 |
 |
 |
 |
|
 |
 |
 |
 |
|
 |
 |
 |
||
 |
 |
 |
||
 |
 |
 |
 |
|
 |
 |
 |
||
 |
 |
 |
||
Tripod Septum
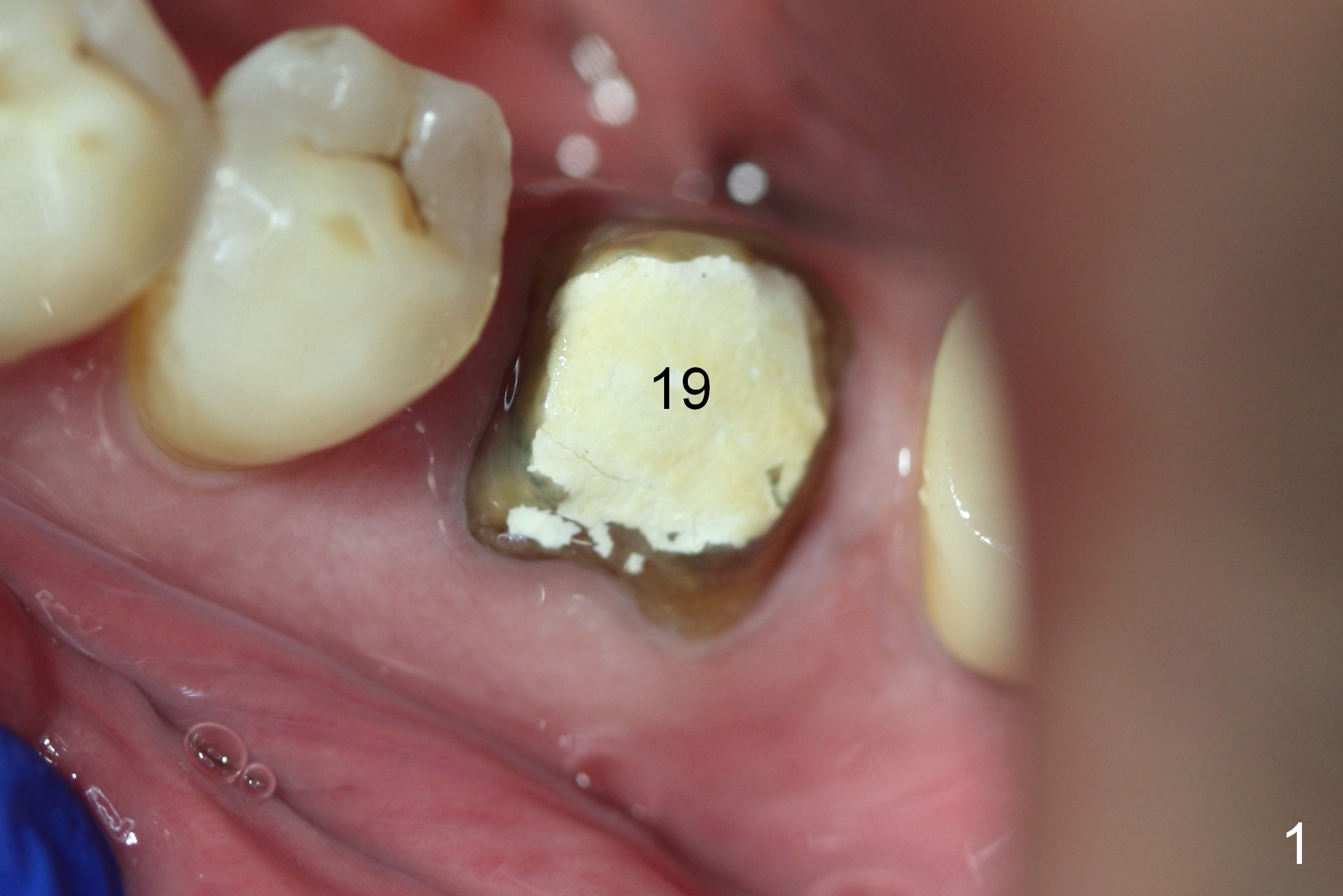
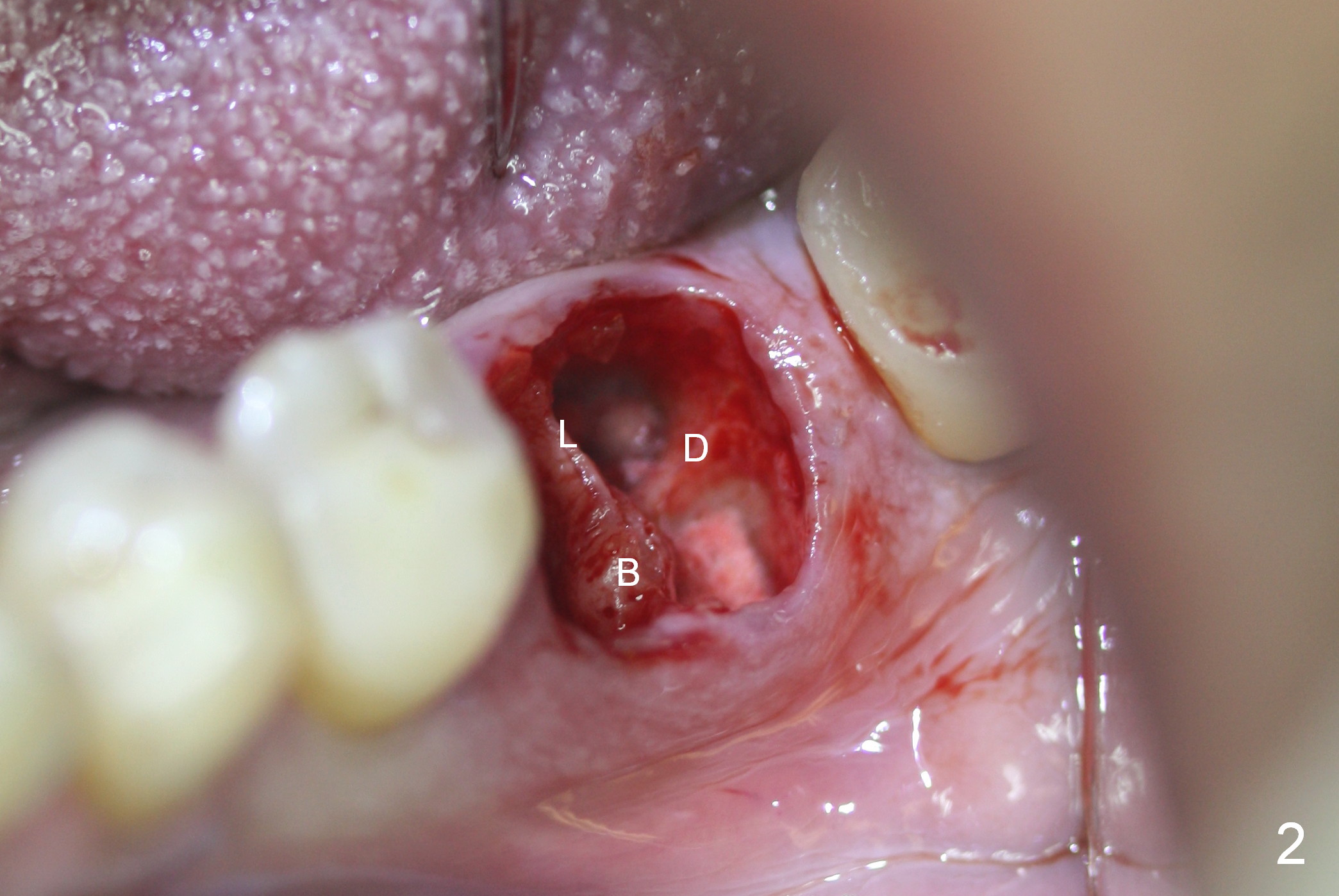
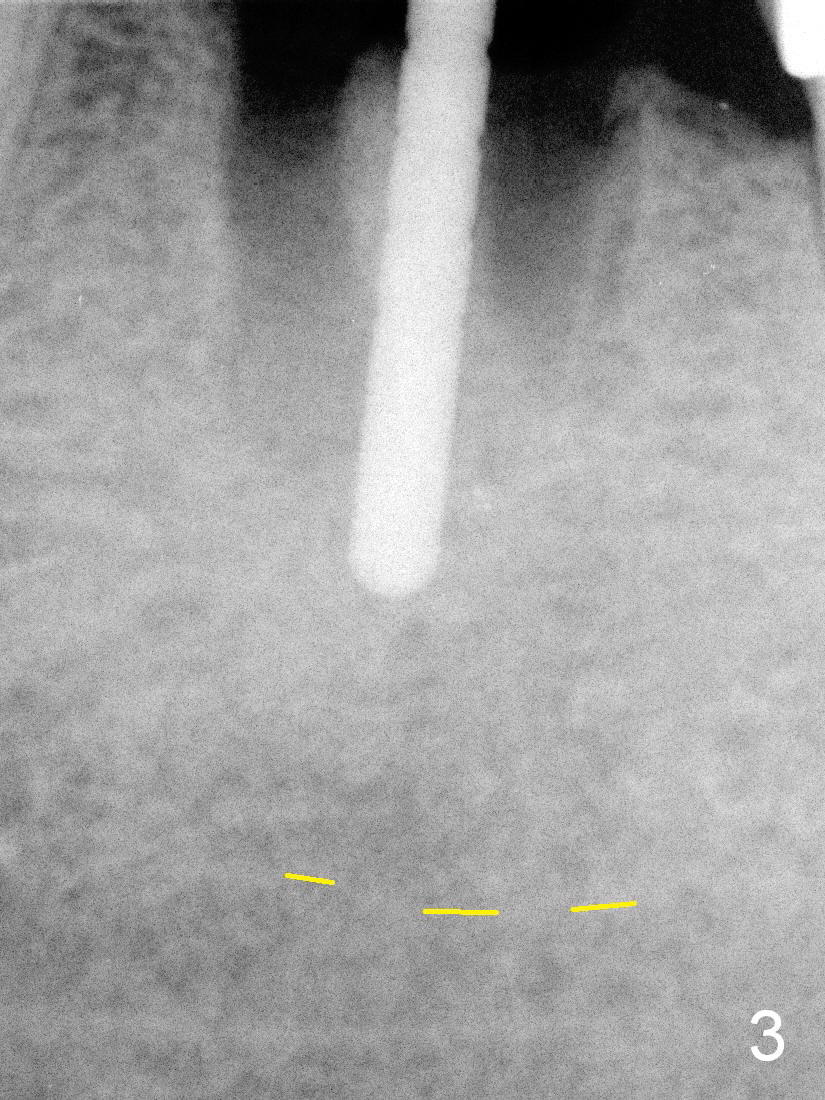
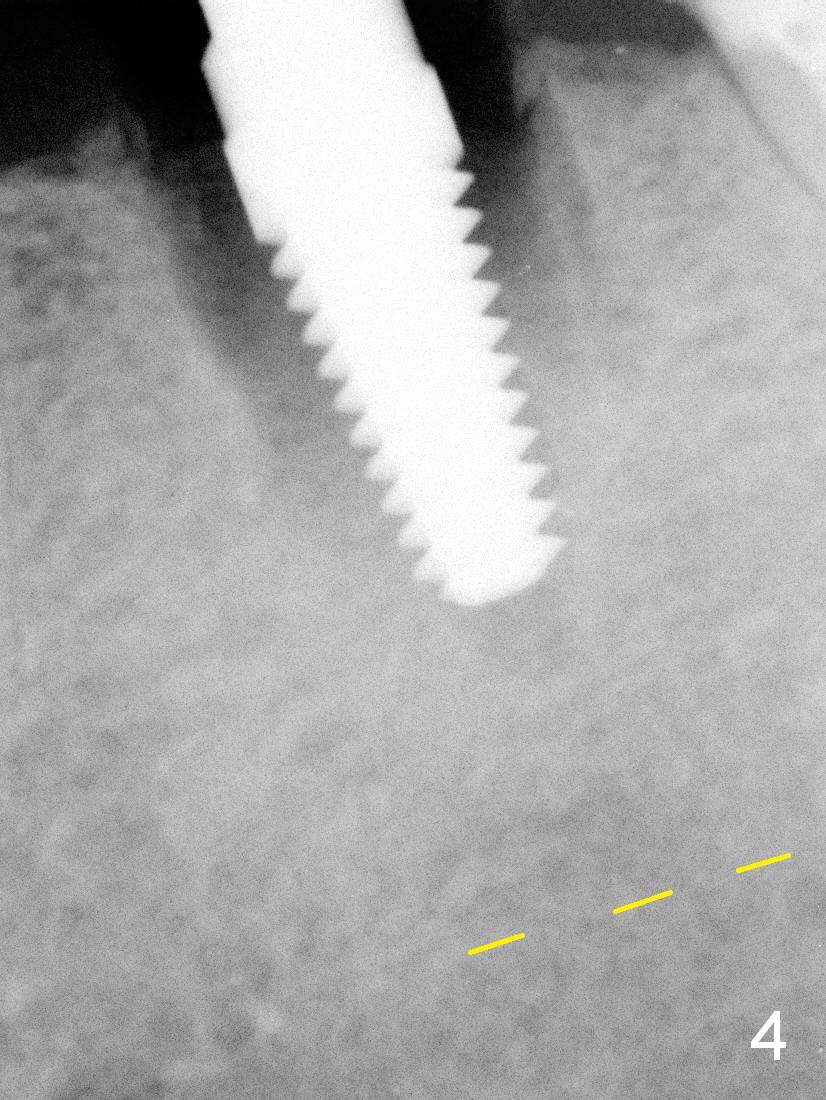
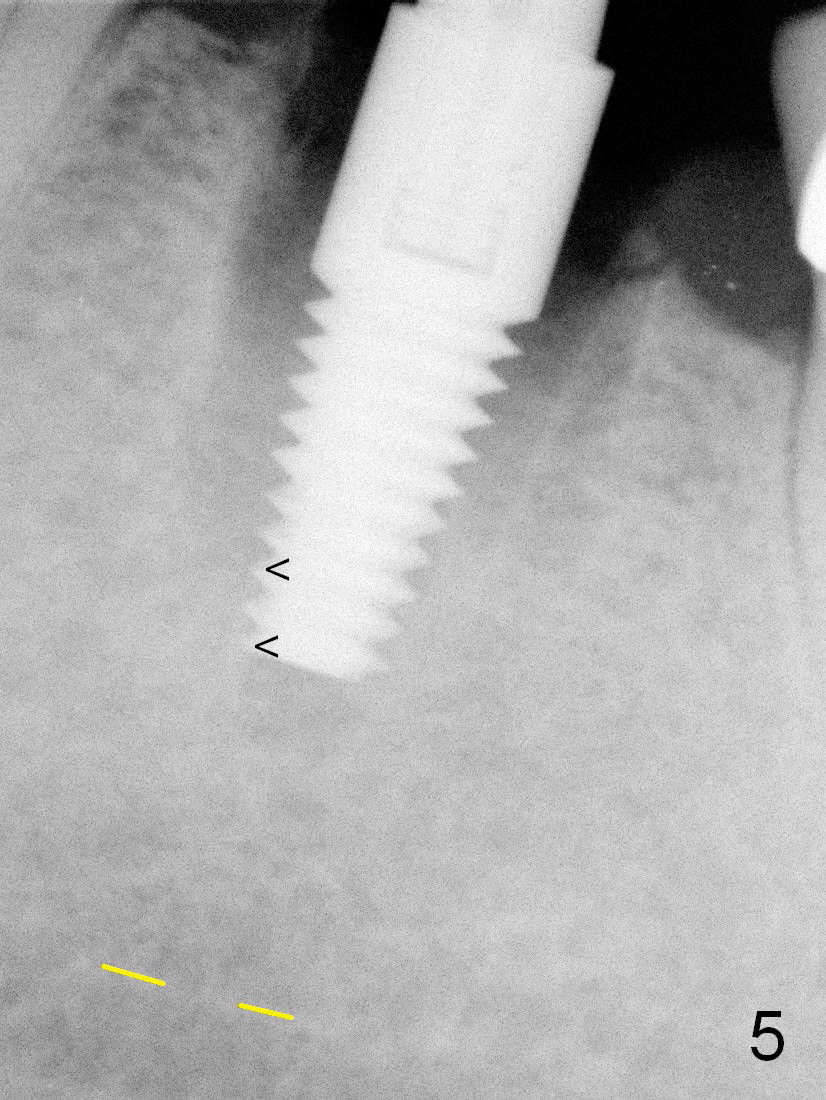
The ridge of the tooth #19 appears wide buccolingually; the immediate implant can be large (Fig.1). As predicted from the preop X-ray, there are 2 distal roots. Furthermore, all of the 3 roots are large; therefore the septum is relatively thin with tripods (3 septal struts: buccal (B), lingual (L) and distal (D) in Fig.2). Osteotomy is initiated in the tripod convergence area. The initial trajectory needs to be adjusted (Fig.3); there is a large margin of safety related to the Inferior Alveolar Nerve (IAN, yellow dashed line). When a 5x14 mm tap is being inserted (Fig.4), it tends to deviate mesially due to the presence of the distal strut. An increase in the diameter of osteotomy may lead to further deviation and a poor axis of the implant. For this reason, a 5x14 mm tissue-level implant is placed (Fig.5, with insertion torque >60 Ncm); the implant is approximately 7 mm from IAN.
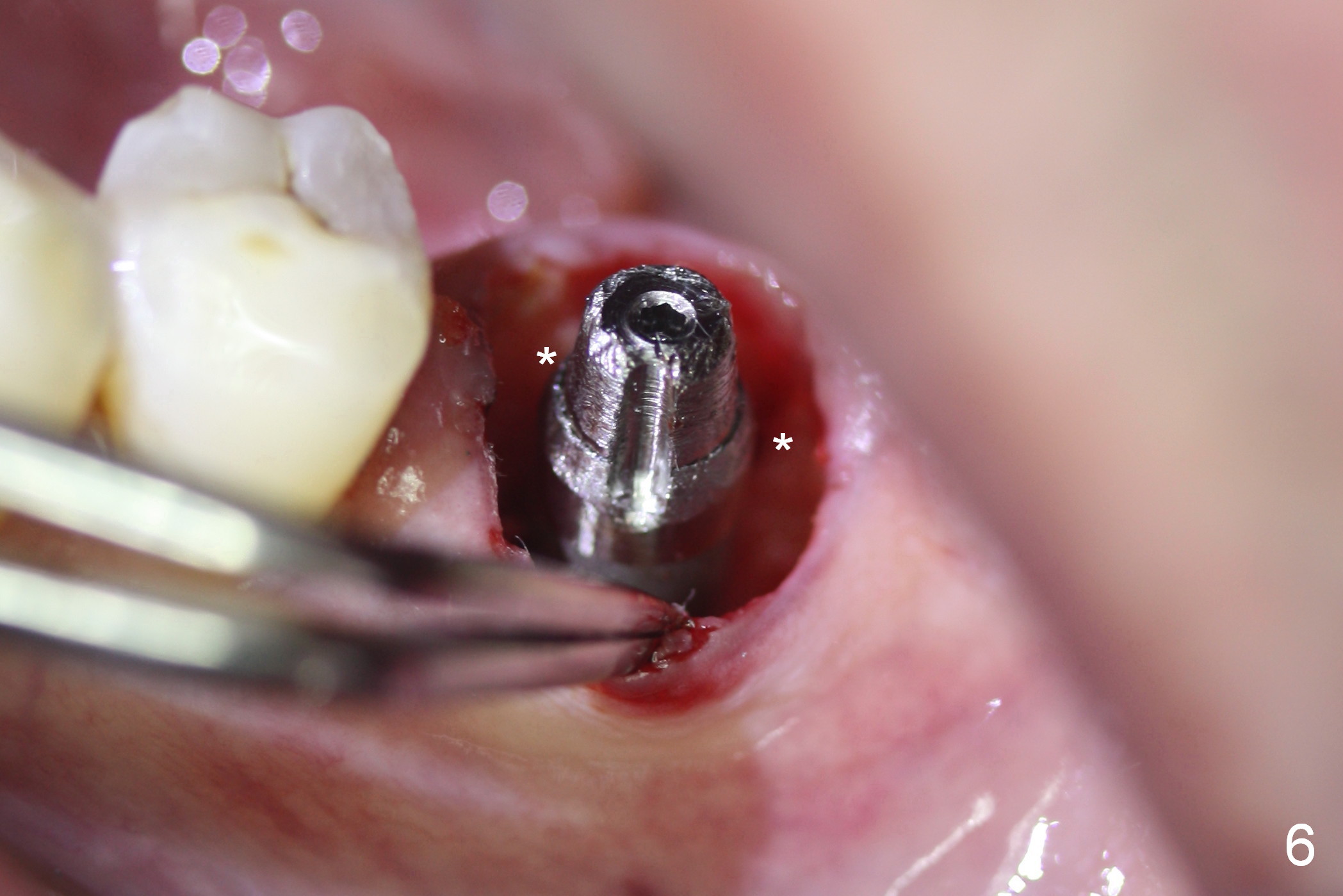
In fact the stability of the implant is due to engagement into the septal tripods coronally (Fig.6 *; the 3rd one behind the forceps) and into the new bone apically (Fig.5 arrowheads). A short implant can be stable and safe at the same time.
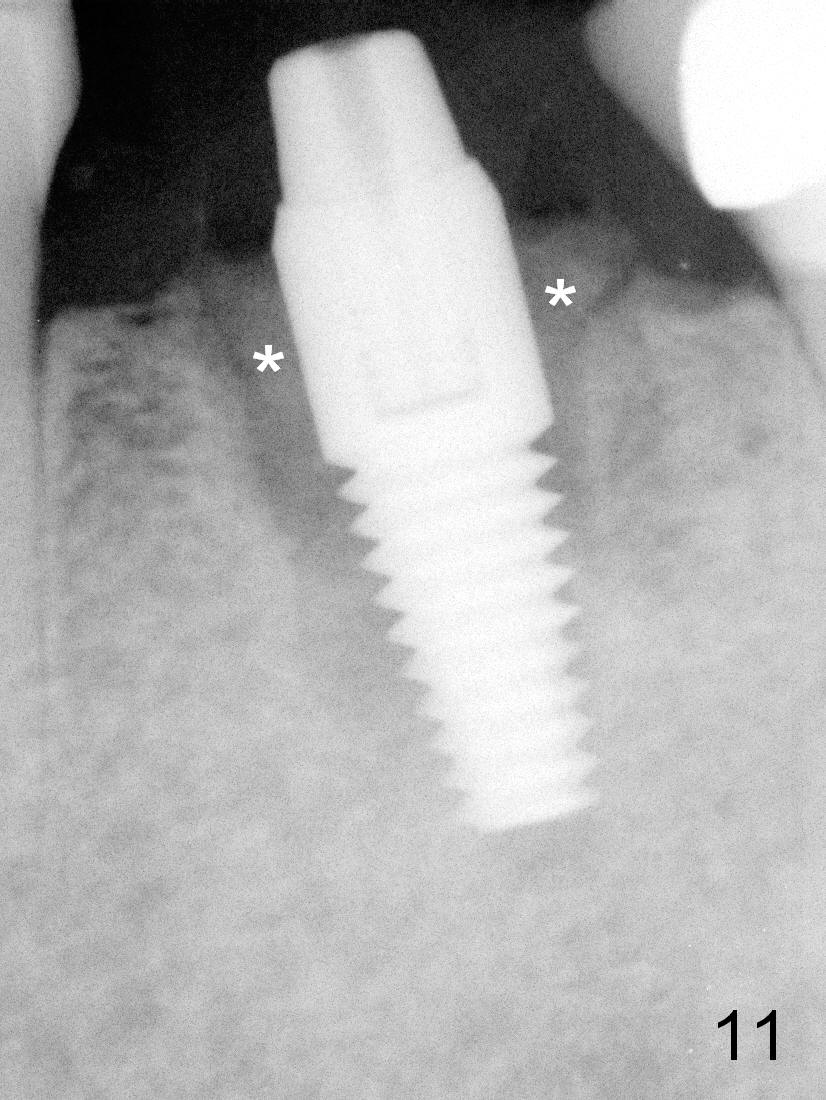
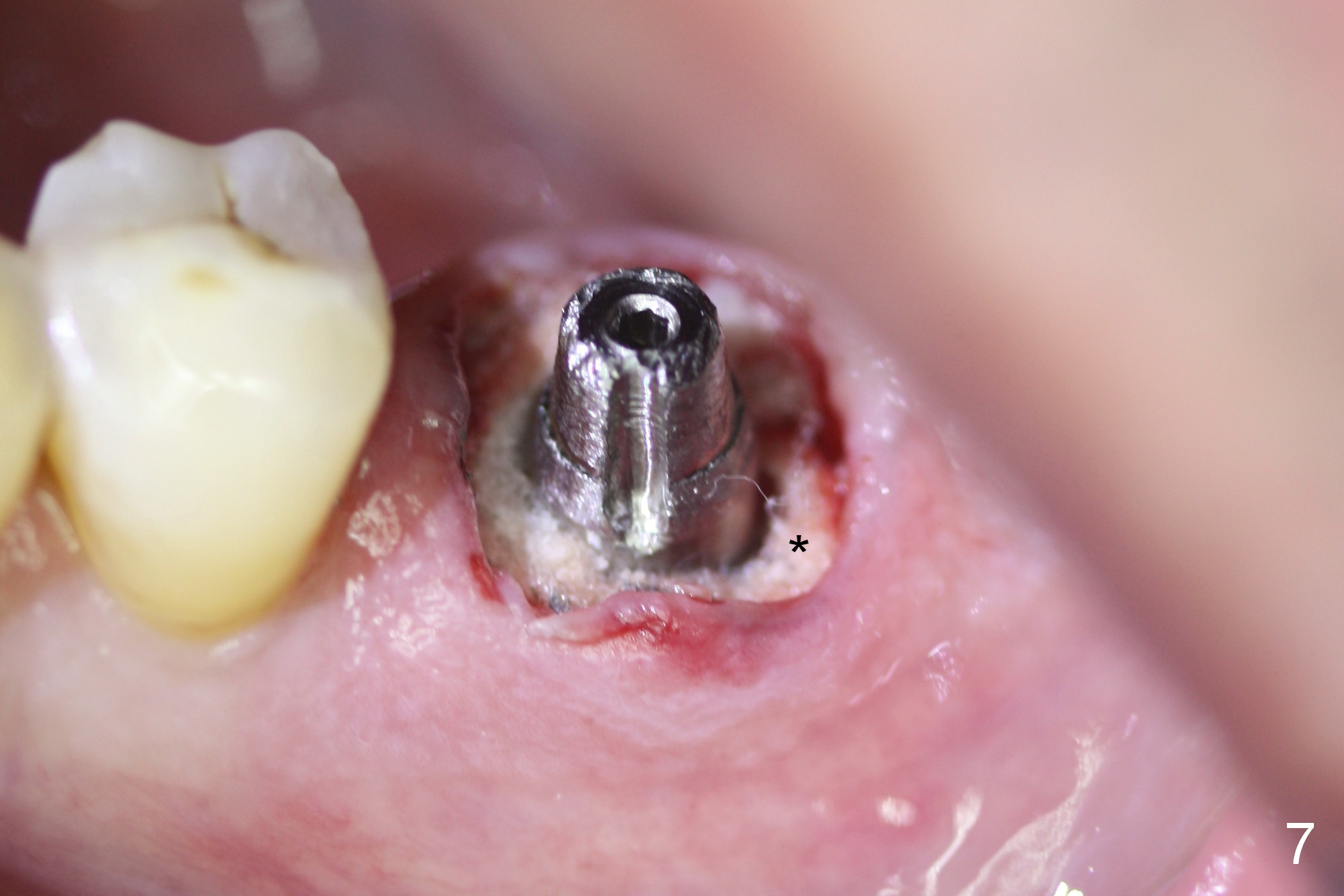
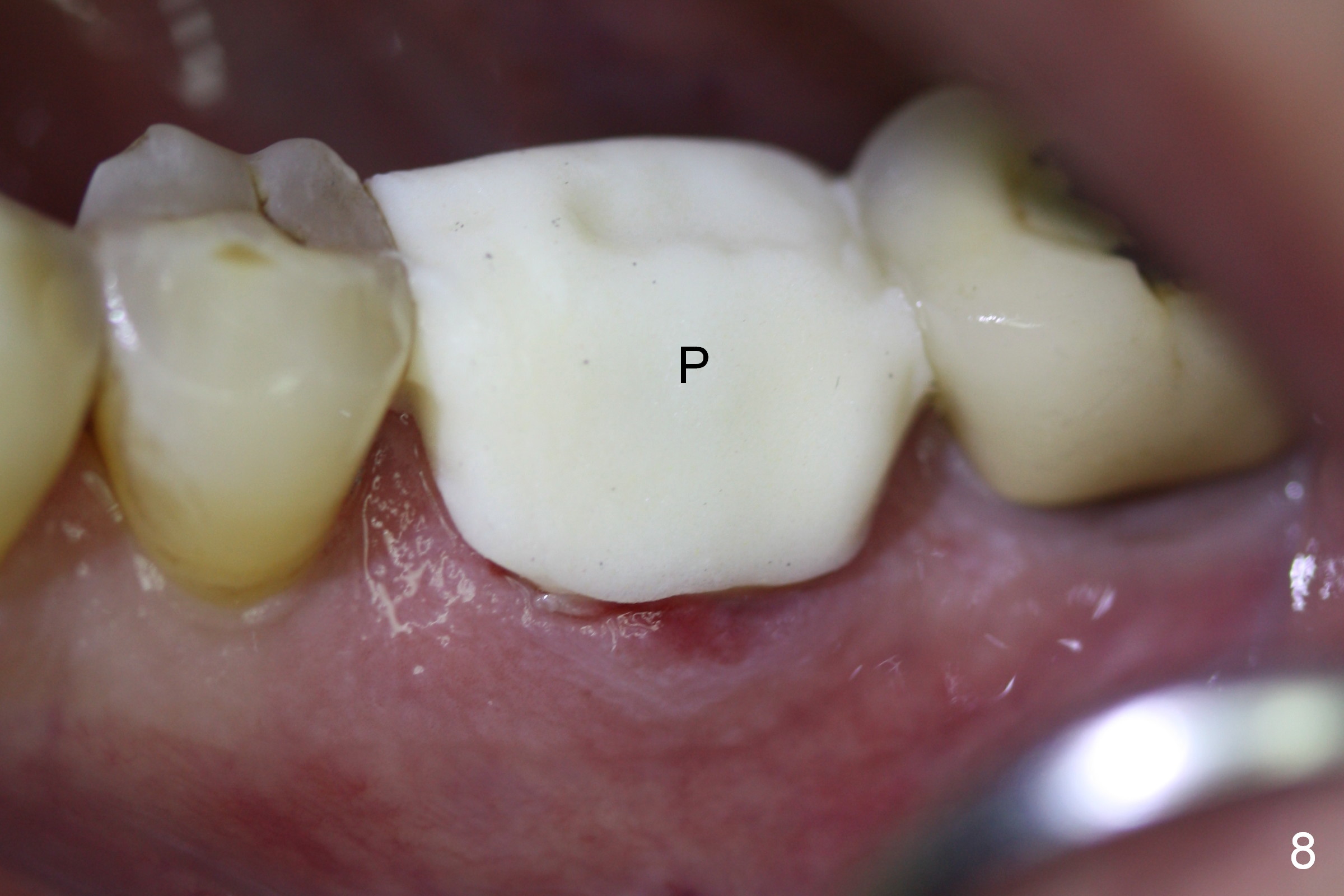
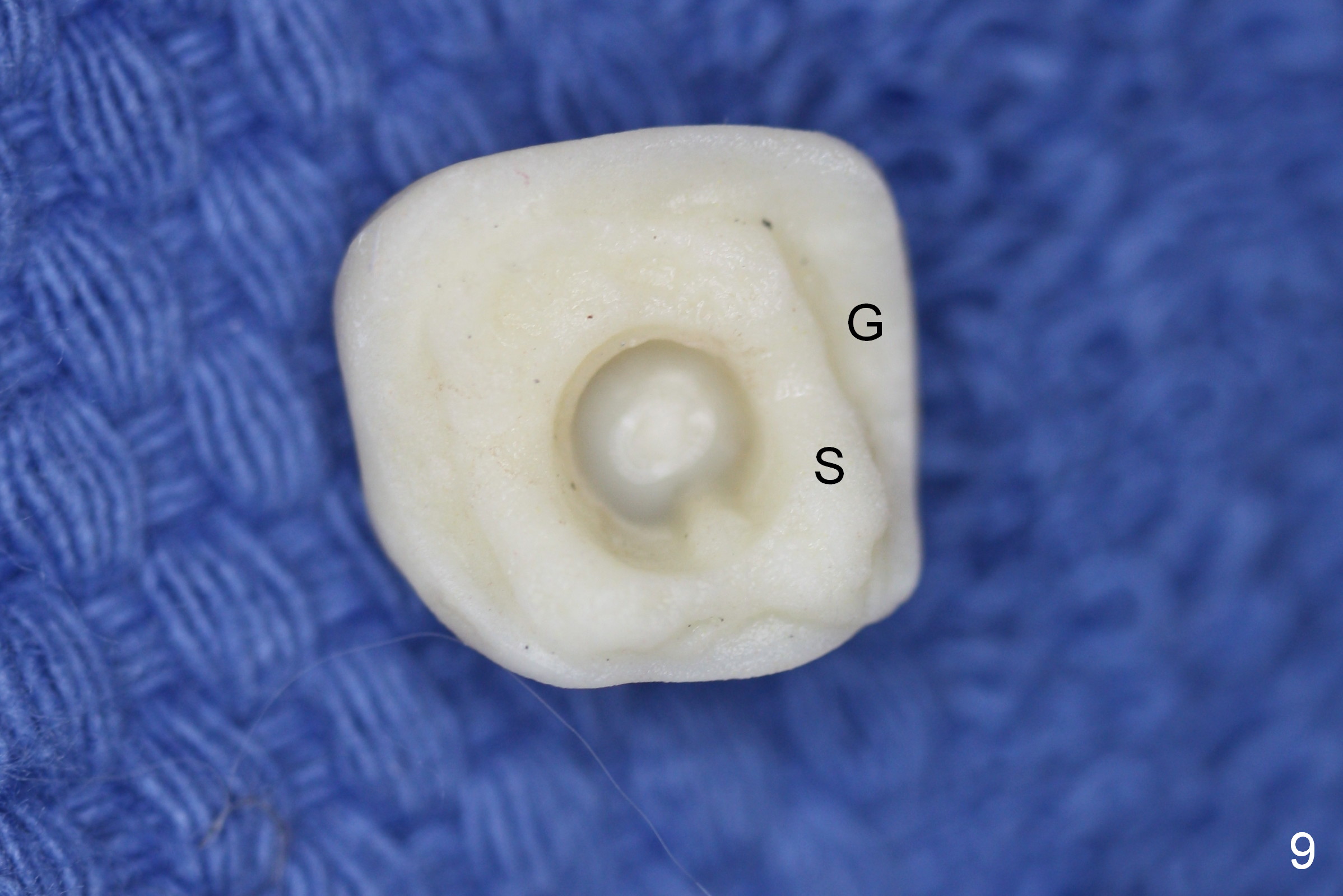
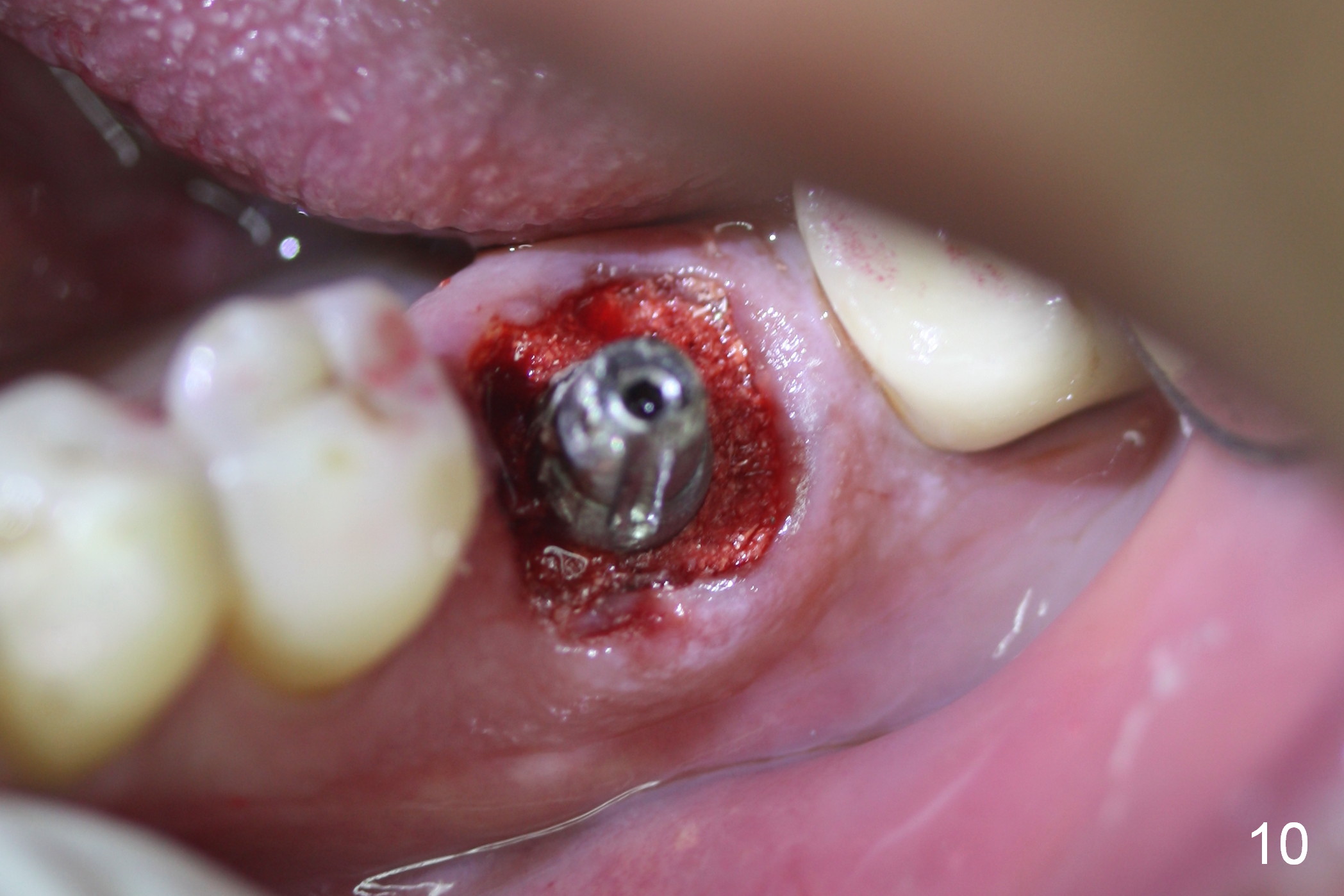
To fabricated an immediate provisional (Fig.8), a piece of unwoven gauze is inserted into the peri-implant gap (Fig.7 *), simulating bone graft level (Fig.10). The inner side of the provisional consists of 2 parts (Fig.9): corresponding to the socket gap (S) and the gingiva (G). This structure allows the provisional to close the socket securely (Fig.8) and prevent loss of the graft granules (Fig.11 *).
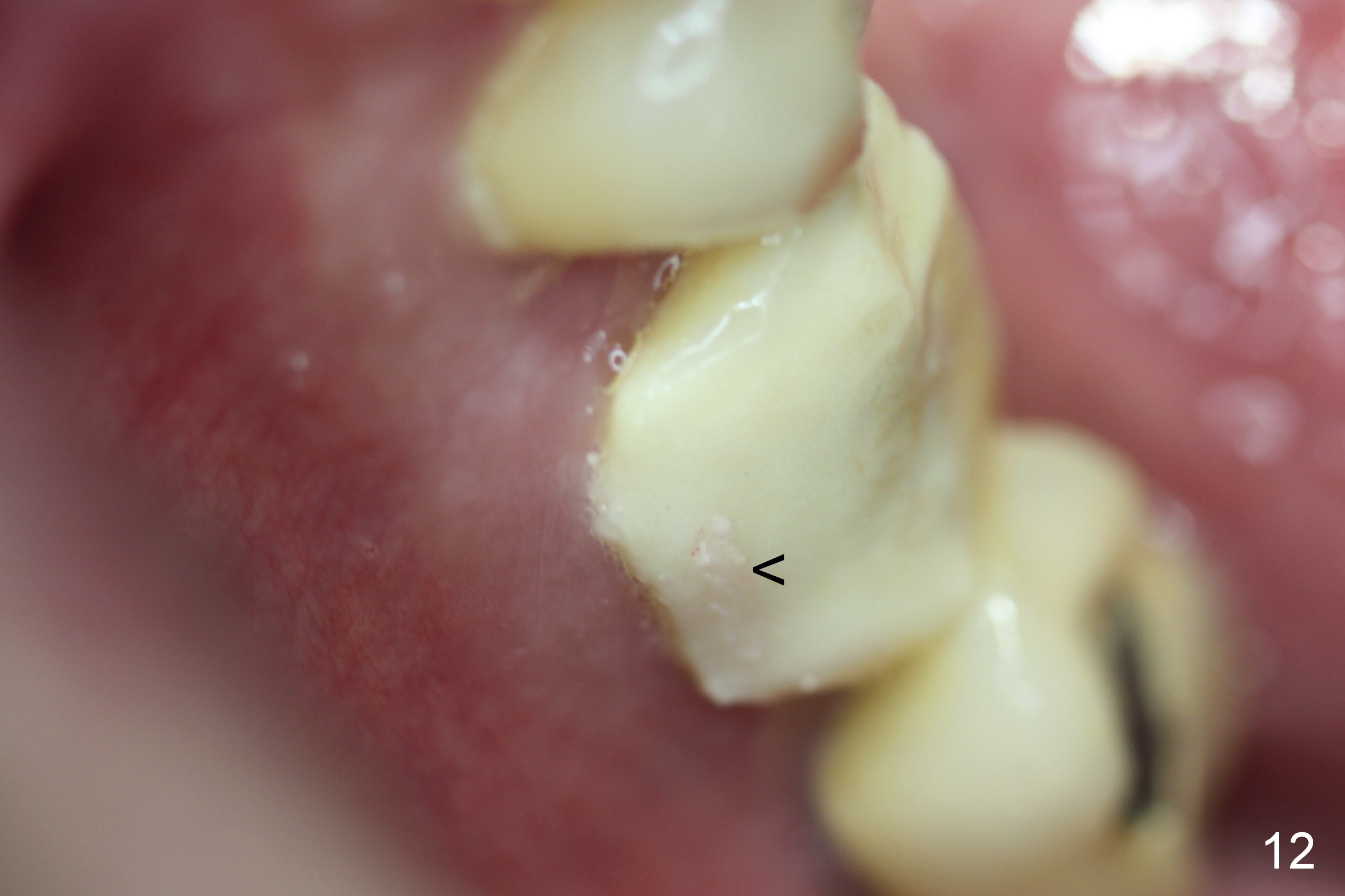
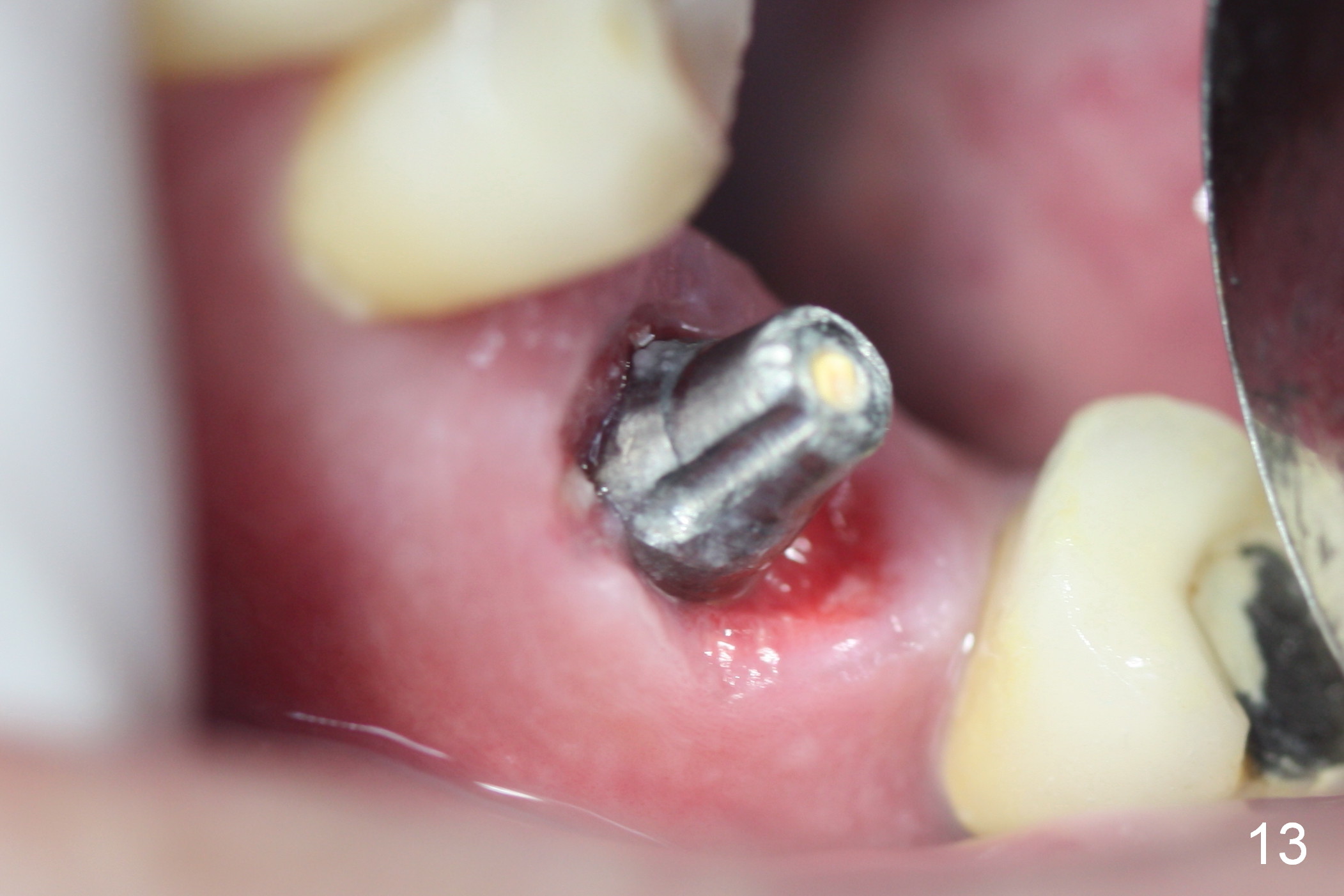
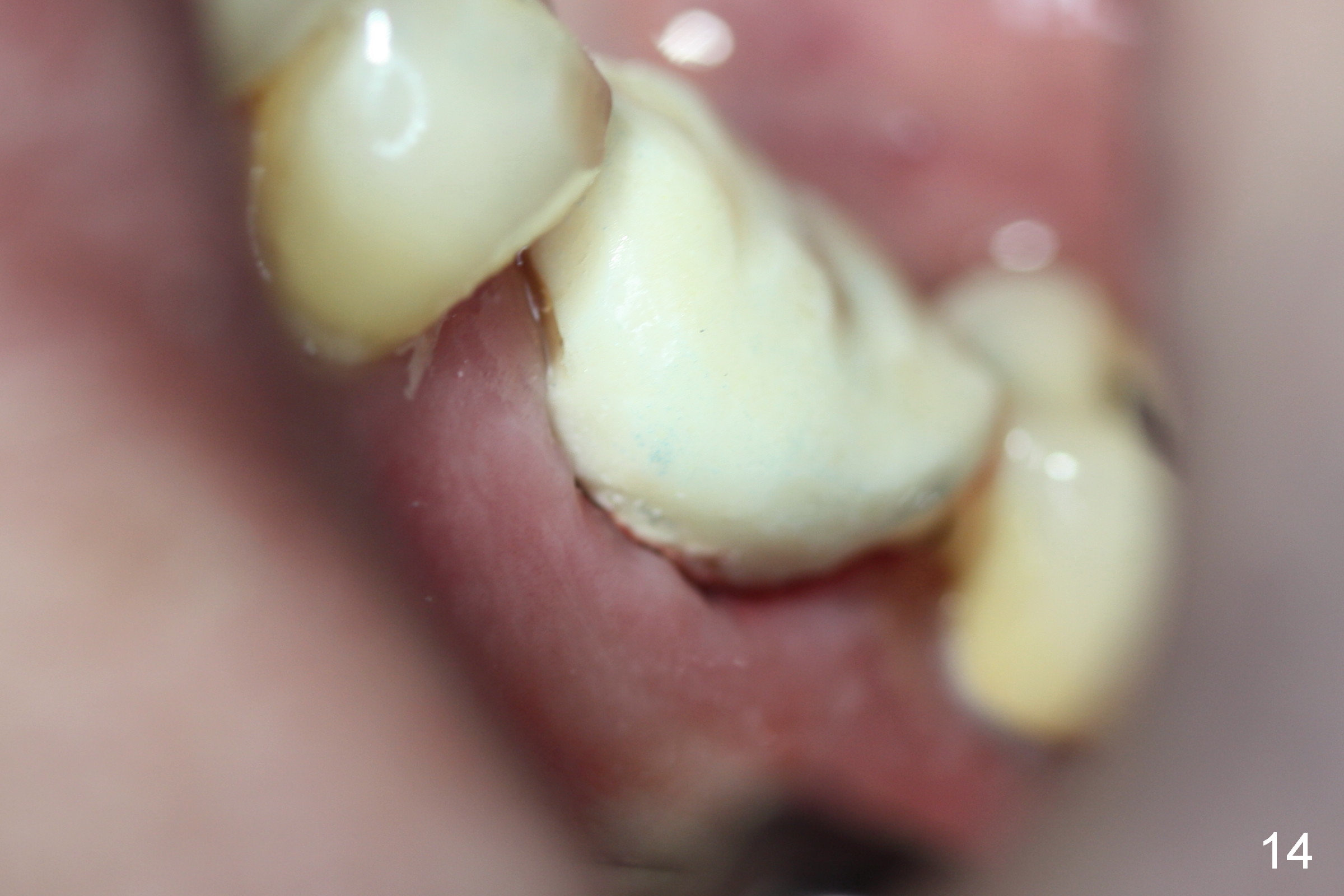
Provisional first, bone graft second may lead to the fact that the provisional may be unable to cover the graft completely. Perio dressing has to be used to cover the remaining gap, as indicated by arrowhead in Fig.12 (residual dressing, 2 months postop). With the loose provisional removed, the socket shows sign of healing (Fig.13, as compared to Fig.10). After the implant/abutment being reprep, the provisional is relined, re-trimmed and recemented (Fig.14).
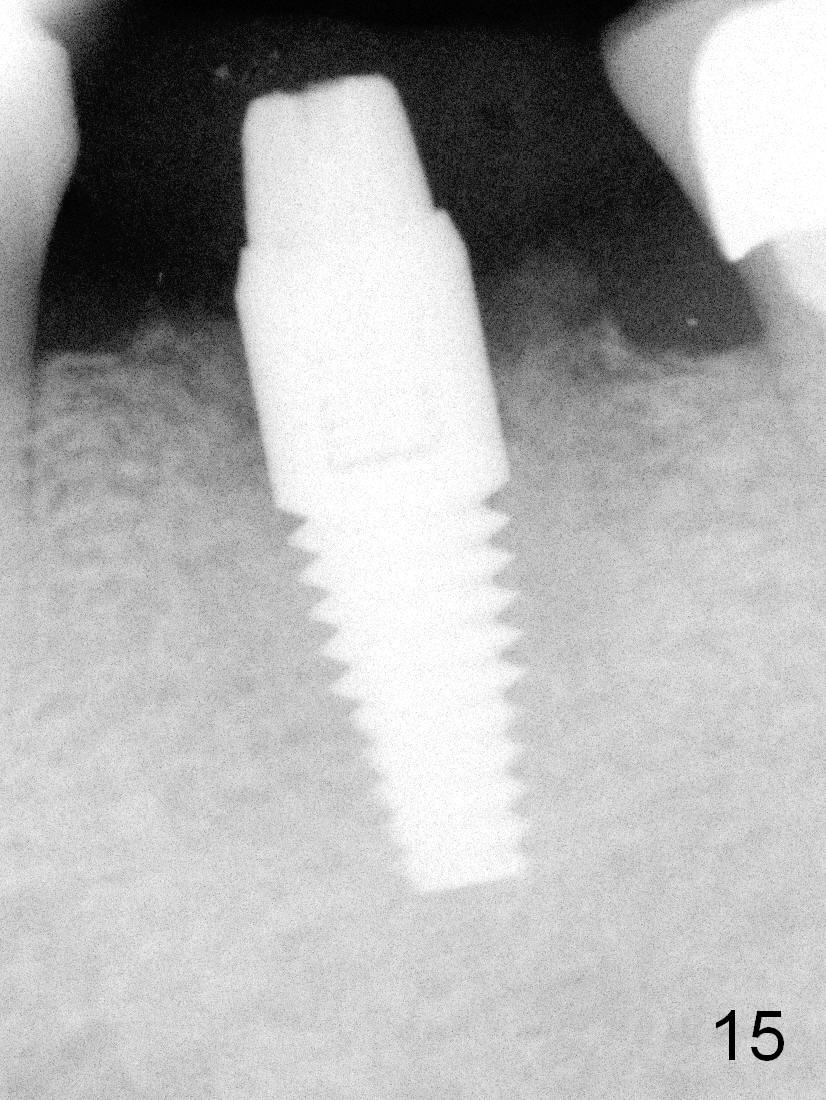
Next visit is less than 5 months postop; there is bone growth in the socket (Fig.15). It appears that the short, small implant can achieve more. It is ready for impression for the definitive restoration.
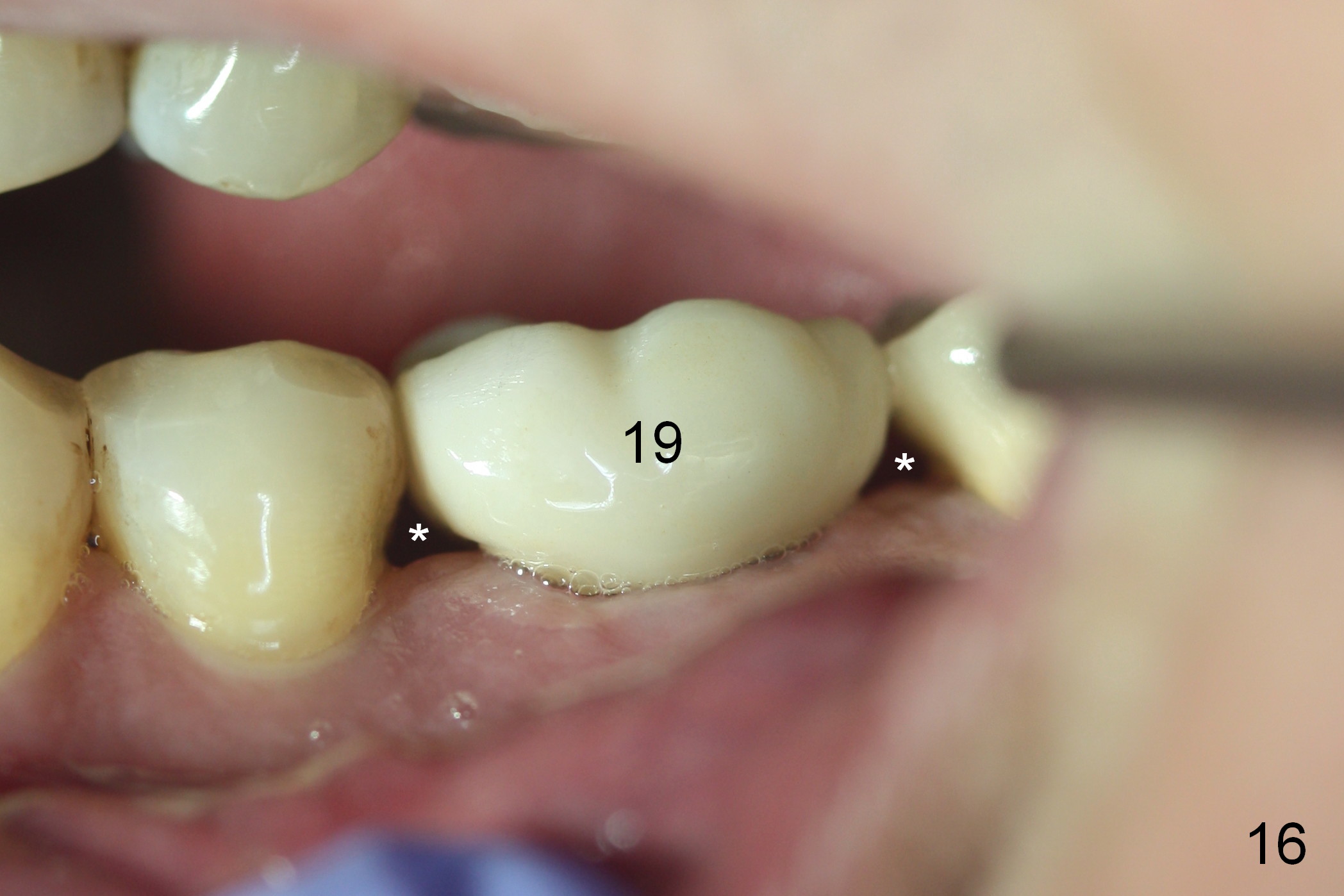
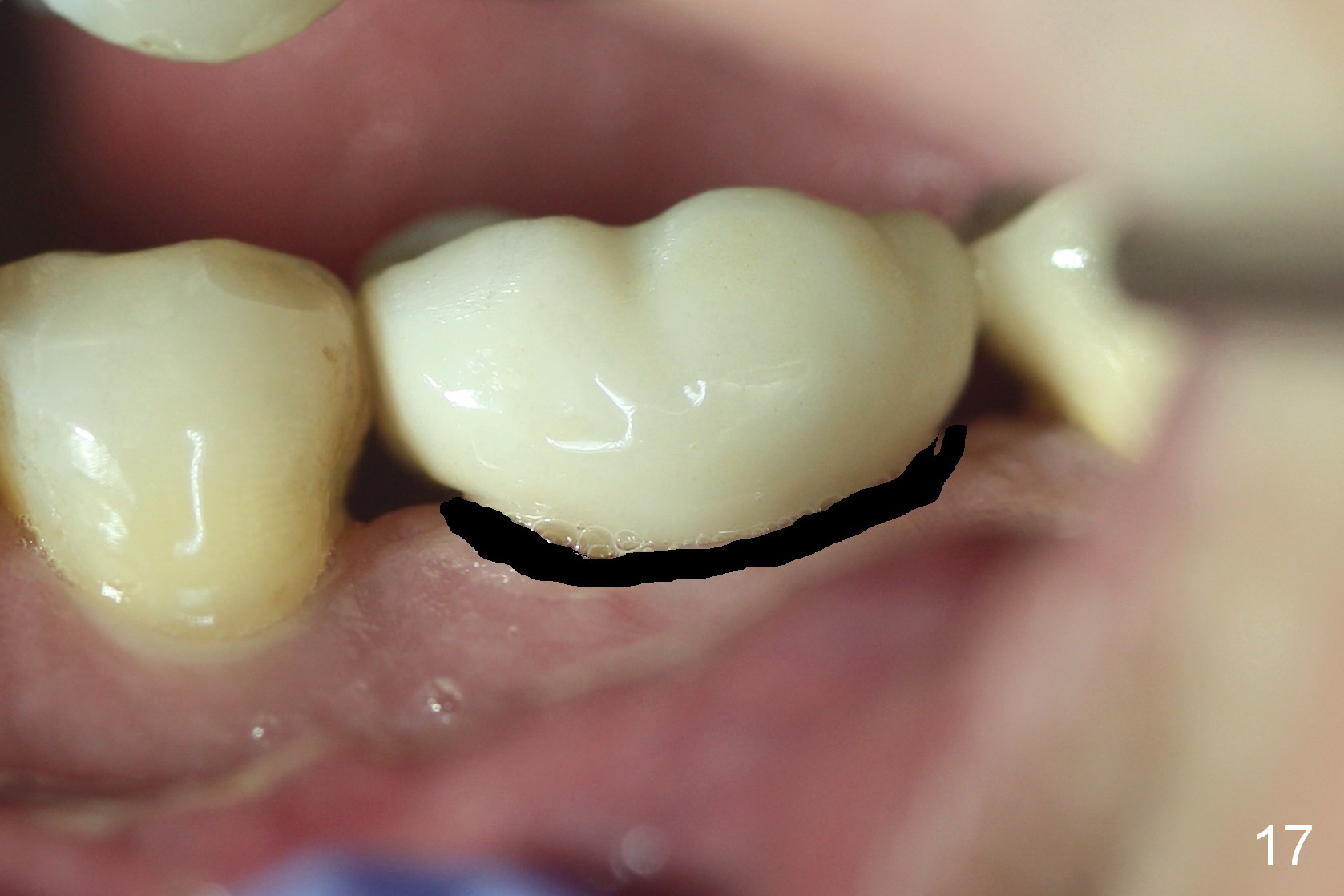
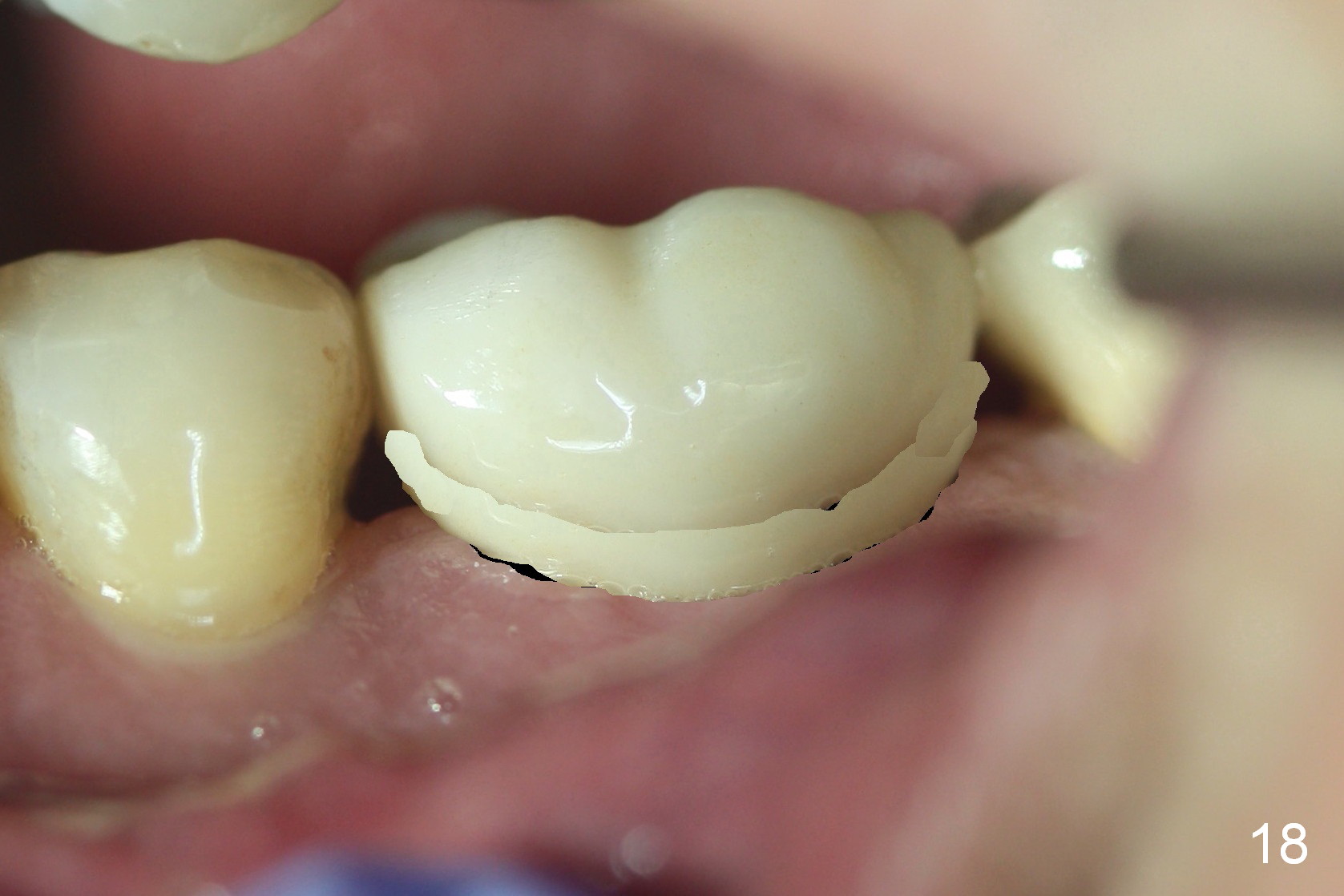
Four months post cementation, the gingival embrasures enlarge (Fig.16 *) with loose mesial contact and food impaction. Before making a new crown, trim the mesial and distal gingiva near the papillae in the model (Fig.17 black area) so that the new crown is a little bulky in the embrasures (Fig.18) to reduce embrasural space. In addition, the contact areas should be tight and wide buccolingually as well as coronocervically. In fact the distal surface of the tooth #20 and the mesial surface of the tooth #18 are trimmed to increase contact areas prior to impression.
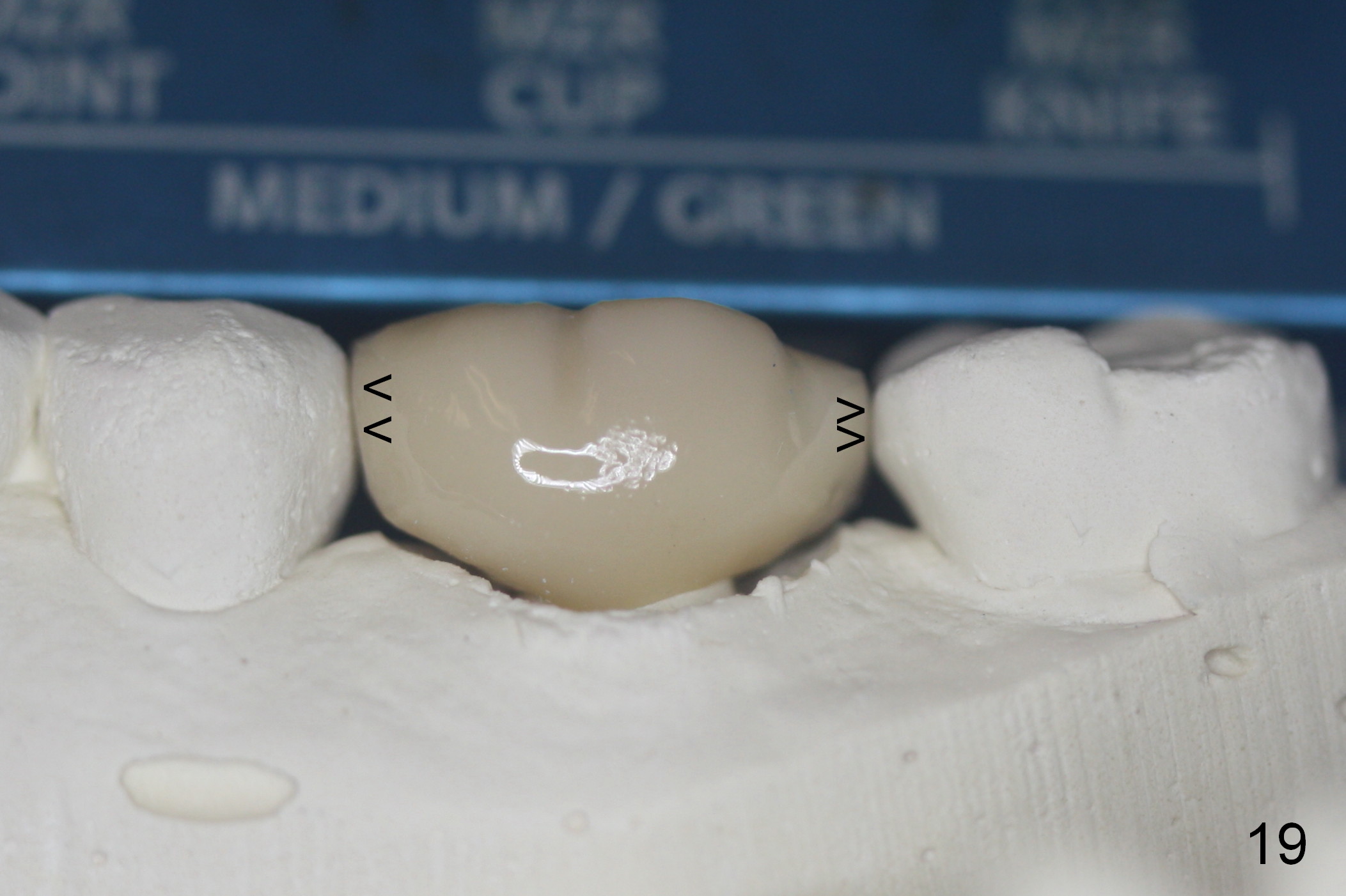
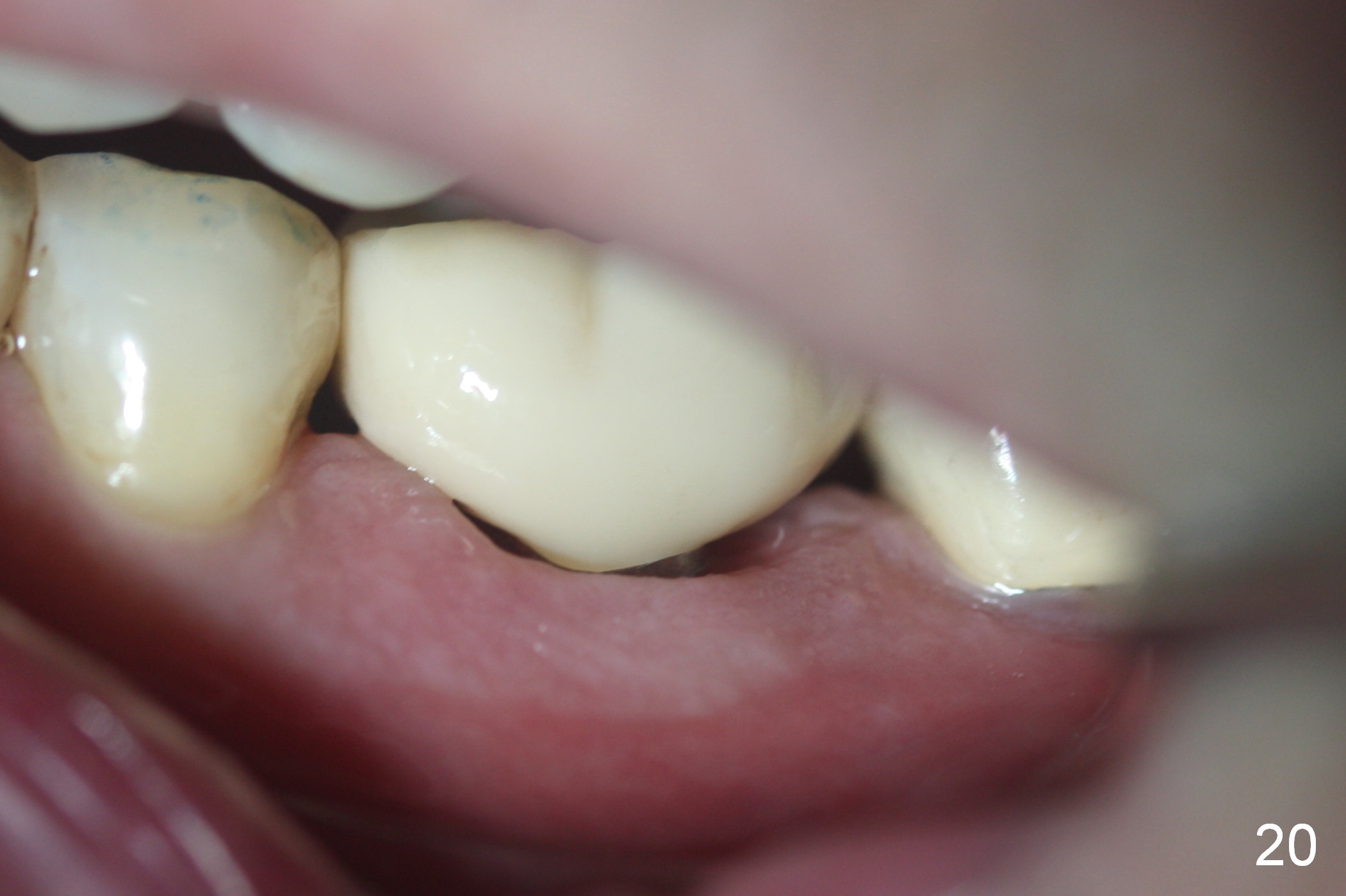
The distal contact area of the redo crown is not as wide as the mesial one (compare arrowheads in Fig.19). Clinically the distal contact is slightly loose. The distal gingival embrasure is also larger than the mesial (Fig.20). There is probability of food impaction distally. Temp bond is used for cementation. Fifteen days later, the crown dislodges and is recemented with a definitive cement.
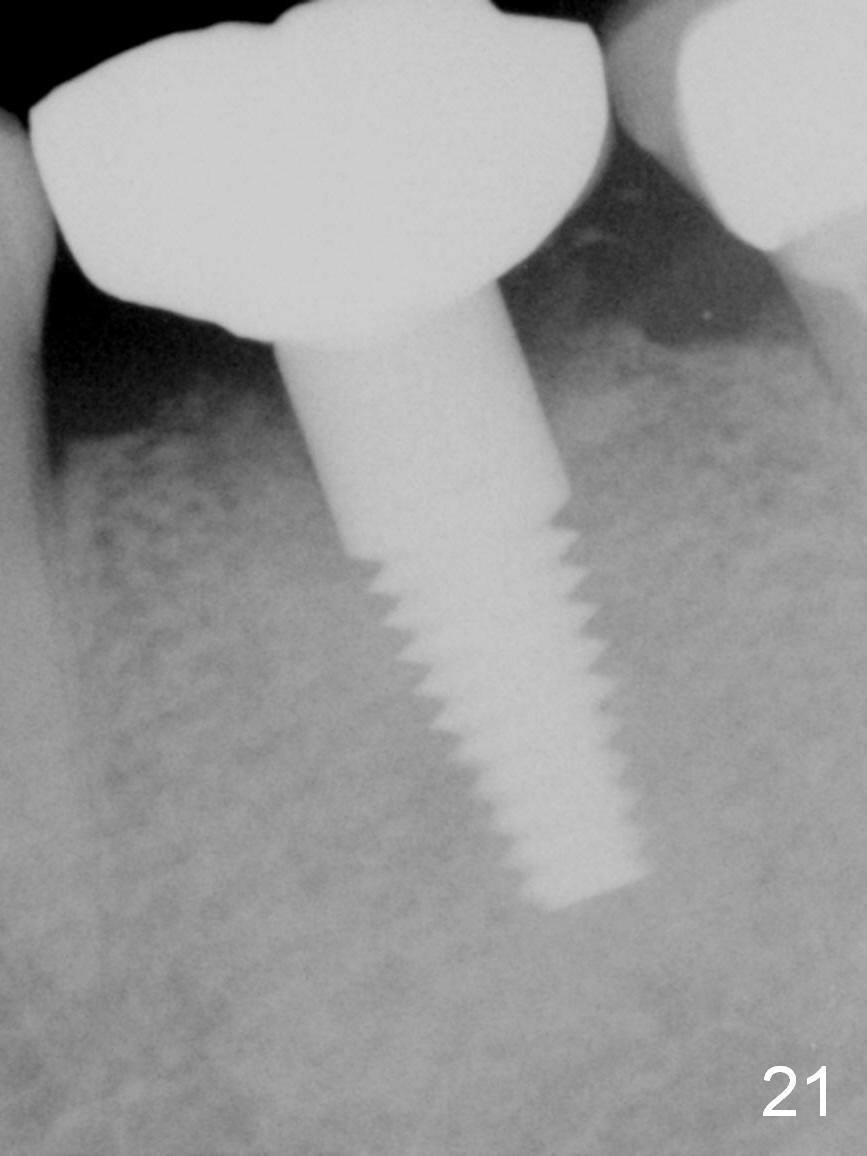
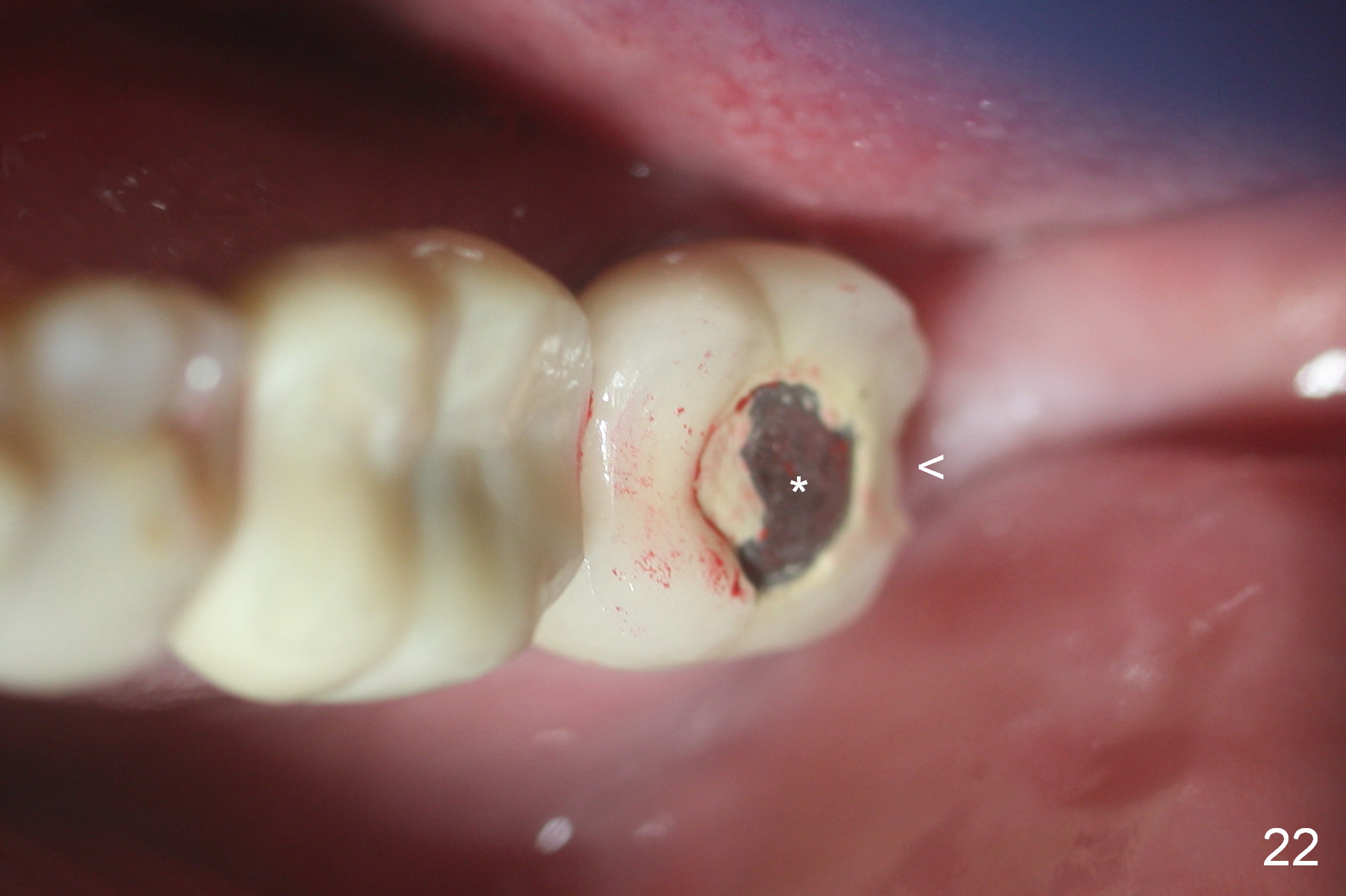
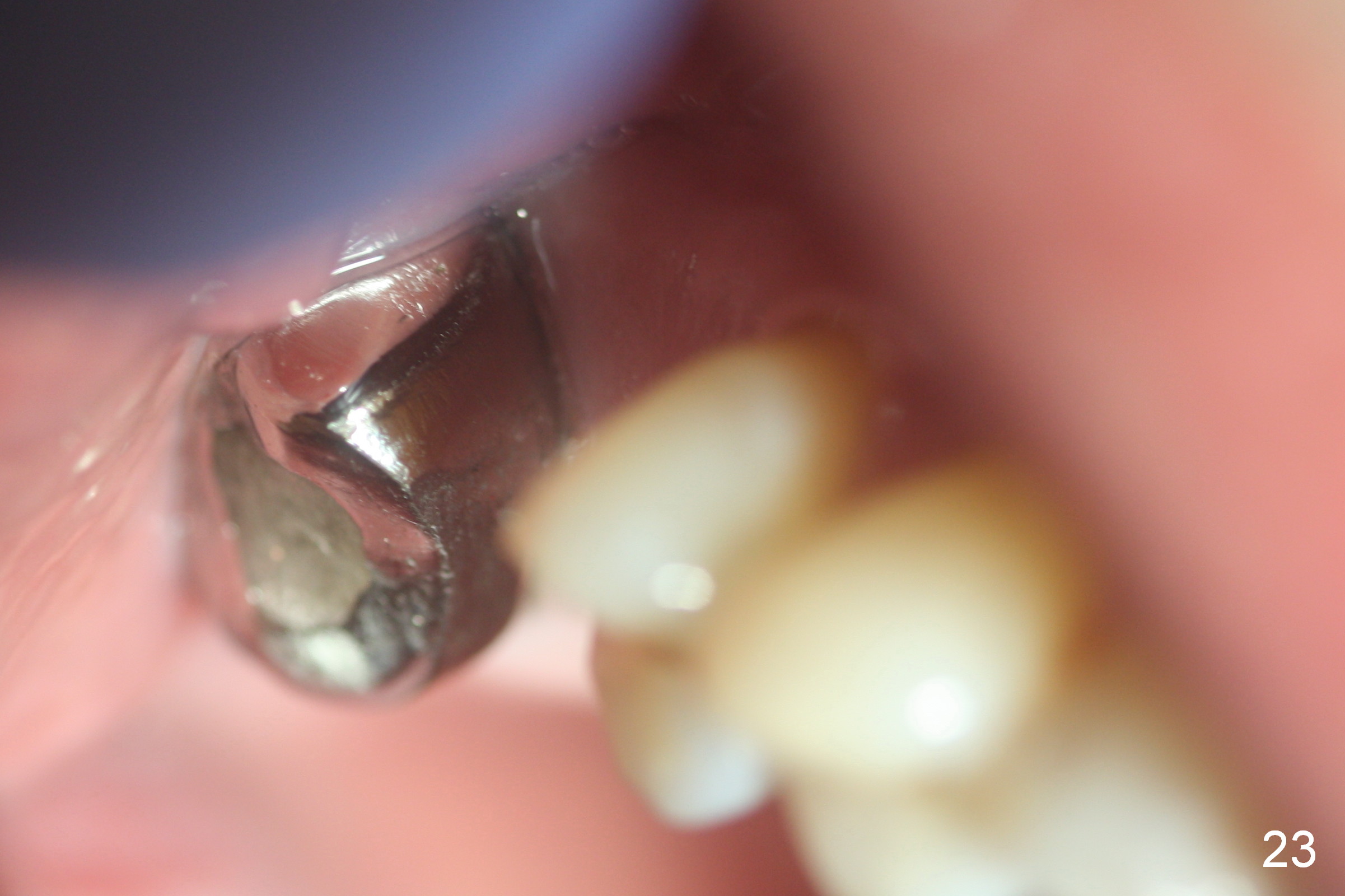
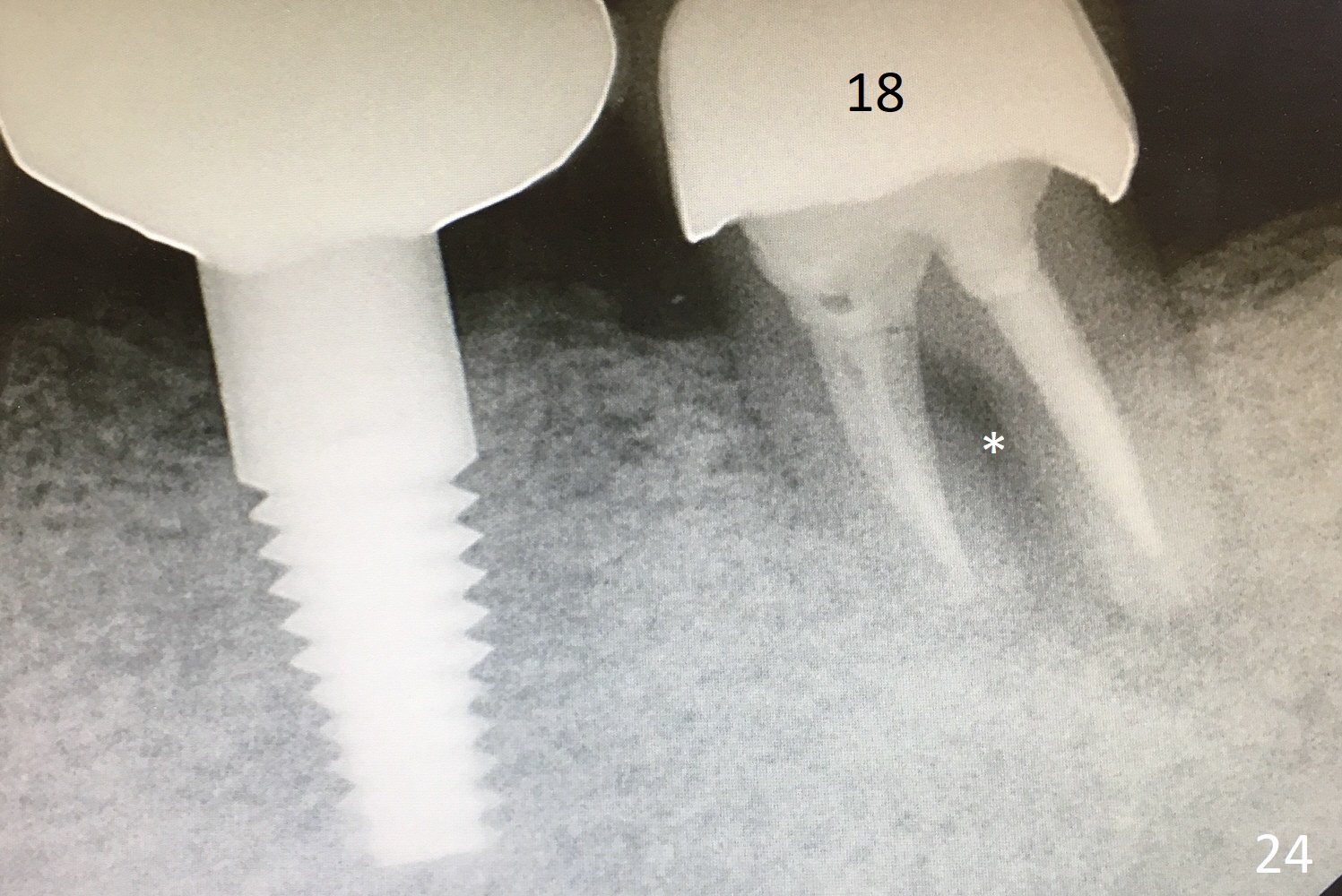
Two months later, the crown dislodges again. The abutment and the crown are cemented with Panavia (resin cement). PA is taken (Fig.21) after initial curing; no residual cement is found. Occlsual adjustment is finished; the patient appears to be a heavy bruxer with porcelain chip at #18 occlusally and distally (Fig.22 *, <). He refuses to have implant placement at #3 (Fig.23). Fifteen months later, the tooth #18 is symptomatic with buccal furca erythema and deep pocket (Fig.24 * bone loss). If the buccal plate loss is so severe that a 6 mm Tatum implant cannot be placed, a SM regular (not narrow) implant is placed with an abutment as large as possible. Take preop PA and make osteotomy in the native bone ~ 3 mm for primary stability.
Return to Lower Molar Immediate Implant,
Posterior Immediate Provisional,
Technicians, Prevent Molar Periimplantitis (Protocols,
Table), Armaments,
Clindamycin,
#3
Xin Wei, DDS, PhD, MS 1st edition 05/17/2015, last revision 06/17/2018