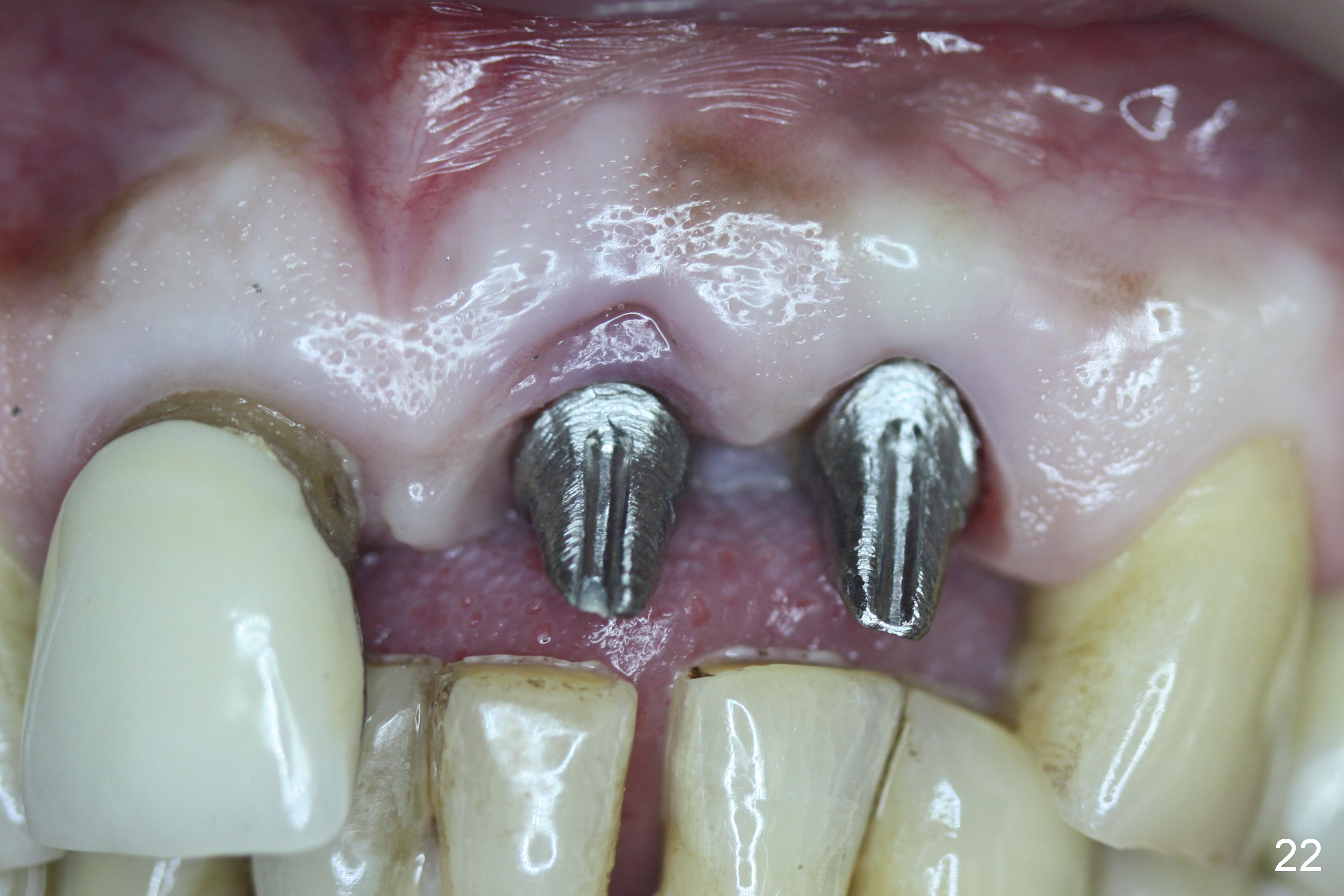
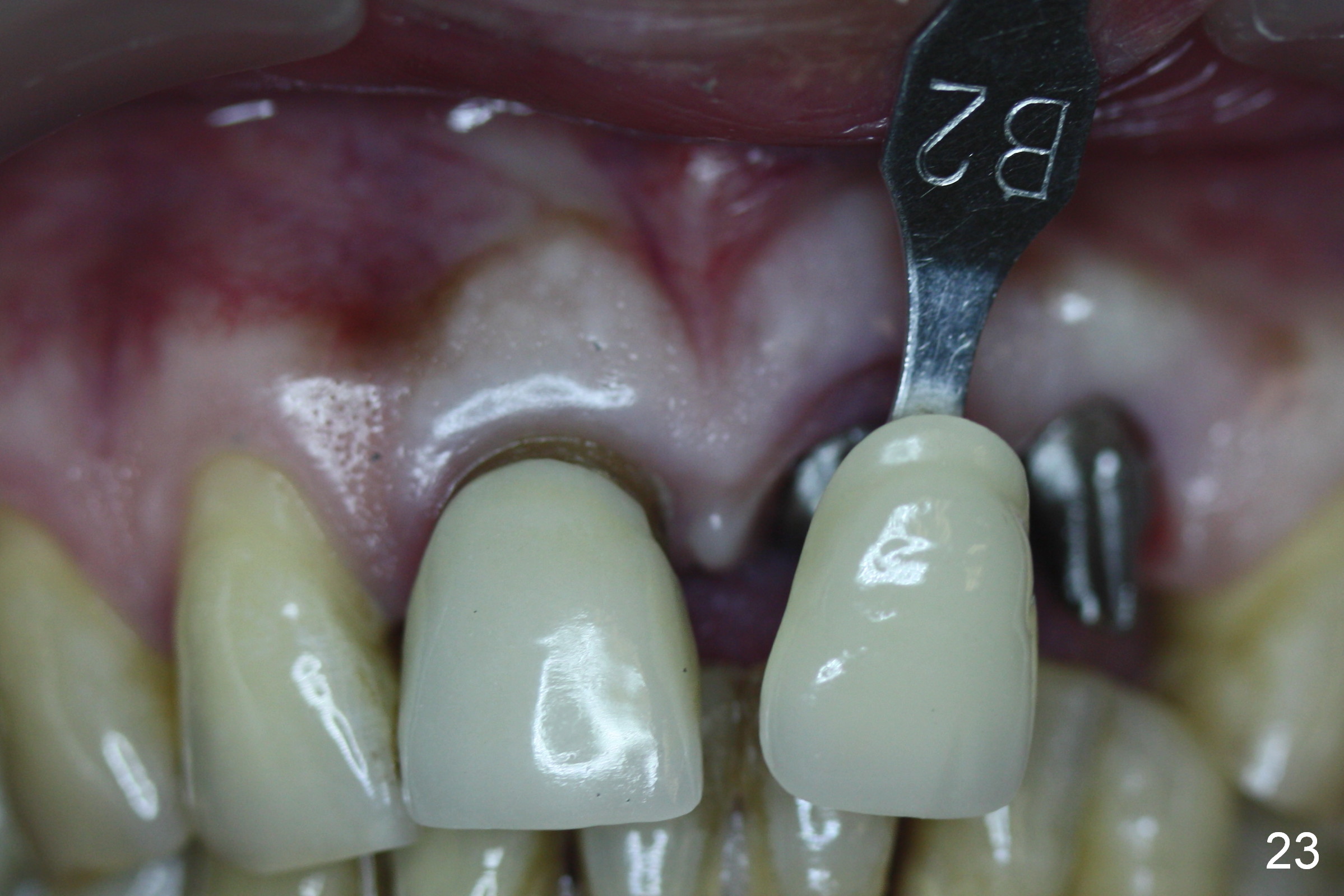
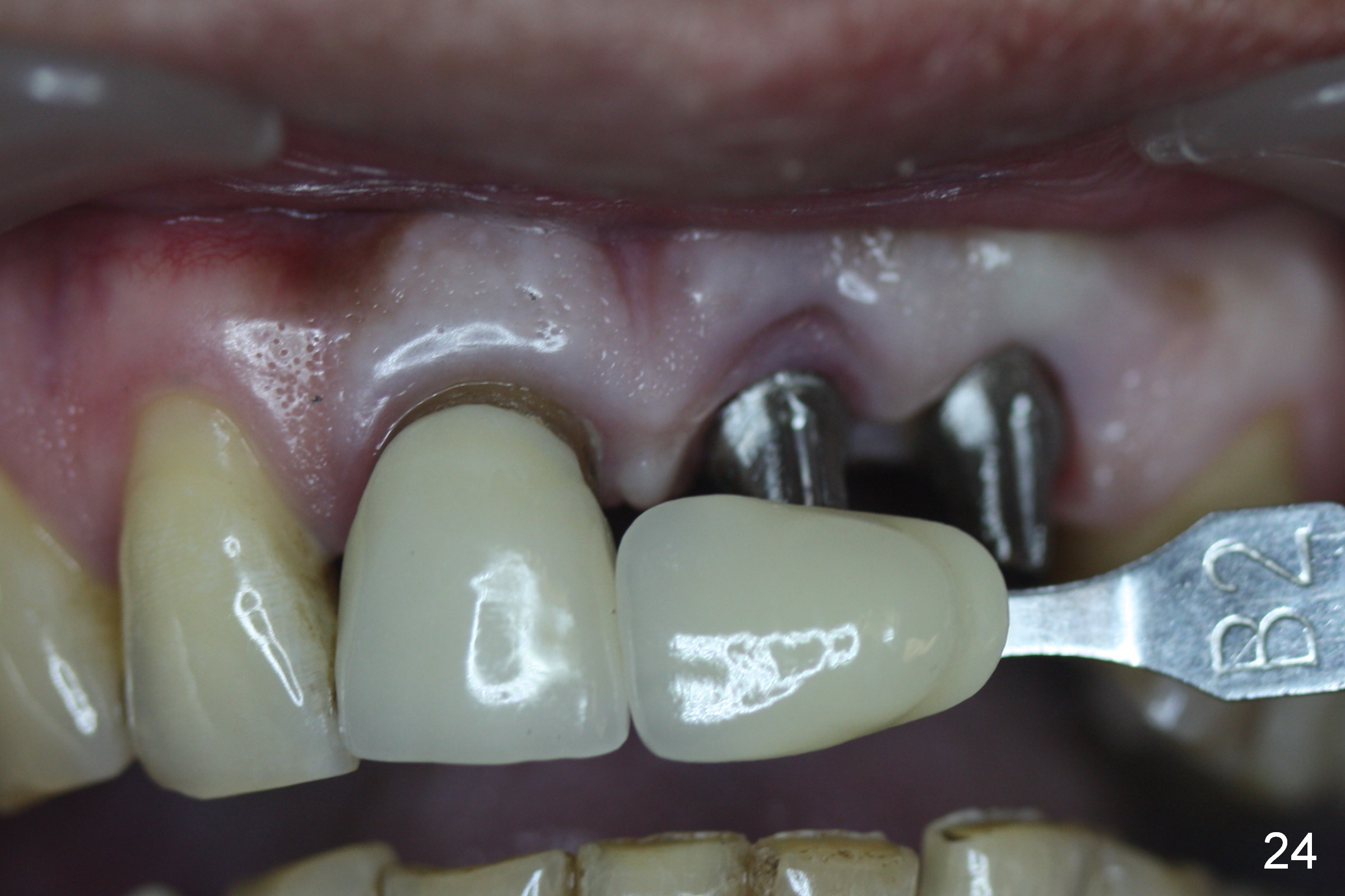
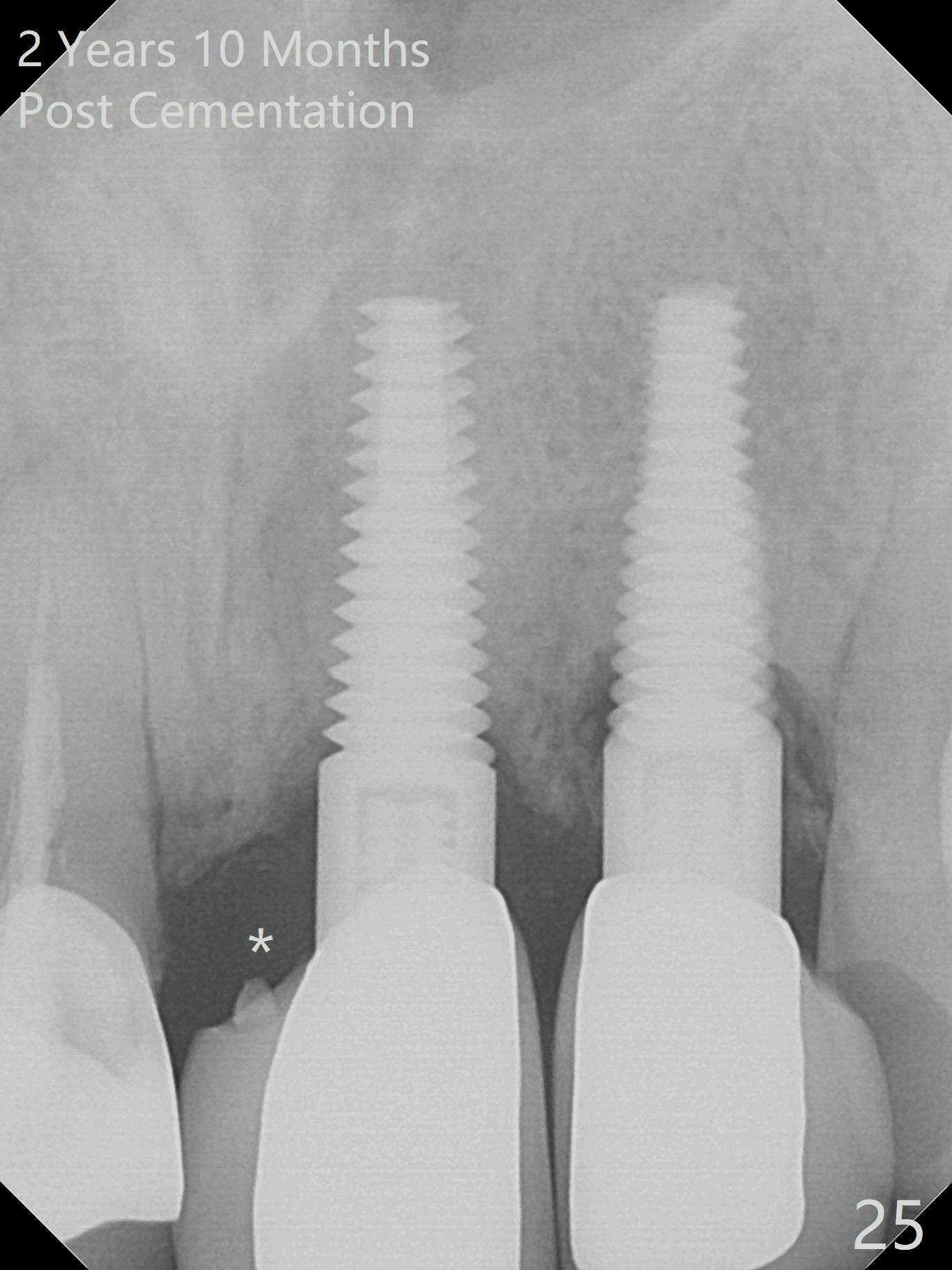
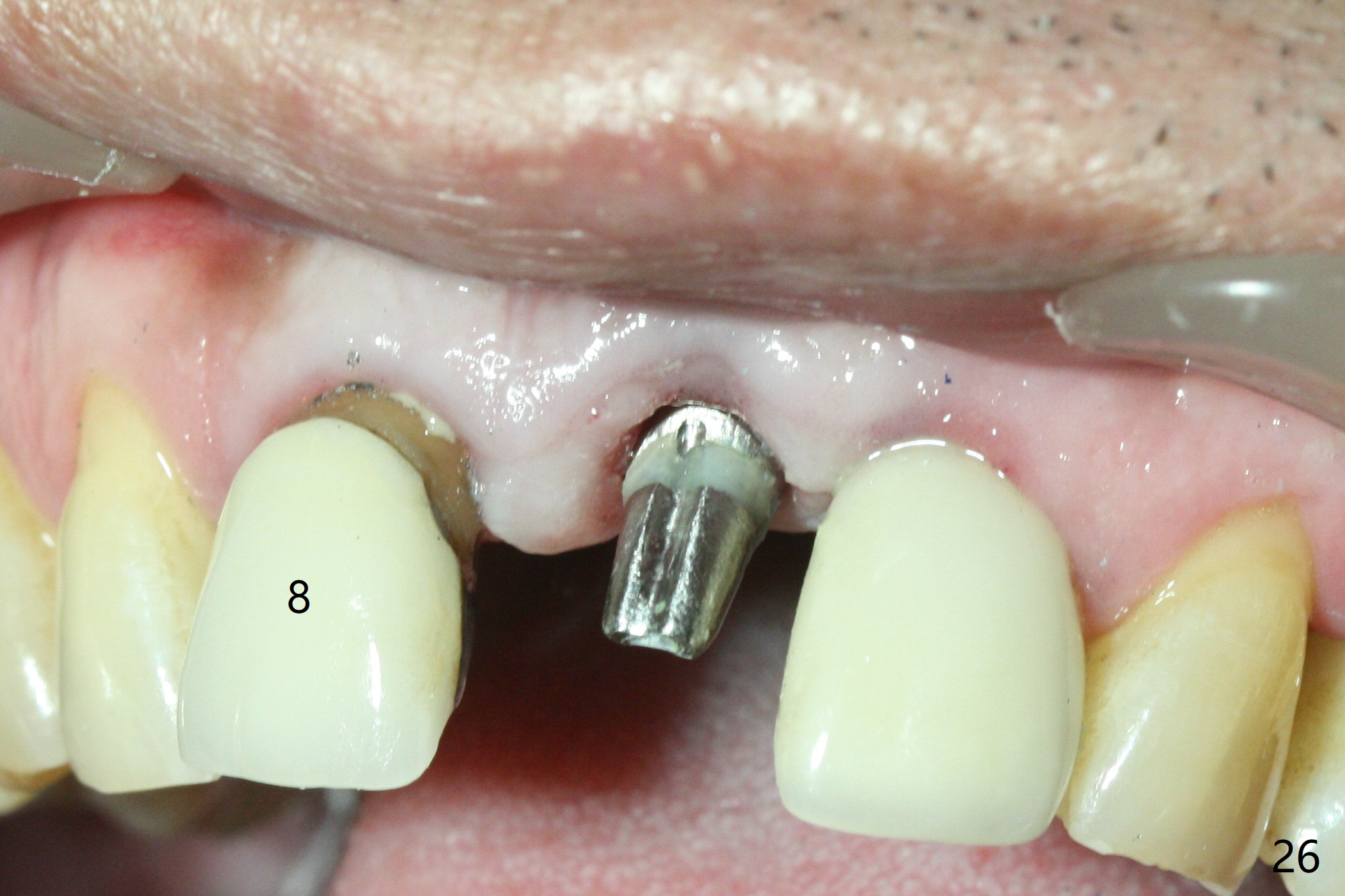
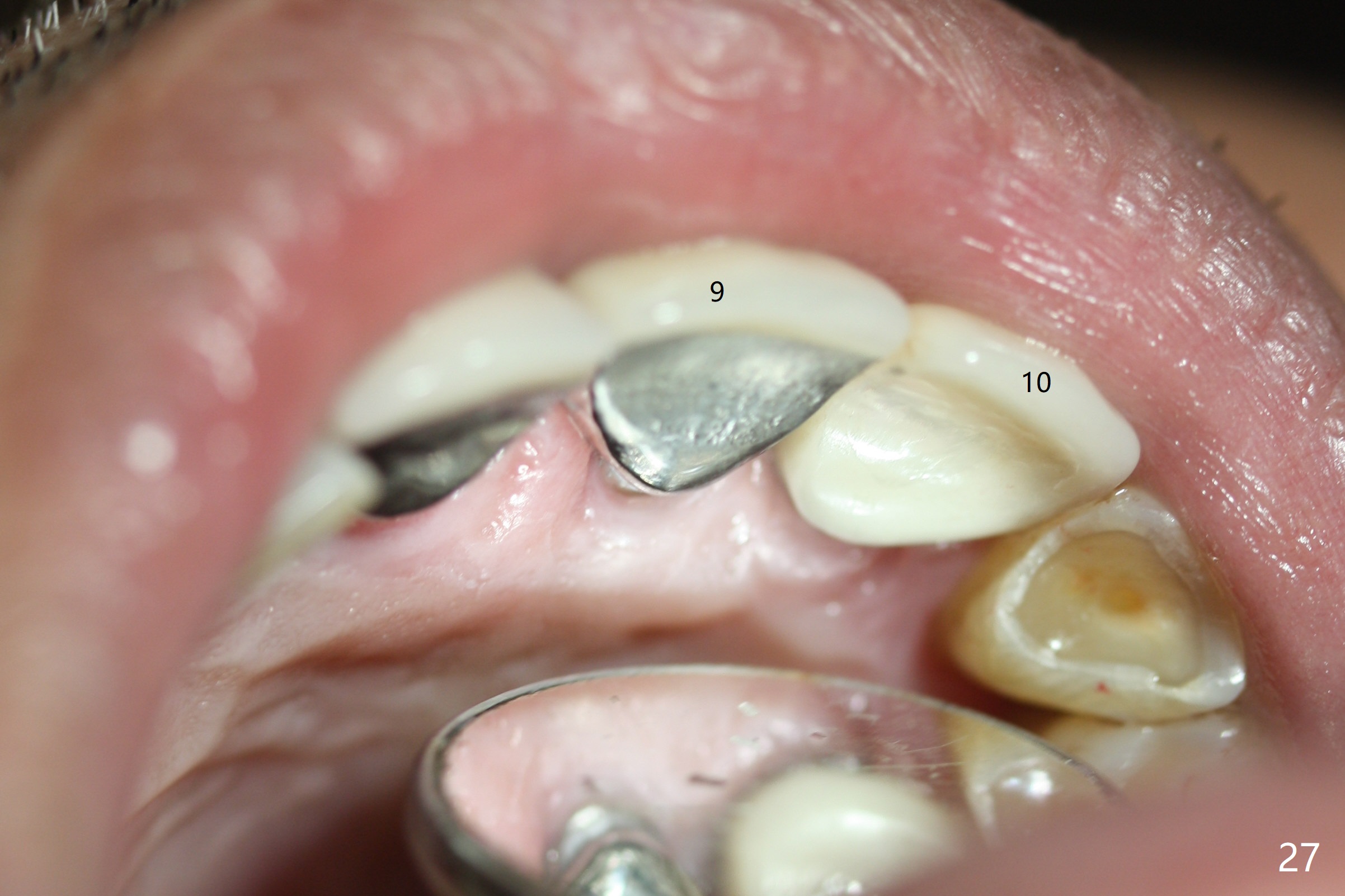
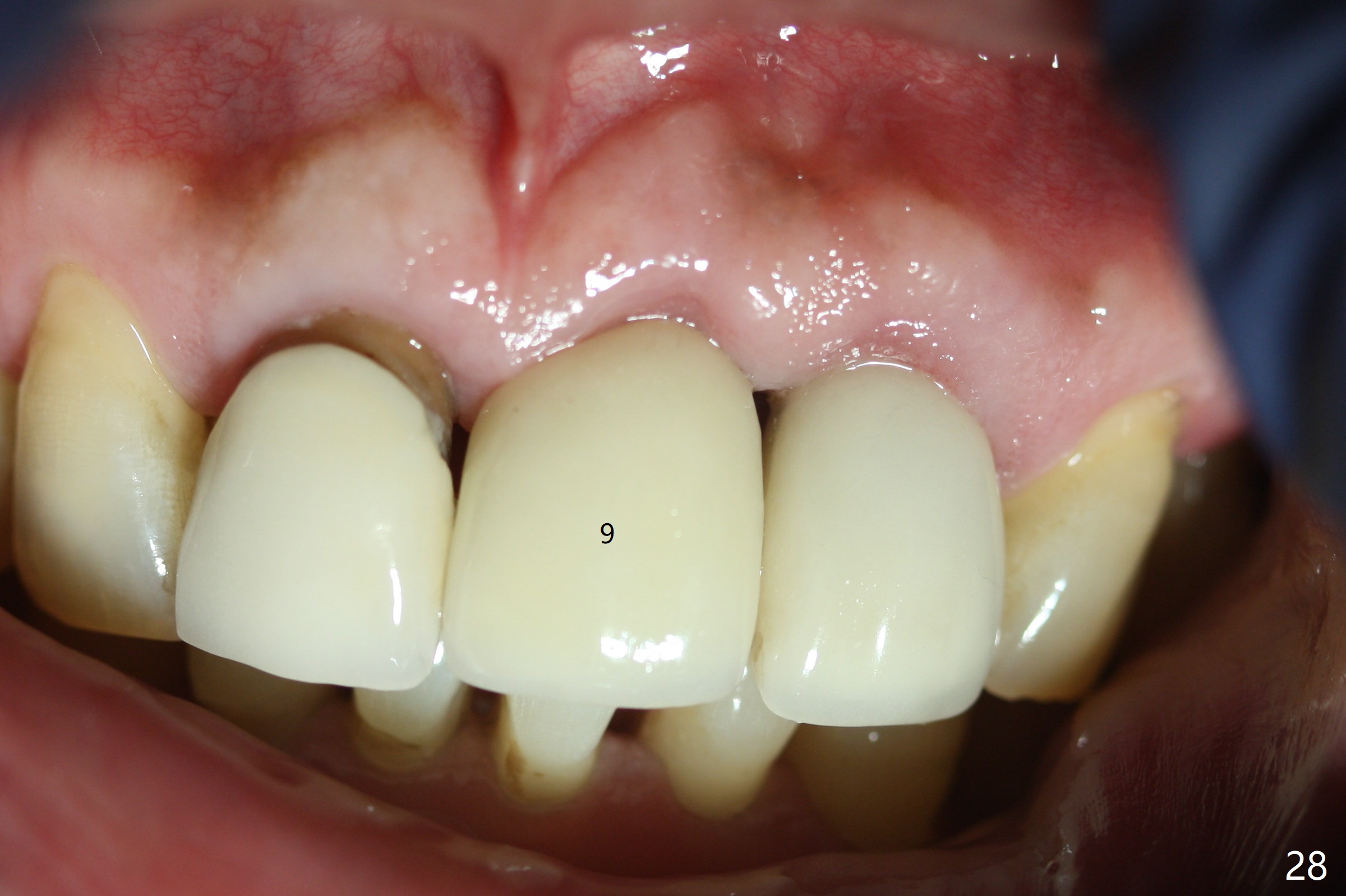
Six weeks postop, the gingival margin does not seem to migrate incisally (Fig.19). More labial reduction of the implant/abutment is finished before reline and recementation (Fig.20). Sixteen days later, the immediate provisional at #9 dislodges again. Although the gingival margins have not descended enough, the implants/abutments are re-prepared for final restoration (Fig.22-24), since there is no bone resorption around the implants (Fig.21, 8 weeks postop). The patient returns with porcelain chip at #9 mesiopalatally 2 years 10 months post cementation (Fig.25 *). The chip is due partially to the distally placed implant and partially to failure to extend zirconia coping mesially. When the crown at #9 is removed, the 3.5x5 mm existig abutment is loose. It is changed to a 4x5 mm one, which is then cemented and prepared (Fig.26). A PFM is made at #9 as the one at #8, while #10 crown remains to be porcelain-fused-Zirconium, in which the implant placement is within normal limit (Fig.27,28).
Return to
Upper Incisor
Immediate Implants,
Technician
Xin Wei, DDS, PhD, MS 1st edition 06/01/2015, last revision 12/24/2018