 |
 |
 |
|
 |
 |
 |
 |
 |
 |
 |
|
 |
 |
 |
|
 |
 |
 |
|
Fibrointegration and Immediate Correction
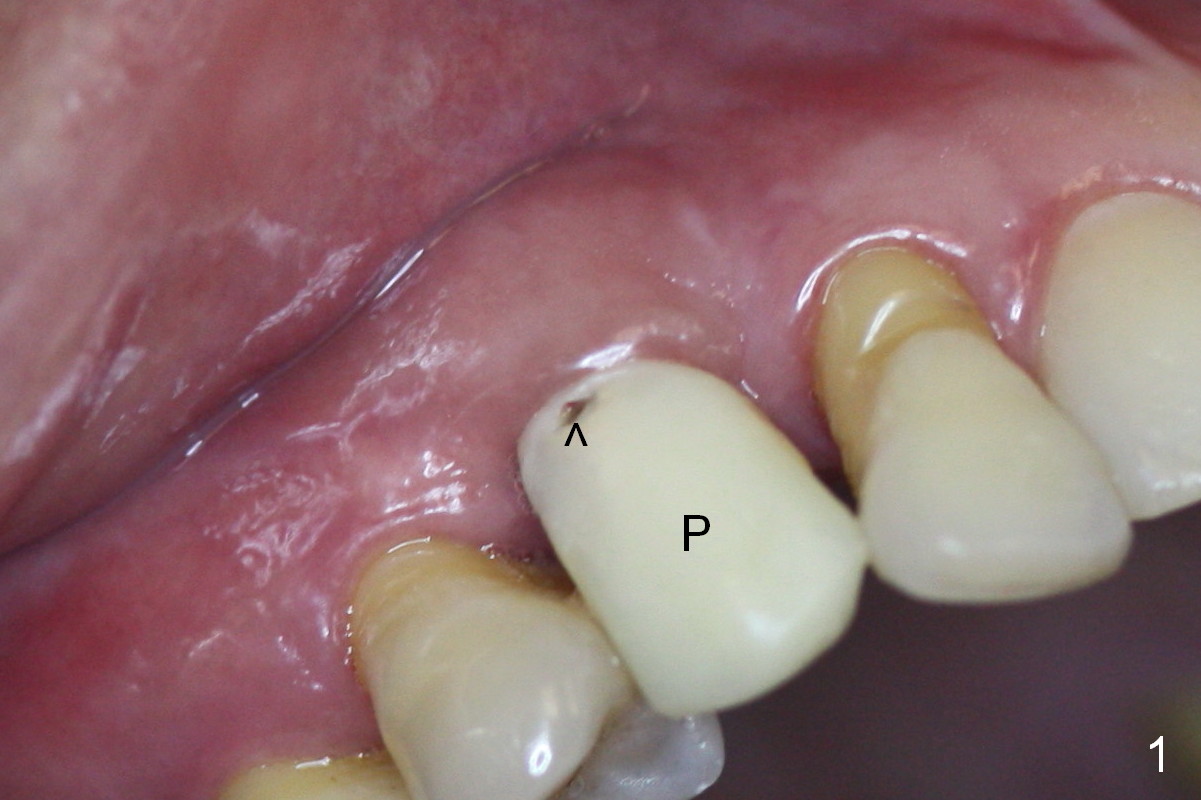
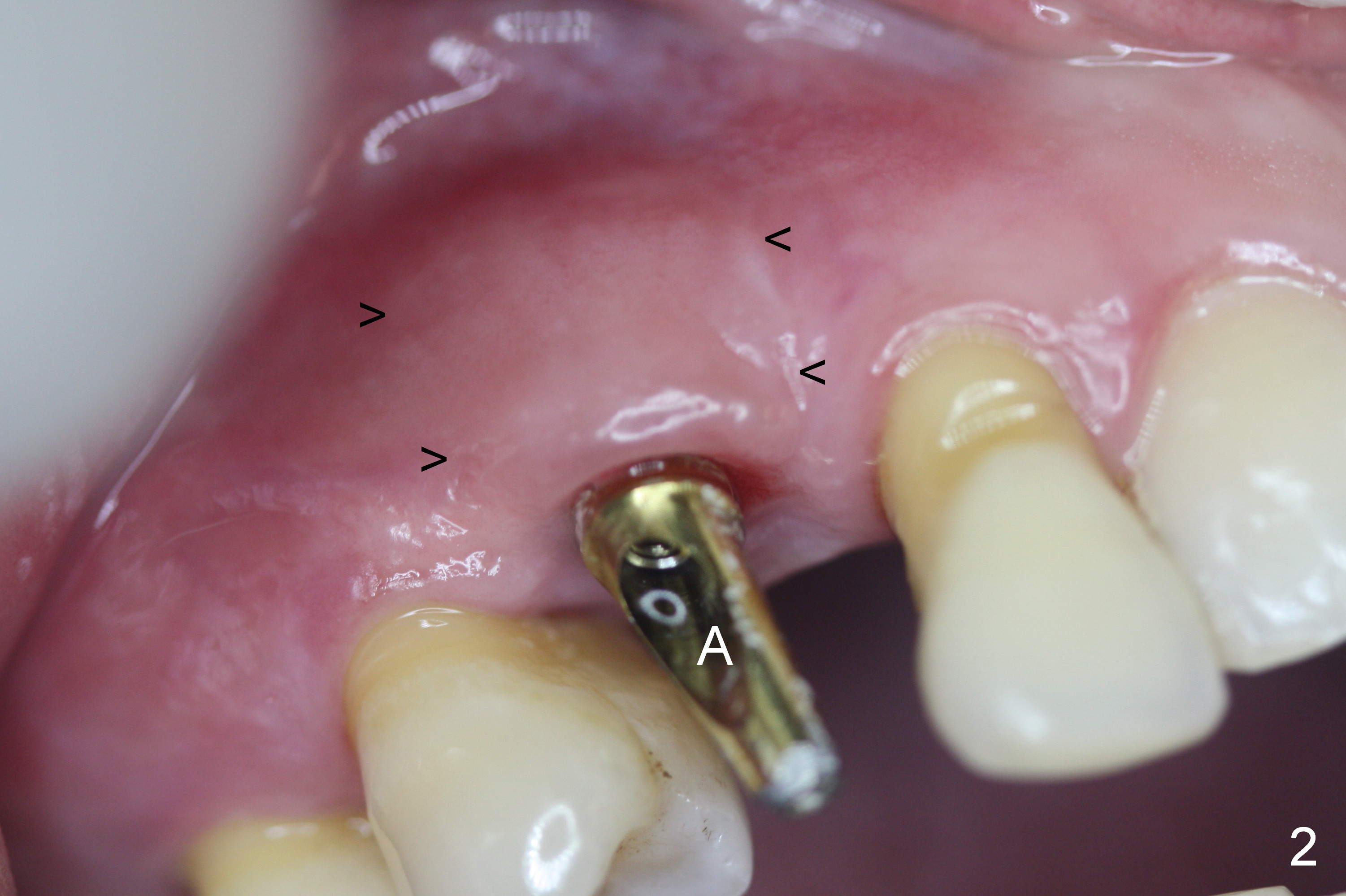
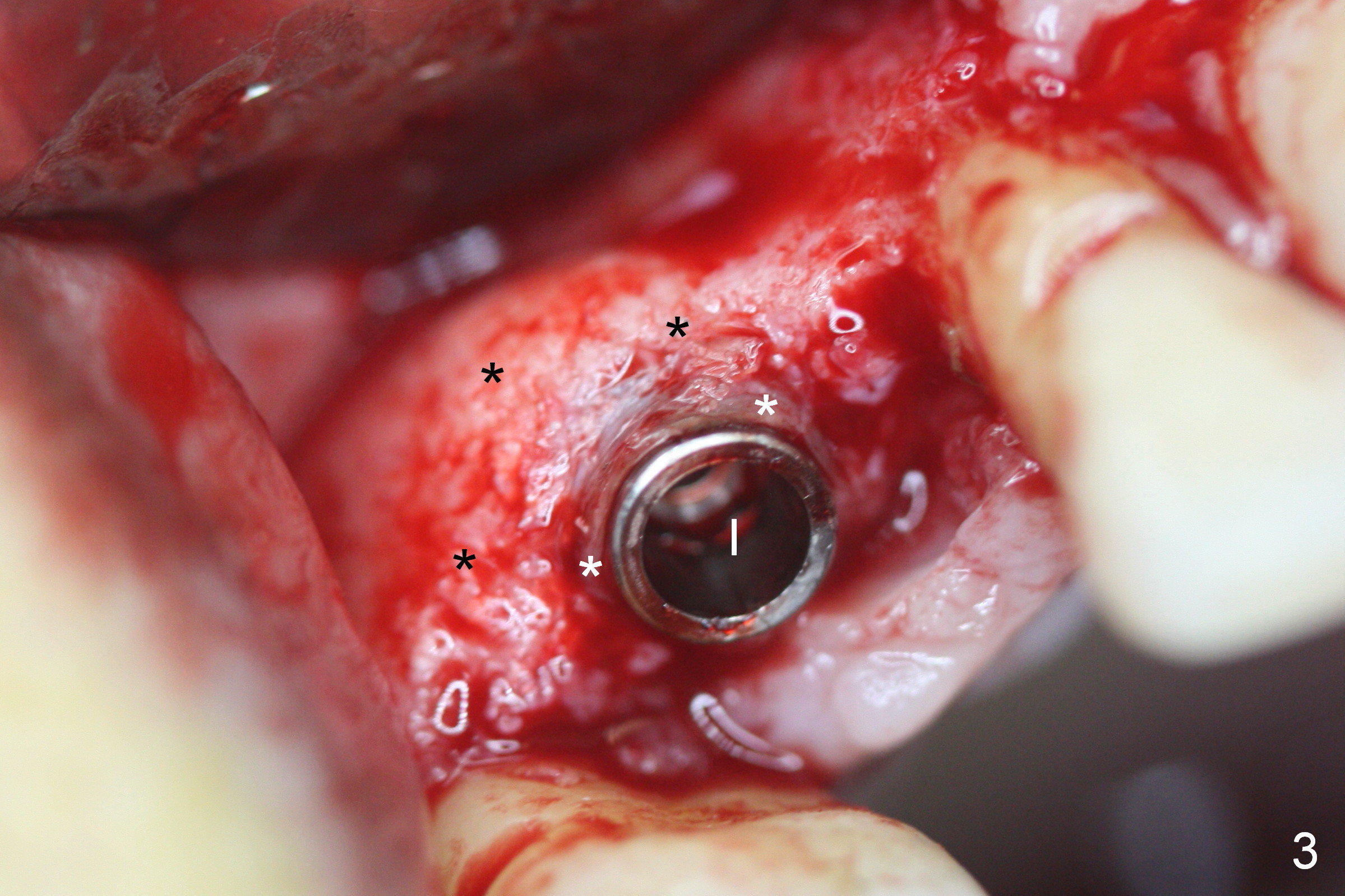
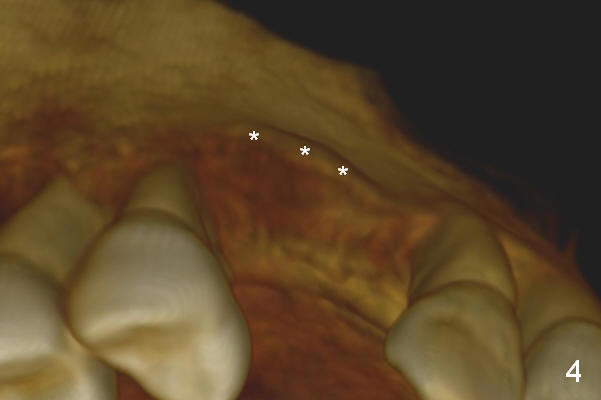
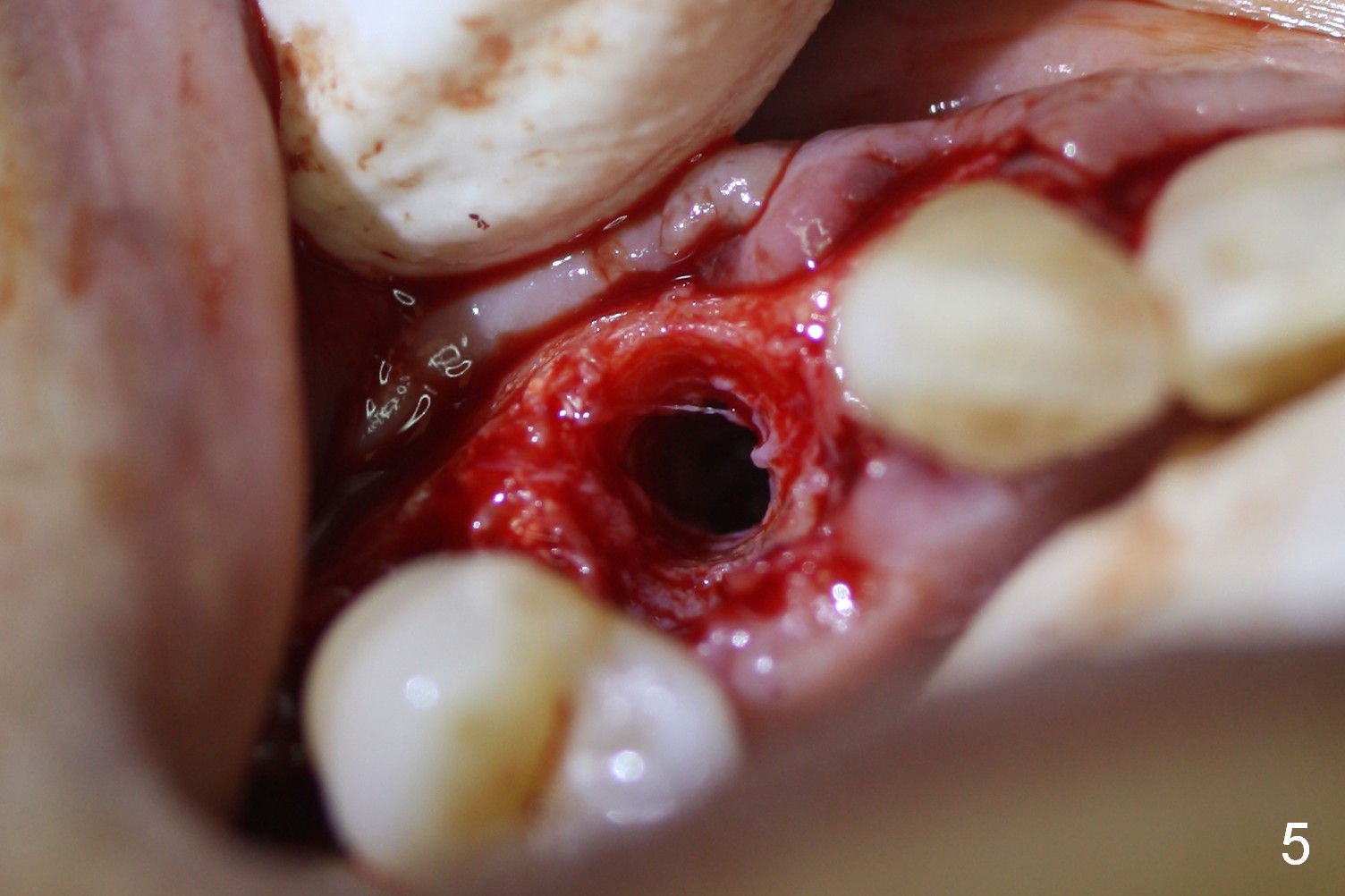
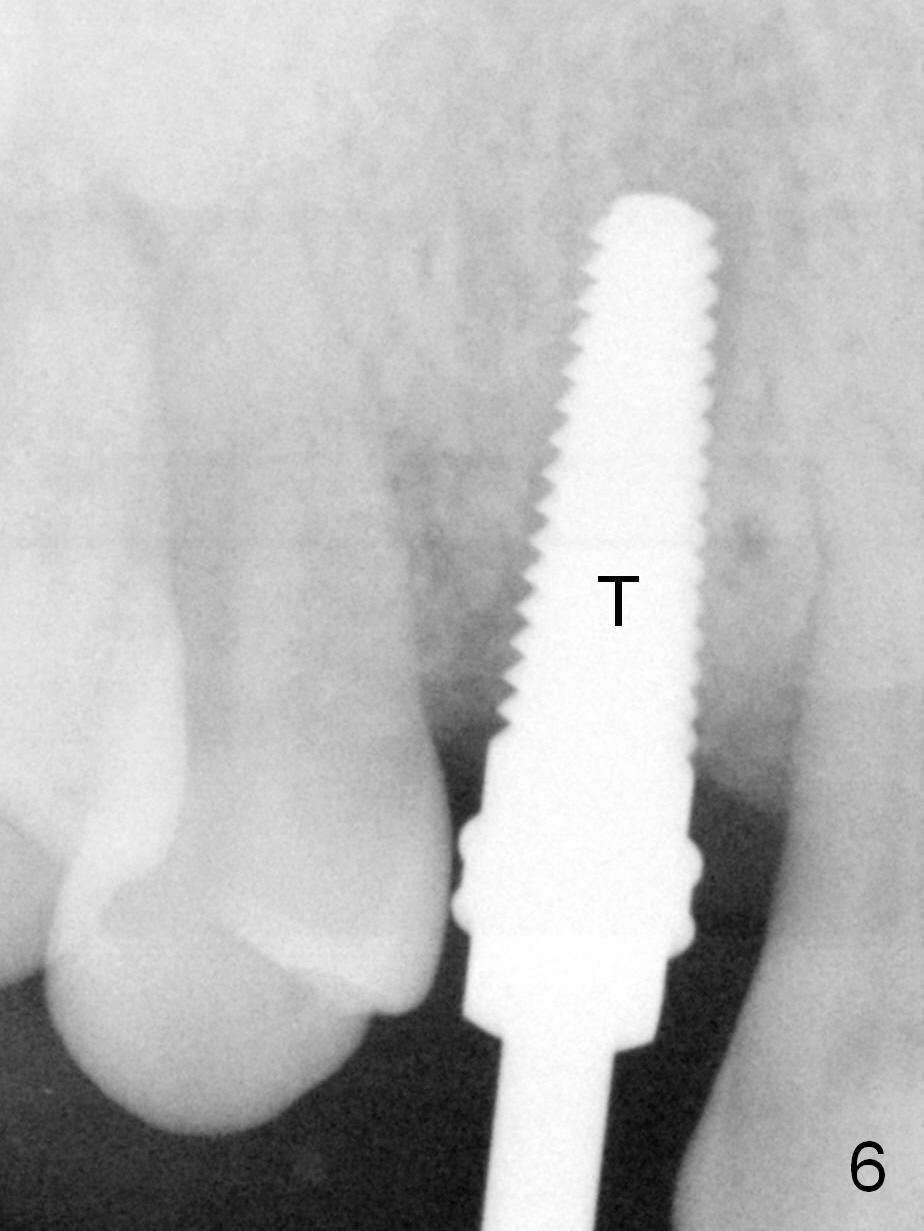
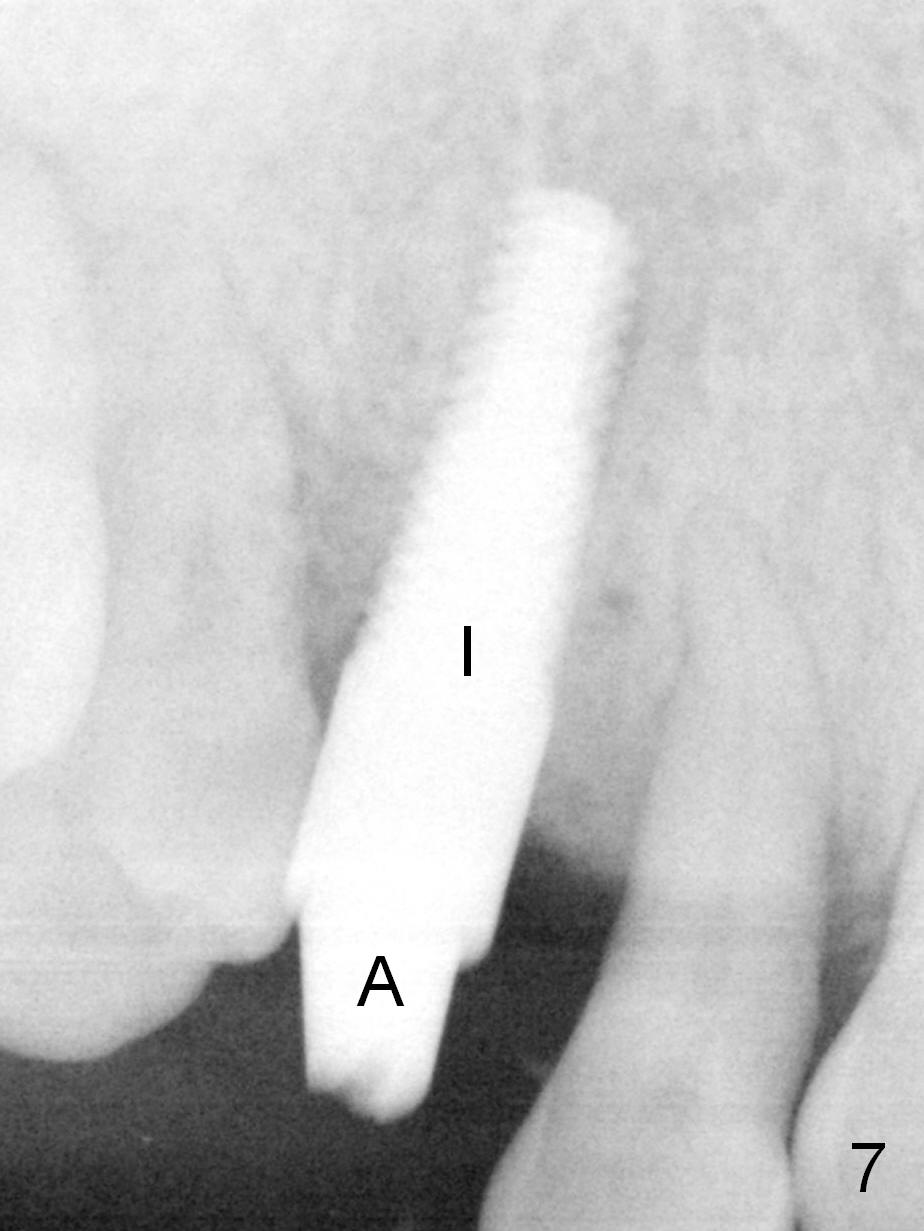
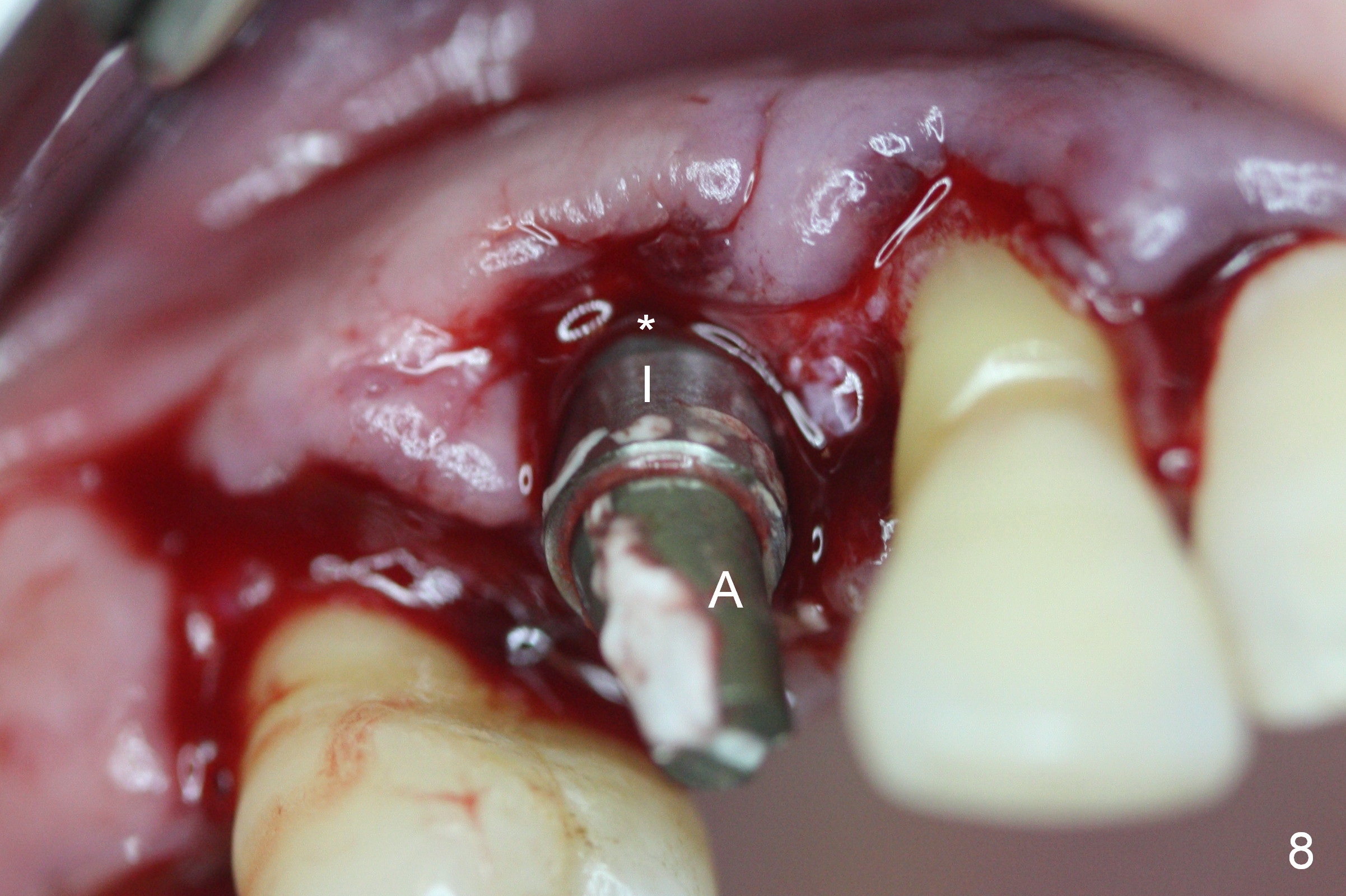
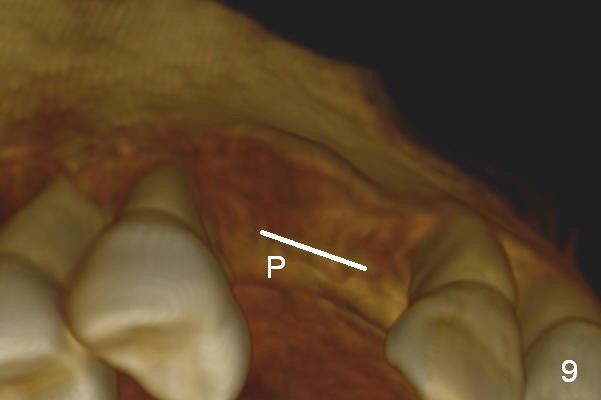
Four months post implant placement, the immediate provisional (Fig.1 P) has mobility with tenderness and perforation at the cervix (^). When the provisional is removed, the buccal plate bulging is more evident (Fig.2 arrowheads). The latter is apparently caused by bone expansion associated with implant placement (Fig.3 black *), since the bulging is not so obvious in a preop CBCT 3 D image (Fig.4 *). There is a layer of fiber granulation tissue (Fig.3 white *) around the mobile implant (I). More fiber tissue is noted when the implant is removed (Fig.5). A new osteotomy is created in the palatal wall of the existing implant site with 2 mm pilot drill, followed by 2.5 and 3 mm reamers. As a 4.5x17 mm tap is being inserted (Fig.6 T), it is deviated buccally. Reamers are re-used to try to remove more palatal bone to let the implant be placed more palatally. When a 4.5x17 mm tissue-level implant is placed (Fig.7,8 I with insertion torque >60 Ncm), there is a small buccal gap (Fig.8 *). A 20° angled abutment (Fig.7,8 A) is placed. An immediate provisional is fabricated with cosmetic satisfaction.
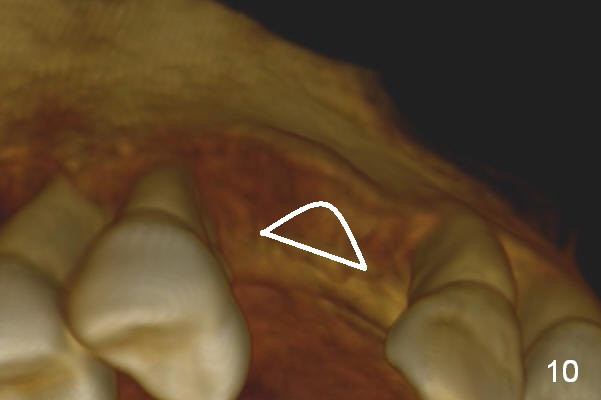
Retrospectively, bone expansion should have been initiated (Fig.9 white line) close to the thicker palatal plate (P). The coronal end of the osteotomes should have been directed palatally. It would be much better to use a D implant (Fig.10).
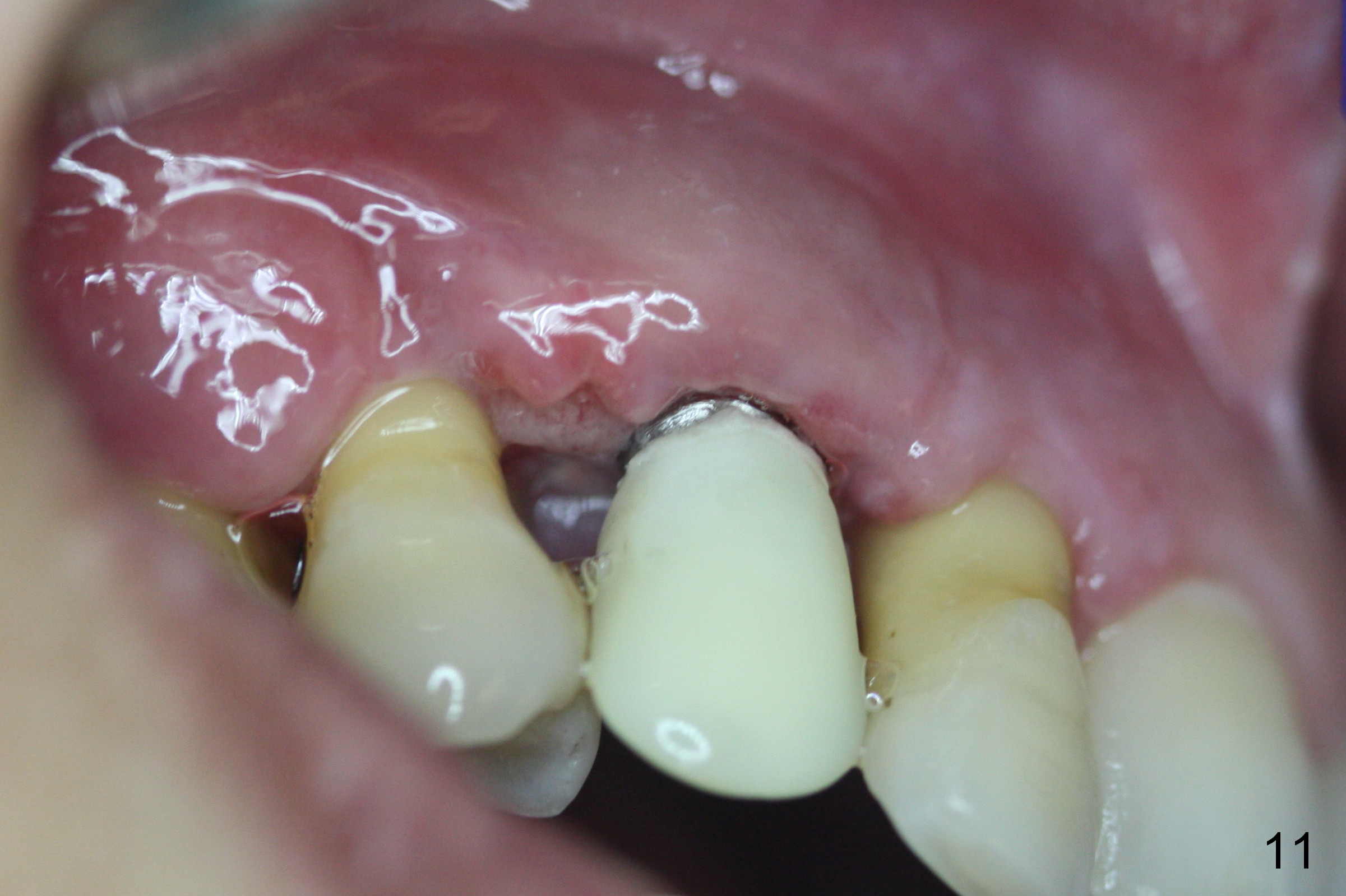
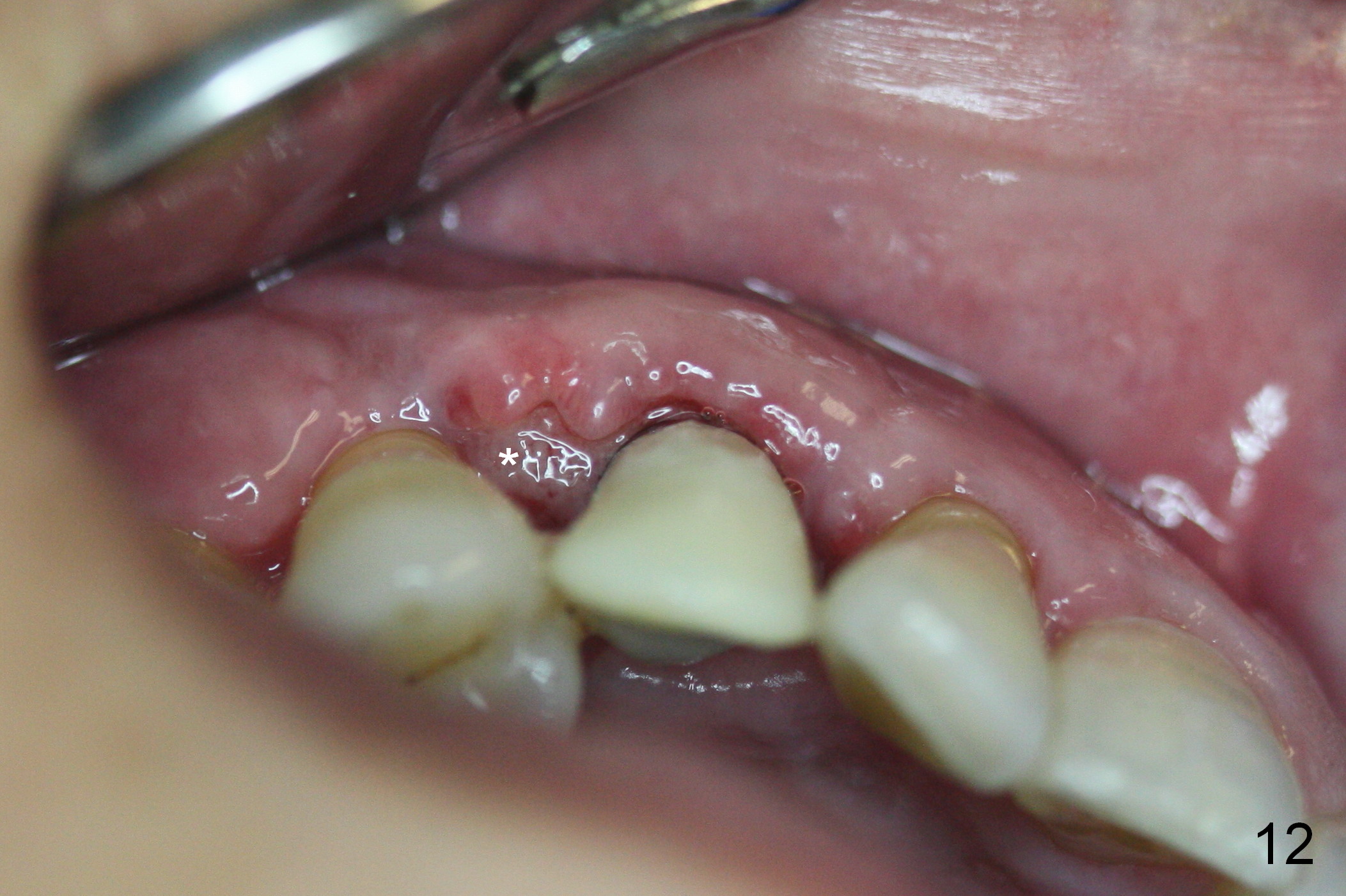
The patient complains of bad smell from the operative field 7 days postop. The wound is gapping with pseudo membrane, which is re-epithelized 14 days postop (Fig.11,12 *) with disappearance of the bad smell.
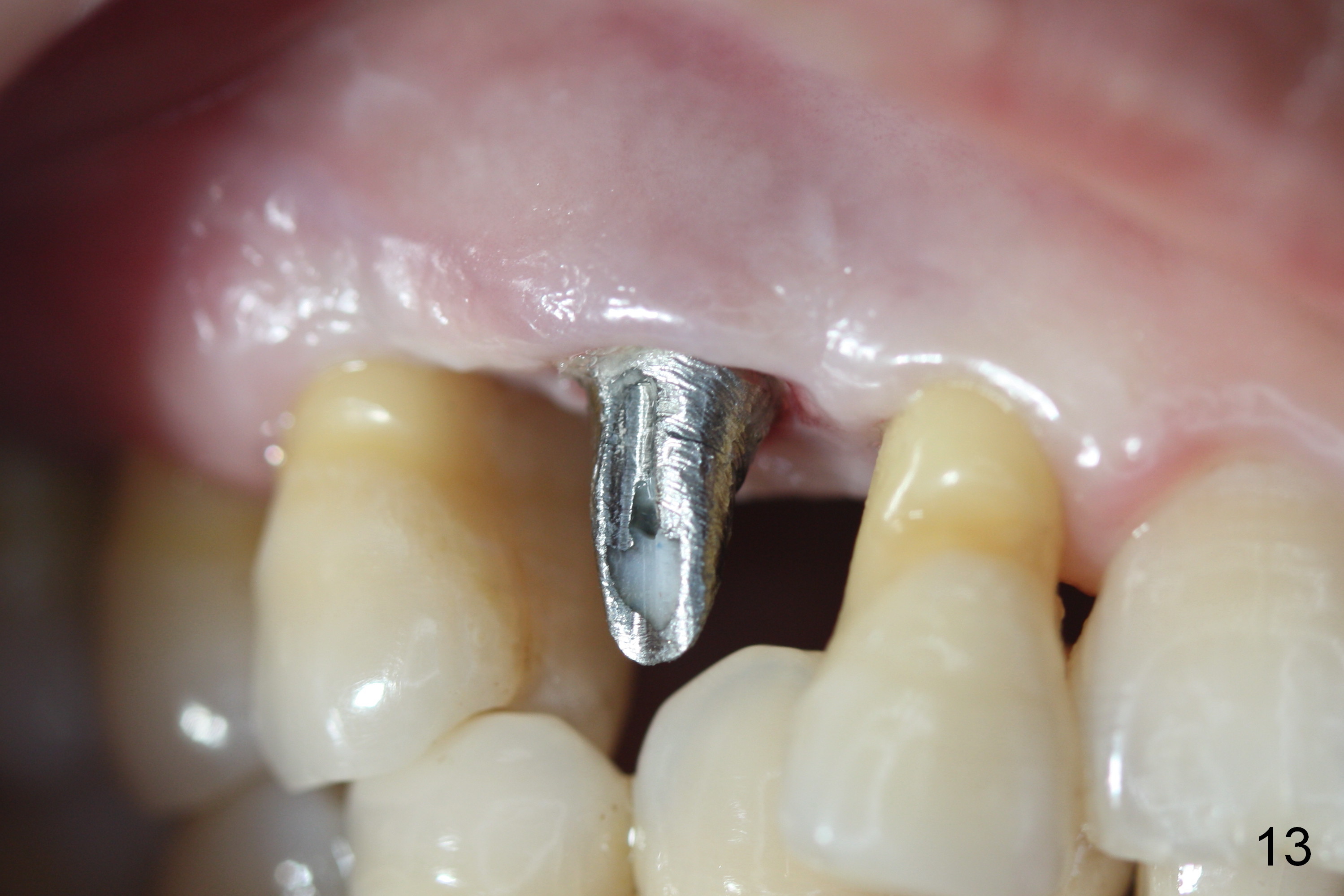
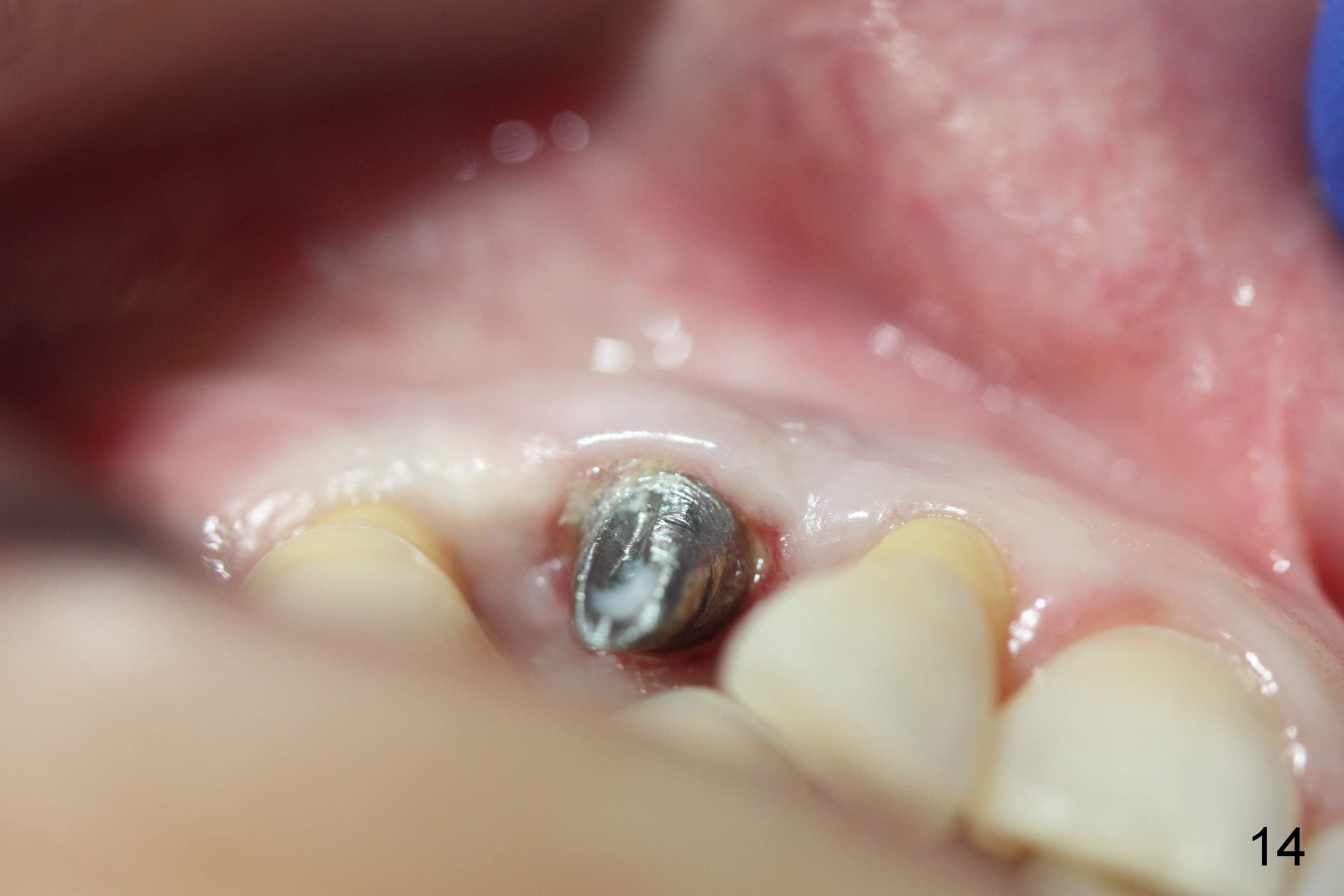
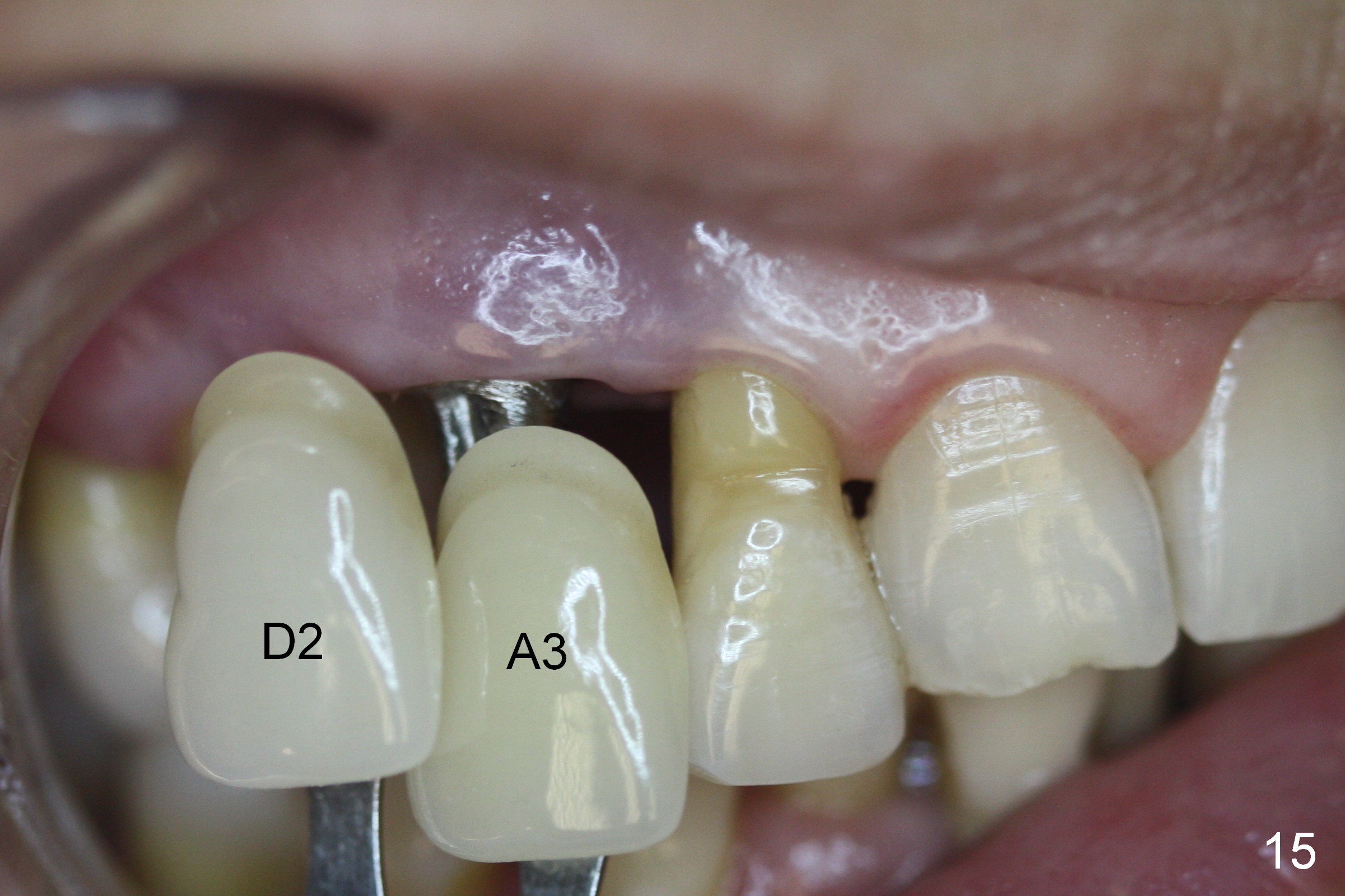
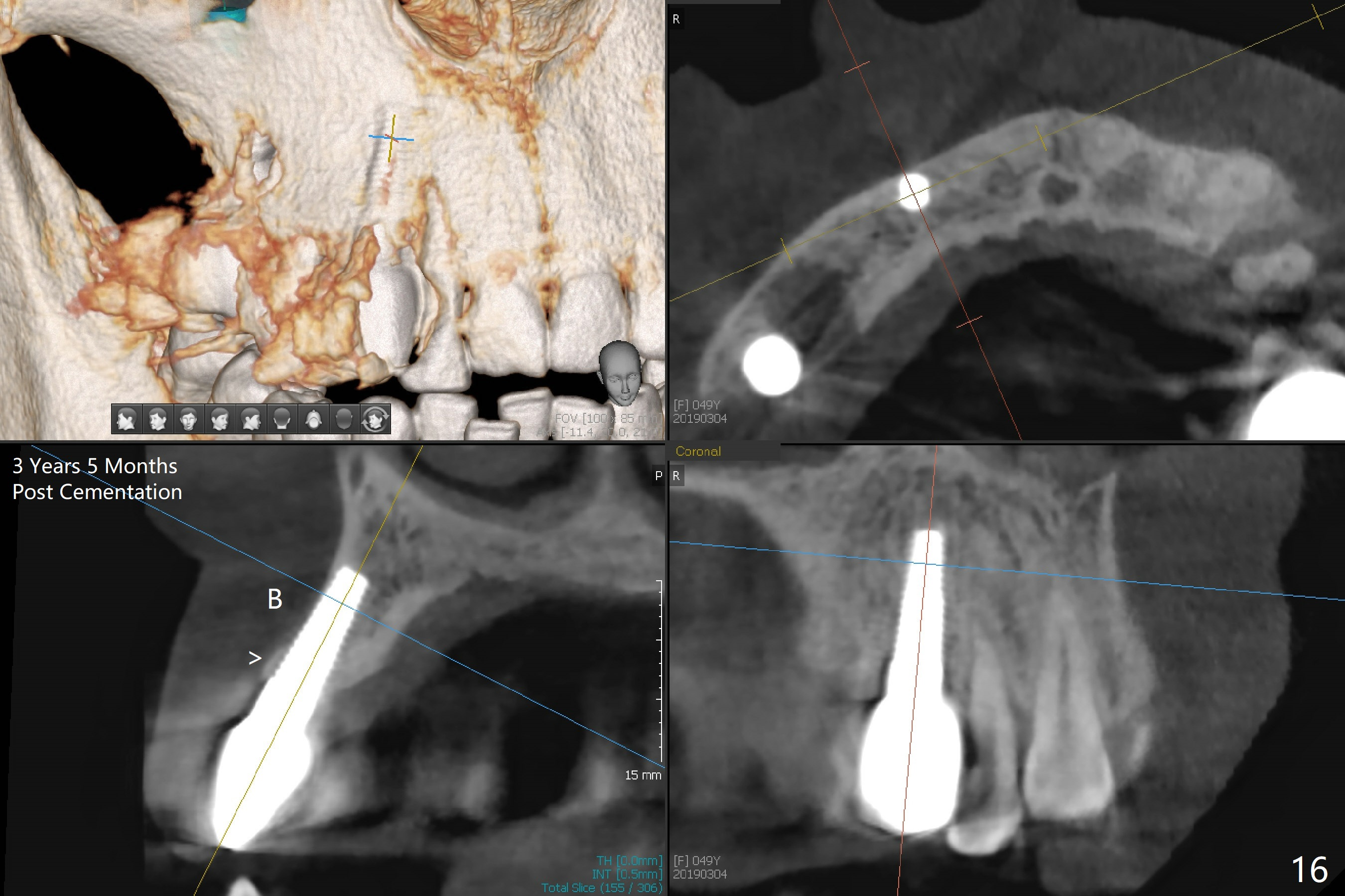
The gingiva is healthy 6 months postop (Fig.13) without buccal plate collapse (Fig.14). The implant and abutment have been prep for final restoration (Fig.15). Although the buccal plate is thin 3 years 5 months post cementation (Fig.16 B), the crest (>) is present, which accounts for no periimplantitis.
Return to Upper
Canine Immediate Implant,
Implant
Fails,
Dr.
Wu,
Technicians, #3,14
2
Xin Wei, DDS, PhD, MS 1st edition 03/24/2015, last revision 11/17/2019